Growing old is a natural process and a fact of life, for all of us, including our four-legged dog and cat family members. This is especially prevalent in dogs and cats since they age faster than us humanoids. Family members will probably be the first to notice the subtle changes of Canine Cognitive Dysfunction Syndrome or CDS. It may be more than just “getting old.”
There is a Prescription Diet food made by Hills that is used to treat this problem. You will learn more about it later in this page.
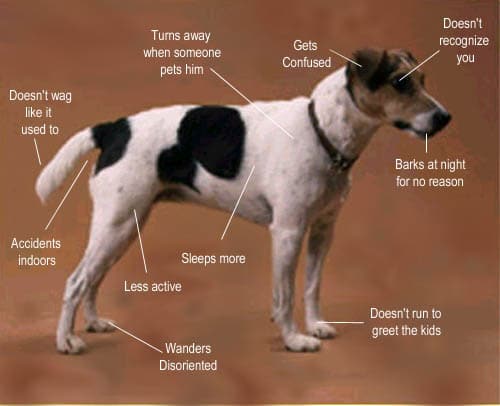
Dogs with CDS may show signs of confusion, forgetfulness, less responsiveness, and/or other various behavioral changes that are not a normal part of aging. They are similar to dementia and senility in older people. These subtle signs might not be exhibited in the examination room so we may not see them during an examination.
A common problem we encounter is an owner thinking their canine is getting old as it slows down and does not go as far and as fast on walks anymore. These dogs more often have arthritis than CDS, and this arthritis is treatable. Please read our Arthritis Page to learn more.
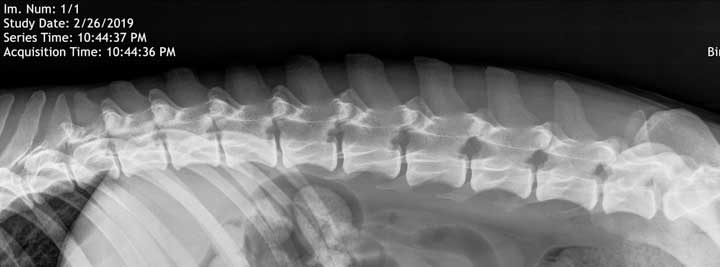
This is a digital radiograph of a normal canine lower spine
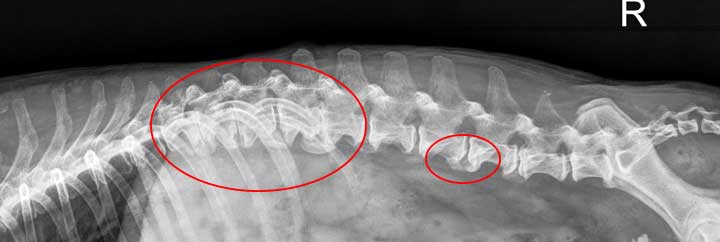
The painful arthritic areas are circled in this dog with arthritis of the spine called spondylosis
Cause
CDS is believed to be caused by physiological and chemical changes in the brain of aging dogs that affect brain function. These may include accumulation of B-amyloid, declining neurotransmitter activities, or increased activity of monoamine oxidase-B, an enzyme that may catalyze the metabolism of dopamine.1
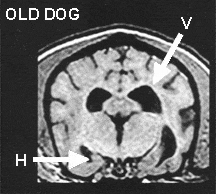
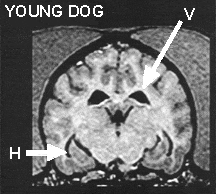
In MRI (Magnetic Resonance Imaging) studies of the head, images show black and white cross-section “slices” of the brain. In MRI studies of older dogs with CDS, we see changes when compared to MRI studies of younger dogs. In the images below, note the ventricular space enlargement (V arrows) and hippocampus tissue shrinkage (H arrows) seen in the older dog image on the left, compared to the younger dog image on the right.1
Symptoms
| Disorientation (not due to vision or hearing loss) |
Wanders aimlessly Appears lost or confused in familiar surroundings such as the house or yard Gets “stuck” in corners or under or behind furniture Stares into space or at walls Has difficulty finding the door Stands at the wrong door to go outside Stands at the “hinge” (wrong) side of the door Does not recognize familiar people Does not respond to verbal cues or their name Appears to forget the reason for going outside |
| Activity and Sleep | Sleeps more in a 24-hour day (overall) Sleeps less during the night Decrease in purposeful activity in a 24-hour day Increase in aimless activity (such as wandering, and pacing) in a 24-hour day |
| Housetraining (for dogs previously housetrained) | Has “accidents” (urinates or defecates) indoors Has “accidents” indoors in view of family members Has “accidents” indoors soon after being outside Signals less to go outside (for dogs who previously signaled/asked to go outside) |
| Interaction with Family Members | Solicits attention less Less likely to stand/lie for petting (walks away) Less enthusiasm upon greeting No longer greets family members (once the dog has realized that family members have arrived) |
Diagnosis
Since a biopsy of the brain is not usually a diagnostic option, a presumptive diagnosis can be made when there are clinical signs consistent with CDS and the absence of any underlying medical causes.
For a suspected case of CDS, as for any behavior problem, a history, physical examination, and diagnostic tests are needed to rule out the presence of any medical conditions that might affect behavior. These might include diseases of the internal organs, especially liver, kidney, and heart.
Additionally, primary and secondary behavioral problems need to be ruled out such as separation anxiety, noise phobias, or housesoiling.
Medical Conditions with Behavioral Components:
| Medical condition | Associated clinical signs |
Sensory dysfunction(loss of sight, hearing, smell) |
Increased irritability, fear or aggression Decreased appetite Increased vocalization Changes in sleep-wake cycle Disorientation Decrease in greeting behavior Inattentive, decreased responsiveness to verbal commands |
Urinary tract disease
|
Incontinence, loss of housetraining polyuria (urinating more) polyphagia (eating more) stranguria (painful urination, straining to urinate) pollakiuria (urinating more frequently) |
Osteoarthritis |
Weakness, reduced mobility and activity Increased pain, irritability Possibly inappropriate elimination |
Hypothyroidism |
Decrease in activity Increased irritability or aggression Reduced tolerance to cold |
Hyperadrenocorticism
|
Polyphagia (eating more), polyuria (urinating more), restlessness Decreased social interaction, responsiveness to commands and greeting behavior Reduced activity Loss of housetraining Disrupted sleep-wake patterns |
Neurological disorders(primary or secondary |
Changes in sleep patterns, eating habits, housetraining, aggression, docility |
To obtain a complete medical and behavioral history, we may ask many questions because signs of CDS may be subtle and not be exhibited in the examination room during during an examination. A printable Senior Dog Behavior History Form to aid in diagnosis of CDS is available by clicking here.
We will perform a thorough physical examination. In addition, a brief neurological examination will include assessment of cranial nerves, evaluation of postural reactions, especially conscious proprioception, and evaluation of the perineal reflex to assess sphincter function.
Typical diagnostic tests would include a serum chemistry profile, complete blood count (CBC), and urinalysis. Additional tests may be warranted based on the patient’s history and physical examination results.
Treatment
The best treatment for this problem is a food from Hill’s called b/d. It stands for brain diet.
An occasional dog have severe symptoms of CDS and fall down the stairs or have a similar type of accident. If you suspect your dog has this disease it needs to be watched closely for a serious injury. The Long Beach Animal Hospital, staffed with emergency vets, is available until the evenings 7 days per week to help if your pet is having any problems, especially any injury related to CDS like a fracture of the bones or a concussion.
Think of us as your Long Beach Animal Emergency Center to help when you need us for everything from minor problems to major a major emergency. We serve all of Los Angeles and Orange county with our Animal Emergency Center Long Beach, and are easily accessible to most everyone in southern California via Pacific Coast Hwy or the 405 freeway.
If you have an emergency that can be taken care of by us at the Animal Emergency Hospital Long Beach always call us first (562-434-9966) before coming. This way our veterinarians can advise you on what to do at home and so that our staff and doctor can prepare for your arrival. To learn more please read our Emergency Services page.
Return to Canine Diseases Page.
Additional Reading:
1. Cognitive Dysfunction Syndrome and Other Geriatric Behavior Problems; CE Advisor a supplement to Veterinary Medicine, Feb 1999.[view PDF format].
2. Controlling CDS with Anipryl®: Post Approval Field Research Results from Private Hospitals in the US; Pfizer Animal Health Technical Bulletin, Dec 2000. [view PDF format]
You will need the Adobe Acrobat Reader to view and print the bulletins and forms, which are in PDF format. If you already have Acrobat® Reader, you can immediately download and print the documents. If you need a copy of the Adobe® Acrobat® Reader®, click the icon below to download it free of charge from Adobe®.
References:
- Adding New Science to the Practice of Medicine – Senior Dog Health, canine Cognitive Dysfunction Syndrome and anipryl® Senior Health Care advisor Program, Pfizer animal Health
- Campbell, S; Controlling CDS with anipryl®: Post approval Field Research Results from Private Hospitals in the US; Pfizer animal Health Technical Bulletin, Dec 2000.
Developed for Long Beach Animal Hospital, by Glenna M Gobar DVM, MPVM, MS, courtesy of Pfizer Animal Health; Sept 2001