One of the most disturbing things to witness in an animal is a seizure, the most common neurologic problem we see in our hospital. It can traumatize the person witnessing it, and always seems to go on forever.
Unfortunately, it is not uncommon for animals to have seizures, particularly dogs. Fortunately, the overwhelming majority of seizures are not life-threatening, and most dogs can live a relatively normal life. Cats and other species also get seizures, but not as frequently as dogs.
There is a type of seizure status epilepticus that is a medical emergency. These are the pets that go into a seizure and don’t stop seizuring once they start. Or, they go into one seizure, come out of it, and then go back into further seizures on and off.
The Long Beach Animal Hospital, staffed with emergency vets, is available until the evenings 7 days per week to help if your pet is having any problems, especially seizures, shock, pain, difficulty breathing, or bleeding.
Think of us as your Long Beach Animal Emergency Center to help when you need us for everything from minor problems to major a major emergency. We serve all of Los Angeles and Orange county with our Animal Emergency Center Long Beach, and are easily accessible to most everyone in southern California via Pacific Coast Hwy or the 405 freeway.
If you have an emergency that can be taken care of by us at the Animal Emergency Hospital Long Beach always call us first (562-434-9966) before coming. This way our veterinarians can advise you on what to do at home and so that our staff and doctor can prepare for your arrival. To learn more please read our Emergency Services page.
This page will give you a complete explanation as to the cause of these traumatic episodes, and how we diagnose and treat them. The overwhelming majority of dogs that are seizuring have epilepsy, so we will emphasize this disorder when discussing treatment.
What is a seizure?
Use technical words, a seizure is a clinical manifestation of abnormal neuronal activity in the brain. Unfortunately, if a pet has recurrent seizures it might have what is called the “kindling effect” and be predisposed to more and more seizures as more neurons are stimulated. These are the ones that are difficult to treat. One of the ways to minimize this is to start seizure medication as soon as seizures become a problem, and to adjust the medication as needed if your pet is not responding. We talk more about this in the Treatment Section below.
Here are some medical terms we will be using:
| neuron- nerve cell | ictus- an actual seizure |
| idiopathic- unknown cause | postictus- period immediately after a seizure |
| hypoglycemia- low blood glucose (sugar) | status epilepticus- continuous or clusters of seizures |
| hypocalcemia- low blood calcium level | epilepsy- brain disorder characterized by seizures |
| aura- initial manifestation of a seizure | EEG- electroencephalogram |
| syncope- a heart problem that mimics a seizure | Depression- not as alert as usual |
| Dementia- dull or emotionless | Stupor- semi conscious, asleep often, hard to arouse |
| Coma- Unconscious, unable to arouse at all | CSF (cerebrospinal fluid)- normal fluid in the brain and spinal cord |
Normal Anatomy & Physiology
The profound complexity of the brain precludes us from going into significant detail regarding anatomy and physiology. You would need to be a neuroanatomist to even begin to understand its basics. The basic unit of the brain is called a neuron, which is a specialized nerve cell. Some of these nerve cells process information, others cause a reaction. For example, your eyes, which are an extension of your brain, process images. Other neurons cause the muscles in your eyes to move in response to movement.
In all cases, there are millions upon millions of neurons in the brain, all with complex connections to each other. It is these connections that leads to the complexity and the sophistication of the mammalian brain. Unfortunately, when a neuron has a problem, these connections can let this problem spread elsewhere. If an individual neuron has is a seizure, the seizure activity in this one neuron can easily and instantaneously spread to other neurons, leading eventually to a generalized seizure.
As a rough comparison, the mammoth power failure that occurred in the Northeast U.S. in august of 2003 shows how a small problem in one area can rapidly spread to other areas. Multiply all those electrical lines and power stations with their connections by a million times, and you start approaching what occurs every second in the mammalian brain. It is beyond human comprehension to understand the complexity of all of these connections.
Pathophysiology
Seizures (fits, convulsions) are caused by abnormal activity in the brain cells, particularly in the frontal and temporal lobes of the cerebral cortex. When a neurons fires off in a seizure, it sets off a chain reaction in other neurons, and the seizure spreads. If this chain reaction stays within a specific location, a partial seizure might occur. If it spreads to occur on both sides of the cerebral cortex, a generalized seizure, the most common type of seizure, might occur.
Characteristics
-
Aura
Behavior just prior to a seizure. Typical behaviors include panting, pacing, barking, and restlessness. Ranges from several minutes to several hours prior to the actual seizure.
-
Ictus
The actual seizure, characterized by involuntary muscle tone and movement. Lasts from seconds to minutes, although it seems like hours when you are observing it.
-
Postictus
Period immediately after seizure, characterized by disorientation, unusual behavior, appetite change, or weakness. It can last up to several days.
Classification
-
Generalized
This is the most common seizure encountered in dogs and cats. Nerve cells on each side of the cerebral cortex start discharging, causing all parts of the body to be affected. Even though the original source of the seizure is usually only a small number of neurons on one side of the cerebral cortex, the discharge of these neurons causes other neurons to discharge also, eventually causing the seizure to be generalized.
-
Partial (focal)
This seizure also starts as a small number of neurons, yet in this case it does not spread far beyond these initial neurons. Symptoms that are seen depend on which neurons are discharging. It can affect motor areas, causing involuntary movement, or it can affect areas of the brain involved with behavior, causing intermittent behavioral changes. Eventually this type of seizure can progress to a generalized seizure.
This movie is typical of a pet having a partial seizure.
Double Click Here to view the movie
Cause
Idiopathic (epilepsy, primary, genetic, true, inherited)
The word “idiopathic” means that the cause is unknown. It is also known as epilepsy in humanoids. It is a diagnosis of exclusion- if all the other causes of seizure are eliminated, then this is the cause. This is the most common type of seizure, and occurs in up to 2% of all dogs, relatively rare in cats. Any dog breed can be affected, with the larger breeds having more severe seizures. Any breed of dog that has a seizure at 6 years of age or older are in this category. In general, we see it more often in purebred animals. The more common breeds are (the breeds with asterisks are especially problematic and can be difficult to treat:
- Alaskan Malamutes
- Australian Shepherd
- Cocker and Springer spaniels
- Beagles
- Bichon Frise
- Border Collie *
- Chihuahua
- Collies
- Boxers
- Dachshunds
- Dalmations
- German Shepherds *
- Golden and Labrador retrievers
- Irish Setters
- Maltese
- Mastiffs
- Schnauzers
- Poodles
- Pugs
- Saint Bernards
- Siberian Huskies *
- Vizslas
- Yorkshire terrier
In the large breeds seizures tend to be more severe. In the Border Collie and Australian Shepherd there is a severe genetic epilepsy present, and these dogs need to be started on seizure medication when seizures first start.
Secondary
Secondary seizures causing epilepsy occur when there is a structural abnormality in the brain.
Hydrocephalus
This disorder, sometimes know by its more common name of “water on the brain”, occurs in small breed dogs and sometimes cats. It is the excessive accumulation of cerebrospinal fluid (CSF) in the brain. The pressure from the fluid causes the seizures. It is not a problem that is easily corrected, and usually requires lifetime medication. Surgery can be used in select cases, but is not always effective. Pets with severe symptoms early in life have a guarded prognosis.
Common dog breeds that get hydrocephalus:
- Chihuahua
- Yorkshire Terriers
- Maltese
- Pomeranian
- Lhasa apso
- Toy Poodle
- Pug
- Pekingese
- Boston Terrier
The most common symptom with this disorder is behavioral. If seizures occur, they start early in life.
Brain Tumor
We tend to encounter brain tumors in middle aged and older pets. Some arise directly from brain tissue, others spread to the brain via the bloodstream (since the brain has an extensive blood supply). Strangely enough, its not the neurons (brain cells) that become cancerous, it is the cells supporting the neurons, called glial cells, that cause the problem.
Tumors that arise directly from the brain include:
- Astrocytoma
- Oligodendroglioma
Symptoms of brain tumor depend on exactly where in the brain they arise, and how fast they grow.
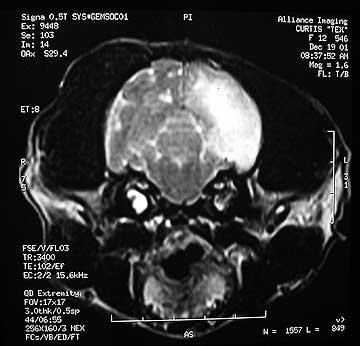
Brain tumors are best diagnosed with an MRI.
Most brain tumors are treated medically- surgery is used only on rare occasion. The progress is poor if your pet has a brain tumor.
Can you see the large tumor in this brain?
Trauma
Pets that have fallen and hit their heads can develop scar tissue in the brain when they heal, leading to seizures later in life.
Stroke
More correctly called “vascular disorders”, they involve damaged blood flow to the brain. The neurons that are normally nourished by these blood vessels can now have a problem.
Viral Disease
Rabies and Distemper are both viral diseases that can cause seizures in dogs.
Reactive Seizures
In this type of seizure the brain is reacting to a problem elsewhere in the body.
- Hypoglycemia (low blood sugar)
- Hypocalcemia (low blood calcium) This video shows an Iguana with twitching muscles caused by hypocalcemia. It is not a seizure. We show it to give an idea of how the bodies neurologic system is affected by hypocalcemia. You can learn more about this Iguana’s problem, which is called Metabolic Bone Disease
- HypothyroidismA low thyroid level, called hypothyroidism, can precipitate seizures.
- Kidney diseaseThe buildup of waste products in the bloodstream, called uremia, can cause seizures. Our Kidney Page has extensive detail on this problem.
- Liver disease – Hepatic encephalopathy, a disorder of blood flow into the liver, can cause seizures. Our Liver Page explains it in much more detail.
- Poisons The vast number of toxins that can cause seizures precludes us from going into detail on each one. One of the most common ones we encounter in our practice is Metaldehyde, also know as snail bait poison. Snail Bait Poison The active ingredient in this product is metaldehyde, a potent drug that will cause seizures in animals. There is no specific antidote- pets need to be sedated to stop the seizures, induced to vomit to rid the stomach of this poison, and even have their stomach flushed if necessary.
After this initial treatment to prevent further absorption of the metaldehyde, we will give your pet intravenous fluids, sedate and even anesthetize it, check a blood panel for damage to internal organs, and monitor its life signs. If a dog that eats snail bait poison is brought to us immediately we can usually help them. This is a short movie of Eddie the morning after he was treated for snail bait poisoning. Notice how unsteady he is (called ataxia) when he lands after jumping up. His seizures are gone but he is still suffering the effects of the poison the next day.
- Other toxins that can cause seizures include:
-
- Lead Poisoning-found in old paint, putty, tile, linoleum, used motor oil, drapery weights, bullets, and fish sinkers
- Organophosphates and Carbamates – found in many different insecticides
- Pyrethrins- found in insecticides
- Strychnine- found in rat poison
- Chocolate
- Ivermectin- found in antiparasiticides
- Mitaban- found in Demodex mange mite treatment
- Caffeine- found in chocolate and NoDoz
- Ethylene Glycol- found in antifreeze
- Fungus
- Some fungi can affect the brain and cause seizures. One of them is called cryptococcus.
- Lead Poisoning-found in old paint, putty, tile, linoleum, used motor oil, drapery weights, bullets, and fish sinkers
This cat was negative for Cryptococcus
Non epileptic Seizures
Syncope
Dogs that have heart disease with an abnormal heart beat (called an arrhythmia), can pass out in a manner that looks just like a seizure. Sometimes syncope can be difficult to differentiate from a seizure. In syncope, a dog does not usually exhibit the motor activity (paddling) or urination/defecation symptoms seen in a seizure. This is one of the may reasons we follow a rigorous approach to the diagnosis of any disease.
Seizures in Cats
Cats have seizures much less commonly than dogs, and they don’t seem to have generalized seizures as often. Seizure symptoms that might occur in cats include:
- Facial twitching
- Salivation
- Attacking invisible objects (although this can be normal behavior in some cats)
- Running frantacially as if something unknown is chasing them
- Colliding with objects (also ban be a normal behavior)
Secondary epilepsy tends to be more common in cats. In addition to the causes in dogs, common causes in cats might also include:
- Thiamine deficiency
- FIP (Feline Infectious Peritonitis)
- FIV (Feline Immunodeficiency virus)
- FeLV (Feline Leukemia virus)
- Toxoplasmosis and Roundworms
- Feline Hyperesthesia Syndrome
- Food allergy
Depending on the cause, they are treated in a similar fashion.
In both dogs and cats we also classify seizures as to their cause when making a diagnosis. Those that occur directly in the brain are called intracranial. Examples include brain tumors, CNS infections and inflammations. Those that occur primarily outside the brain are called extracranial. Examples include hypocalcemia and hypoglycemia
Symptoms
Seizures commonly start while your pet is sleeping. Typical symptoms in a severe, or grand mal seizure, include: Falling
- Loss of Consciousness
- Extension of the limbs
- Paddling of the limbs
- Chomping at the jaws
- Dilated pupils
- Excess salivation
- Defecation
- Urination
Behavior changes during a milder seizure include:
- Fear
- Hysteria
- Aggression
- Barking or meowing
- Hiding or cowering
In milder seizures your pet might remain conscious, and appear anxious or walk like it is drunk. Even though people like to compare this to “petit mal” seizures in people, it is not the same thing. Milder seizures might last for a few minutes, or could go on for hours, maybe even leading to a generalized seizure.
Pets appear to have an aura (preictal) prior to a seizure. They might be restless, seek attention, try to hide, whine, or tremble. After their seizure (postictal) they might show similar symptoms, even blindness, aggression, or sleepiness. The postictal stage lasts a variable period of time, up to hours after the seizure.
Diagnosis of seizures in dogs and cats
In most cases, by the time we examine a pet that has seizures, the seizures are no longer present. It is important to follow the tenets of the diagnostic process closely when making a diagnosis of seizures, especially since the syncope that occurs with heart disease mimics a seizure. A large part of the diagnosis in this disease is based on history, which you learned about when your linked to thediagnostic process page.
Signalment
Idiopathic seizures occur in any age dog or cat, particularly the breeds previously mentioned. Usually a dog with idiopathic epilepsy is between 1-3 years of age. Dogs not in this age range have a greater potential for secondary seizures as their cause.
History
Exposure to toxins, a prior history of head trauma, or concurrent diseases like liver and kidney disease, give us a clue to seizures and their cause. It is important to differentiate syncope from seizure, since some cases of syncope can look like your pet is having a seizure. If we suspect syncope we will perform tests to analyze the heart and lungs. You will find these tests in our heart page.
Physical Exam
In most cases the physical exam is normal. This is because most seizures are caused by idiopathic epilepsy. If your dog has a seizures caused by a brain tumor or infection/inflammation in the central nervous system (CNS), we might see neurologic signs like uneven pupils.

This is a picture of an adult dog with diseased teeth, which might be an indication of Distemper when it was younger

In some cases of Distemper the pads might be thickened
As part of the physical exam on of our doctors might feel a need for a more detailed neurologic exam. Things that might be checked are:
- Mental status – alert, depressed, unresponsive to stimuli, comatose, circling, head pressing, behavior change and disorientation
- Cranial Nerves – menace response, pupillary light reflex (PLR), eyeball deviations (strabismus, nystagmus), oculocephalic reflex
- Postural reflexes – conscious proprioceptive (CP), tremors, gait, extensor thrust, and wheelbarrowing
- Spinal reflexes – pelvic limb (patellar reflex and perineal reflex), thoracic limb triceps reflex and biceps reflex)
- Muscle – mass and tone
- Pain and tactile reflexes – deep pain and light touch reflexes
- Cutaneous trunci reflex
- Tail tone
Diagnostic Tests
A Blood Panel and Urinalysis might give us a clue as to the secondary or extracranial cause of seizures. Careful interpretation is needed. If a dog has a low blood sugar (hypoglycemia) on the blood panel, it might be because the seizure activity has depleted its stores of glucose, not because it has hypoglycemia. This is why sometimes its a good idea to perform the exam well after a seizure has occurred, and the body has a chance to get back to normal.
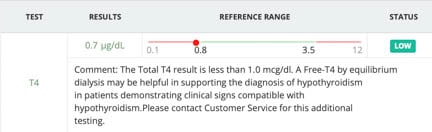
Our routine blood panel also includes a thyroid check to make sure the level is not too low, which can precipitate a seizure.
This one came back as 0.7, so it is marginally low and needs to be investigated further if a dog or cat is having seizure. Our hypothyroid page has much more information.
Radiographs
Radiographs of the head of dogs and cats are complex compared to humanoids. There is a much smaller brain to view, the bones are more massive and overlapping, and there is great degree of variation among breeds. They can be used to diagnose hydrocephalus, trauma, or cancer, although they can’t be relied upon in most cases.
If we radiograph the hey can help us identify a secondary cause of seizures like an enlarged liver or kidney. We can sometimes see cancer on a radiograph as it has spread from its primary location to other parts of the body, particularly the lungs and lymph nodes. We might note fluid in the abdomen (ascites), an indication that a cat has FIP.
CSF Pressure
When a pet has a brain tumor there will be increased pressure within the central nervous system (CNS). This increased pressure, when it occurs, is measure by performing a spinal tap, and measuring the pressure with a manometer. Fluid that is obtained this way (called cerebrospinal fluid) can also be analyzed for inflammation and infection by our pathologist. This is how we diagnosis meningitis and encephalitis.
MRI
One of the most accurate and efficient ways to diagnoses the cause of a seizure, especially if there is a brain tumor, is Magnetic Resonance Imaging (MRI). It is also used to diagnose hydrocephalus, and blood vessel problems in the brain. If you double click on the picture below you will view a series of “slices” of the brain. The first picture shows a side view of a dog’s brain, and gives you an idea of the “slices” as the pictures continue on through the brain. This dog’s nose is on the far left. In slices 6-10 it will be obvious there is a problem when you see the large white mass in the middle of the brain – that is a tumor.
Click here to view a movie on MRI sequence
Treatment
The ultimate goal of treatment is to eliminate all seizures, which would be rare to do. In most cases we are able to reduce the seizures substantially and get them to what is an acceptable level.
In most cases by the time you can bring your dog to us for treatment the seizure has subsided. If your pet experiences a seizure, move any furniture out of the way, move things like lamps that might fall, remove other pets from the area, make sure it cannot fall down any stairs, and let the seizure run its course. Most will run their course within 1-2 minutes. Do not put your hands in your pets mouth to prevent it from swallowing its tongue- all that will do is get you bitten severely. If your pet turns blue during a seizure it is because its muscles of respiration (ribs, diaphragm) are locked, and it is not breathing temporarily. This problem will resolve itself, unless the rare occurrence of status epilepticus is present. Have a crate or airline carrier present to bring your dog to your veterinarian.
One rare but serious type of seizure is called status epilepticus, where the seizure lasts more than 5 minutes, it doesn’t stop at all , or it stops but returns soon after. This is a medical emergency, and requires the use of injectable medication, and even general anesthesia, to prevent it from progressing to a life threatening problem. If your dog is experiencing this problem call us immediately. If we are not available for some reason, you should have information at hand for a 24 hour emergency hospital close to you that will take care of you.
Idiopathic
Idiopathic epilepsy cannot be cured, only controlled, and once treatment is started, it is lifelong. Most dogs and cats respond well to anticonvulsant medication give orally.
Deciding when to treat idiopathic epilepsy is just as important as how to treat. Some dogs only have 1 or 2 seizures per year, and don’t require treatment. Some dogs have seizures weekly or daily, and require treatment. Other dogs can be in the gray zone. They might have a seizure every 1-4 months, so making a determination to treat them is not so clear cut.
If these dogs with infrequent seizures start having them more frequently, then we recommend anticonvulsant medication. As a general guideline, if your dog as 2 or more seizures in a 6 month period we should start an anti-convulsant therapy. The sooner we start on these dogs the better the long term outcome.
In some breeds the seizures will increase in severity, so it is wise to treat when seizures first appear and try to prevent this problem. This applies to Border Collie’s and Australian Shepherds. In these breeds more than one seizure medication needs to be started earlier in the course of disease if the first medication does not work well.
Every dog is different, and what works in one dog might not work in another. Doses sometimes need to be adjusted, and even combination therapy with several different medications might be needed to control the seizures.We don’t start a second seizure medication until we are sure the first medication is at optimum therapeutic levels with a blood panel.
These medications will take several days to take affect, so a seizure during that time might occur. Never abruptly discontinue them. Our goal is to balance seizure control with quality of life, using minimal medication. In most cases of idiopathic epilepsy we are able to achieve this goal, at least initially. Some dogs with epilepsy do not respond to medication.
Monitoring serum levels of anti seizure medications is important for the following reasons:
Determine effective drug concentrations after we have started treatment
Determine if a drug failure is due to a low level of the drug in the blood stream (inadequate dose), or if it is due to a drug that is not working, no matter what the dose.
Determine if treatment failure is caused by poor compliance
Prevent toxic effects if level is too high
Allows individual treatment
Phenobarbitol
One of the most common and effective medications for epilepsy is phenobarbitol, given twice to three times daily. Phenobarbitol has been around for a long time, so the price makes it the most cost effective anti seizure medication.
The overwhelming majority of dogs are maintained at twice daily dosing in our hospital. It takes several weeks for the blood level of phenobarbitol to reach adequate levels, so there might be an occasional seizure during that time. Phenobarbitol works in the majority of dogs, is inexpensive, and safe, so it is widely used.
The dose of this drug has a wide range, so if your dog is not responding to phenobarbitol, and the blood level of the drug is low to normal, we might increase the dose. Doses are changed gradually since it takes time for the effects of this drug to become apparent. An injectable version of this drug given intravenously (IV) to stop status epilepticus.
Never give your dog oral phenobarbitol if it is experiencing status epilepticus as described above- it needs to be seen by a veterinarian immediately. Never put your hands in the mouth of a dog having a seizure because you believe it is swallowing it’s tongue because it is turning blue. It is not swallowing it’s tongue, and all you will end up doing is getting injured.
Some dogs will be sedated initially, but may eventually return to normal activity. Other dogs might drink and urinate more than usual, and have an increased appetite, so go on a diet that will not cause an increase in weight and lead to other problems related to obesity. In rare cases the liver will become toxic due to this drug. This is why we check a full blood panel every 6 months while your pet is on this medication.
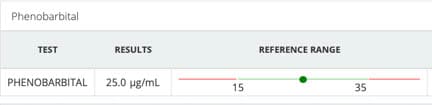
Phenobarbitol levels can be measured in the bloodstream, and are an important guide to proper dose of this drug. This will make sure we are at adequate levels in the bloodstream. One of the reasons a dog might continue to have seizures while on phenobarbital is an inadequate blood level. In this case we adjust the dose. If the blood level of phenobarbital is adequate and your pet is having seizures frequently it might be time to add another medication to the phenobarbital.
This dog is right in the middle of the normal range
We recommend performing the phenobarbitol check every few weeks to months for the first few months of therapy in order to get an idea of how your pet reacts to the medication. The phenobarbitol level is interpreted in conjunction with the amount of seizures that is occurring. All adequately controlled dogs on long term phenobarbitol should have an exam, blood panel with urinalysis, and phenobarbitol level checked every 6 months at least. Dogs can become refractory to phenobarbitol, so it is imperative you give the medication as prescribed and monitor carefully so we can decide the best course of action in this case. It is not uncommon to have to increase the dose in some dogs.
When giving this medication on a twice daily basis it is important for busy households to give the medication as directed. Using a dedicated calendar to help you know when the next dose is due, along with monitoring seizure activity, is the best way to prevent inadequate dosing, especially when several people are involved with treatment. It is not unusual for dogs to spit out the pill on occasion, so always verify it went down the hatch. If you have trouble at any time giving this medication our nurses will assist you. They can review proper administration techniques, and will even give the medication for you in our hospital if necessary.
If your dog has gone over 1 year without a seizure me might slowly lower the medication over several months, and even stop it completely on a trial basis. This does not apply to every breed of dog.
Imepitoin
This is another good first time treatment like phenobarbital. It is not easily monitored with a blood test to see if it is at a propper theraeutic level in dogs.
Keppra (levetiracetam)
This anti-seizure medication is used commonly as an additional drug given simultaneously when the first drug was not effective. It does not do as well when given by itself in the dog or cat. It has to be given at least 2x per day, and sometimes 3X per day to stop seizures, so that can be problematic.
Potassium Bromide
If a dog is on phenobarbitol, and it is not adequately controlling seizures, even as we increase the dose, we will sometimes add this drug to the treatment regimen instead of Keppra. It can sometimes take several months for this drug to achieve enough potency in the bloodstream to prevent seizures.
Whenever we have a dog on both medications we start dosing conservatively, and make changes gradually so the body has time to adjust.
It is also monitored with a blood sample periodically in a similar fashion to phenobarbitol.
Side effects can be similar to phenobarbitol, and also include an unsteady gait and inflamed pancreas (called pancreatitis). Liver toxicity to this drug is not usually a problem, so we can use it in cases where phenobarbitol is working but might be affecting the liver. Give it with a meal to prevent an upset stomach, and don’t change your dogs diet abruptly because salt in the diet influences how potassium bromide is absorbed.
It does not work well in cats and can even cause serious side effects, so we do not use it in cats.
Valium
Valium is given intravenously (IV) to dogs with status epilepticus. It is usually the drug of choice in status epilepticus because it is so effective. We might also give you a valium solution, to be given via rectum if your dog starts the continual seizure seen in status epilepticus. This gives you an effective treatment at home if this occurs, although if it does not work you need to seek medical care immediately.
We don’t use Valium in cats because it can cause a liver problem.
Injectable valium is our first line of treatment if your dog or cat is in status epilepticus
Alternative Treatments
- Vagal nerve stimulation, in 2 small studies, showed a significant (34%) decrease in seizure frequency in a population of 10 dogs.
- Ketogenic diets are not effective, and might even cause pancreatitis.
- MCT diets, which are medium chain triglyceride diets used for Cognitive Dysfunction Syndrome, have been shown to be effective in some dogs. The food here is Hill’s B/D (Brain Diet).
- Omega 3 fatty acid supplementation is not effective.
- Acupuncture- Not enough data is available in dogs. When data for humans is analyzed acupuncture is found to be of no value.
- With the recent relaxing of marijuana (cannabis) laws in several states we might be able to find out if CBD works in a bona fide study. Ongoing studies are being performed to make sure it works and also to make sure it does not cause any harm.
Alternative Medications
Since seizures have been around for many years, well intentioned people have postulated many treatment regimens that range from high doses of vitamins to herbal treatments, all in the name of being better than drugs because thely are “natural”. These claims are yet to be proven, and until proper clinical trials are performed, these claims have no basis in fact, and are just a repeat of anecdotal evidence that has been around so long and repeated in print so often that it has become fact.
Many of these “natural” remedies are drugs themselves, drugs in which no studies have been performed to see if they work and to make sure there are no toxic effects. Herbal treatments contain drugs, and just because they are natural does not mean they are not toxic.
Several drugs used in humanoid medicine are being investigated for use in the dog. We might use them if the standard medications are not working, although they are too new to know for sure how they react in the dog or cat.They have the ptential to be more toxic than the use of phenobarbitol and valium.
Long Term Plan
Everything regarding your pets seizures she be noted on a calendar. It will help us look for trends, and let us know if the medication is working. You should also note the dates your pet needs to return for an exam or blood sample.
Never discontinue medications just because your pet has not had a seizure in a while.