This page explains the more common heart diseases encountered in dogs and cats, along with how they are treated. We will cover the following seven topics:
- Chronic valve disease
- Cardiomyopathy
- Heartworm
- Aortic Stenosis
- Pulmonic Stenosis
- PDA (Patent Ductus Arteriosis)
- Medical Treatment of Heart Disease
Before you read about these diseases you might want to review some of the diagnostic tests we used to diagnose heart disease at our Heart Disease Diagnostics Page.
Chronic Atrioventricular Valve Disease (Myxomatous AV Valvular Degeneration)
This disease goes by several names. They include endocardiosis, mucoid valvular degeneration, chronic valvular fibrosis and acquired mitral regurgitation/insufficiency. It is the most common cause of heart disease and congestive heart failure (CHF) in the dog. Tricuspid valve regurgitation can also occur with this disease. It is rarely seen in cats.
Cause
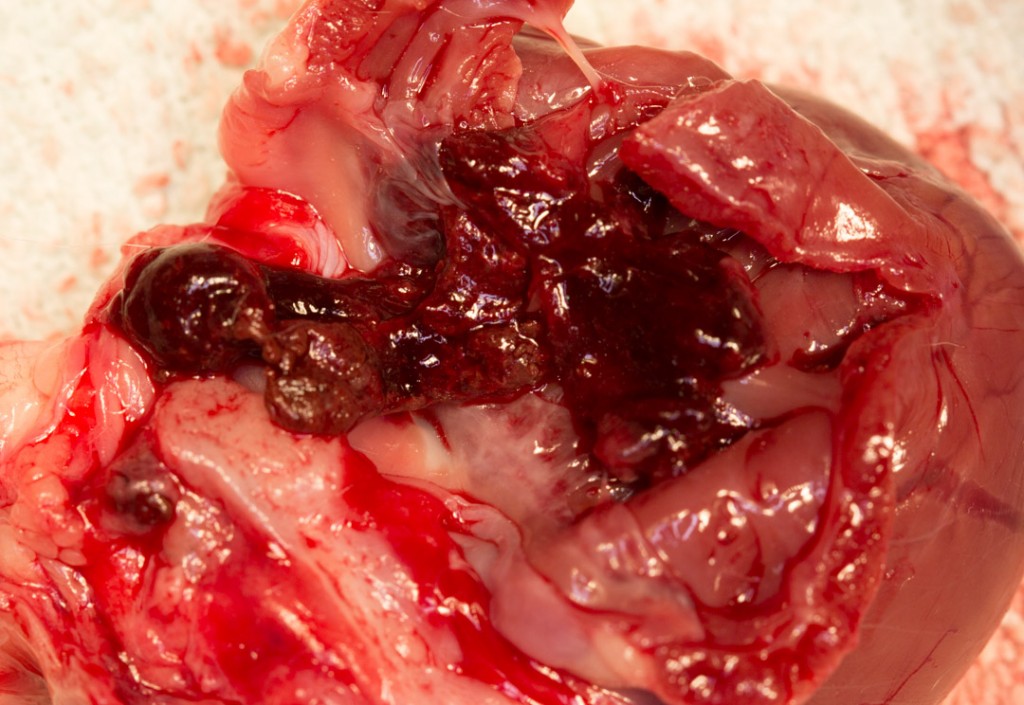
The exact cause is unknown. It effects the mitral valve more commonly than the tricuspid valve, although both can be involved. It probably affects the mitral valve more commonly because of the high pressure in the left ventricle. As dogs age nodules form along the edge of mitral and tricuspid valves. When they get thicker the valves begin to leak (regurgitation), and as the disease progresses, the valves become deformed and shrink. You saw this previously in the necropsy pictures of the dog heart. As the problem progresses the chordinae tendinae might even rupture.
As the blood regurgitates abnormally backwards into the left atrium it increases the pressure in the atrium, making it harder for blood to flow from the lungs into the heart (from the pulmonary vein to the left atrium). As the back pressure increases, the pressure in the veins of the lungs increases to a point (pulmonary hypertension) where the fluid leaks out, leading to pulmonary edema.
This regurgitating flow of blood through the left atrium eventually causes it to enlarge (you saw this in the radiograph pictures). The regurgitating blood can go from the left ventricle through this valve and into the left atrium with such force that it causes “jet” lesions in the wall of the left atrium. The left atrium might also develop an arrhythmia as it continues to dilate. The enlarging left atrium can actually tear and cause blood to leak within the pericardial sac.
Since some of the blood that would normally be ejected by the left ventricle is now regurgitating back into the left atrium there is less flow of blood out of the left ventricle and into the aorta. This can begin the process of poor perfusion, leading to the cascading series of events culminating in congestive heart failure (CHF). Not every case of chronic atrioventricular valve disease will lead to heart failure though. Some dogs can have thickened and deformed valves and never show any symptoms.
To review all of this again in more detail follow our Heart Anatomy & Physiology Page.
Signalment
It usually occurs in smaller breed dogs, notably:
- Poodles
- Miniature Schnauzers
- Chihuahuas
- Fox terriers
- Cocker spaniels
- Boston terriers
- Cavalier King Charles spaniels
- Lhasa apso’s
- Dachshunds
- Shetland sheepdogs
History
Symptoms might include exercise intolerance, weakness, syncope (passing out), cough, shortness of breath, and lethargy. Some pets have no symptoms
Physical Exam
A heart murmur along with an arrhythmia is a clue to this disease. As the problem progresses the murmur becomes louder. In the later stages of the disease the fluid that builds up in the lungs (pulmonary edema) can be heard with the stethoscope also. Fluid in the abdomen, called ascites, could also occur. In cat there might be general fluid in the chest surrounding the lungs called pleural effusion.
An irregular rhythm and increased heart rate might also be present as the disease progresses. In the early stages of this disease there might not be any abnormalities on the physical exam.
Diagnostic Tests
Blood samples are usually normal if only the heart is having a problem. Since these are geriatric patients usually, a blood sample is still indicated to check for other problems in pets this age.
Radiographs are used commonly to help in the diagnosis. The left atrium is enlarged, and sometimes the left ventricle. We might also find enlargement of the pulmonary veins and even evidence of pulmonary edema.
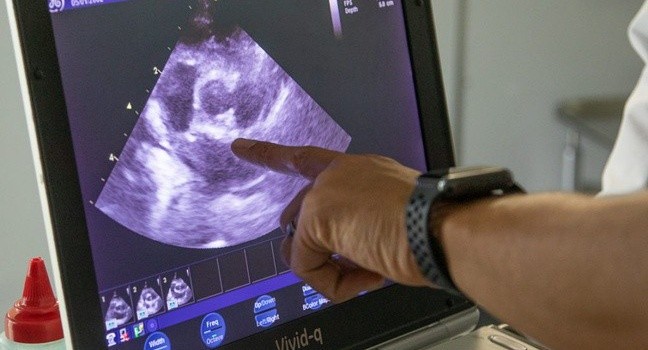
An echocardiogram can also give us significant information. The abnormal valves can be seen, along with rupture of the chordae tendinae in some cases. The doppler can actually view the blood regurgitating through the abnormal valve. The left ventricle might also be enlarged.
Our cardiologist Dr. Fred Brewer is pointing to a heart valve on this echocardiogram
This is what mitral regurgitation looks like during a doppler echocardiogram
In the early stages the ECG might be normal. As the problem progresses arrhythmia’s might be present.
Treatment
- Surgery and balloon catheter dilation are helpful but may be of limited value. Medical therapy is used to treat this problem if it progresses to CHF.
- Medical therapy is utilized to slow the progression of the disease (minimize the compensation mechanism we describe earlier), control the fluid that builds up in the lungs, and decrease the heart rate as the problem worsens. The advent of ACE inhibitors (afterload reducers) has given us the opportunity to help slow the progression of this incurable problem.
- Therapy might depend on the stage of the disease. If there is a murmur in one of the affected breeds, but the left atrium is not enlarged, then minimizing sodium (salt) in the diet might be of help. As the murmur intensifies and the left atrium enlarges we will start Enalapril, and continue with the low sodium diet. As the murmur intensifies and the problem progresses we might increase the dose of Enalapril.
- Pimobendan is of significant help to the heart
- When a cough appears lasix will be used, and even a beta adrenergic blocker. If pneumonia occurs or other lung problems become apparent we will also use antibiotics and bronchodilators.
Prognosis
Mildly affected dogs can have a good quality of life for many years. It all depends on when the diagnosis is made and when therapy is instituted.
All dogs on therapy for CHF should be monitored every 3-6 months to adjust for changes. This includes a blood panel with thyroid, a chemistry panel, ECG, and chest radiographs. Echocardiograms should be performed every 6-12 months to follow the progression of the problem and modify medication
Chronic atrioventricular Valve Disease can mimic infectious endocarditis, which is an actual infection of these valves caused by a bacteria. This is a serious disease that can cause significant illness.
Some of the more common bacteria are:
- Strep. spp.
- Staph. spp.
- E. coli
- Pasteurella spp.
- Klebsiella
These bacteria arise from infections of the gums, skin, urinary tract, prostate, lungs, and internal organs. The infection can spread to the spinal cord, causing a disease we call diskospondylitis. It is treated the same way, since CHF is present. In addition we will use antibiotics for up to several months to control the infection.
Cardiomyopathy
Cardiomyopathy is a disease where the actual heart muscle (myocardium) becomes weak and unable to contract with sufficient force (decreased contractility leading to a decreased stroke volume) to provide adequate perfusion (reduced cardiac output) for the cells of the body. Pets that get cardiomyopathy have a poor prognosis in general.
There are three types of cardiomyopathy:
Dilated
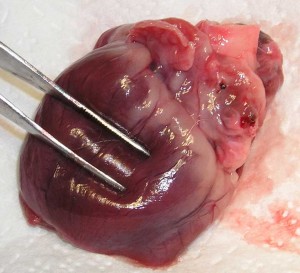
The heart muscle is weak and flabby, and does not have the strength to contract with enough force to provide adequate perfusion of the cells. This form is rare in cats now because of supplementation with Taurine.
This is the heart of a cat with this disease. The forceps are pushing on the ventricles and showing how flabby they are.
Hypertrophic
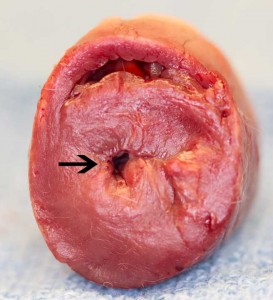
The heart muscle has become so thickened that the left ventricle chamber is too small to allow an adequate amount of blood to flow into it (diastole) before it contracts (systole) and perfuses the cells of the body. It is like a bodybuilder who is too buff to move efficiently.
This is the form of the disease that is prevalent in cats. The heart muscle might hypertrophy due to hypertension or problems with the outflow tract of the aorta.
The bottom tiny opening (arrow) is the left ventricle surrounded by excessive thickened heart muscle. The opening should be 4x this size. You can see it is just too small to hold enough blood to be pumped out of the aorta to the cells of the body.
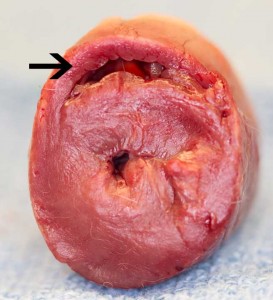
This increase muscularity of the left ventricle increases pressure in the left atrium, causing it to dilate. This increases the pressure in the pulmonary veins leading to pulmonary edema. Pulmonary edema (congestive heart failure) is fluid in the lungs, and is a serious end consequence of cardiomyopathy.
This arrow points to the dilated left atrium, which is 2x larger than it should be
Restrictive (Intermediate)
This form has characteristics similar to dilated and hypertrophic. Cats with this problem have scar tissue instead of normal heart muscle. The scar tissue decreased the strength of the heart, so it pumps out less blood at each beat (decreased stroke volume).
The diseased heart muscle beats irregularly (arrhythmia) and does not have the contractility to pump blood to the rest of the body (decreased cardiac output). This leads to the congestive heart failure we described in the pathophysiology section. In some cases there is sudden death from the arrhythmia that occurs.
Cause
Viruses, toxins, drugs, and taurine deficiency are suspected as causes. In most cases, especially in the breeds that are prone to this problem, the cause is unknown.
Signalment
This disease occurs in large breed dogs like the Great Dane, Labrador, German Shepherd, St. Bernard, Irish wolfhound, English cocker spaniel, Scottish deerhound and Boxer. It is especially prevalent in Doberman pinschers. Most of these dogs are males and get the dilated version of cardiomyopathy.
Even though dogs of any age can get this problem, the tend to me middle aged. Dilated cardiomyopathy also occurs in Burmese, Siamese, and Abyssinians.
History
The symptoms noted are those of congestive heart failure (CHF). Typical symptoms include weakness, poor appetite (anorexia), cough, breathing difficulty (dyspnea), weight loss collapse (syncope) and distended abdomen (ascites). In some cases sudden death occurs before any symptoms.
Some Doberman pinschers can have this disease and not show symptoms for several years. By then the prognosis is poor.
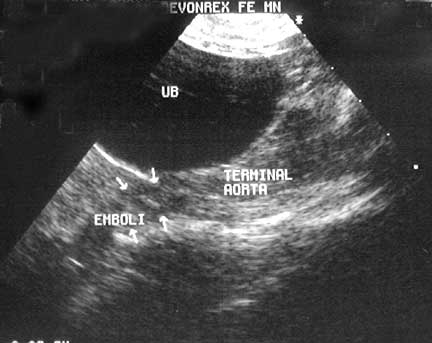
In cats the symptoms are similar. Unfortunately, a significant number of cats do not show any symptoms, they just have a sudden death. Cats also get paralyzed in their back legs because of a blood clot (thrombus) that enters the blood vessels to the back legs. This is called a “saddle thrombus” because it occurs at the point where the abdominal aorta branches into each of the arteries that supplies the rear legs with blood.
The blood clot arises from the pooling of blood that occurs in the left atrium secondary to the hypertrophy of the left ventricle (described above in the hypertrophic section). These cats are in significant pain, and palpation of the rear legs might reveal a cooler temperature than the rest of the extremities. The prognosis is poor for this form of feline cardiomyopathy.
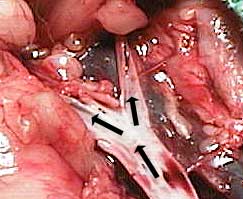
To get you oriented for the following pictures, this cat’s head is towards the left and the back legs are towards the right. Blood coming from the heart flows down the abdominal aorta (labeled as artery in this picture) and towards the rear legs. At the vertical arrow the abdominal aorta branches into the internal and external iliac arteries.
From there it goes into the femoral arteries to supply the rear legs with freshly oxygenated blood. The poorly oxygenated blood returns to the heart through the femoral vein, then the iliac veins, and eventually the caudal vena cava (labeled as Vein in this picture). At the vertical arrow is where the saddle thrombus forms.
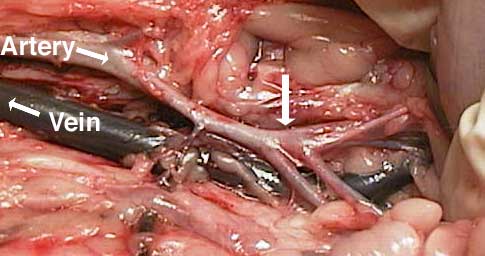
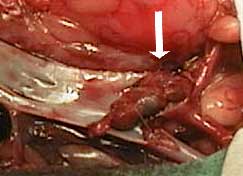
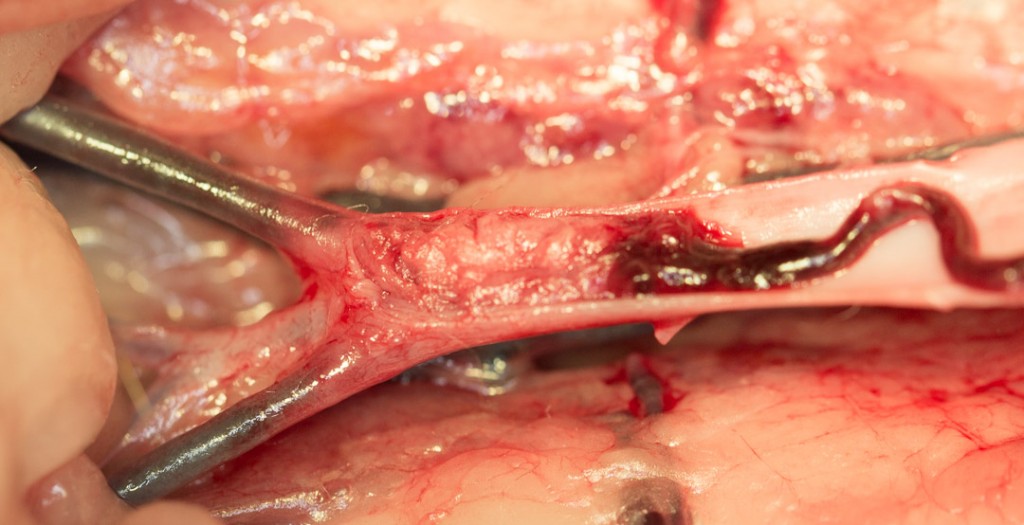
The thrombus (vertical arrow) is now apparent when we open up the arteries
This is the way the artery is supposed to look when there is no thrombus
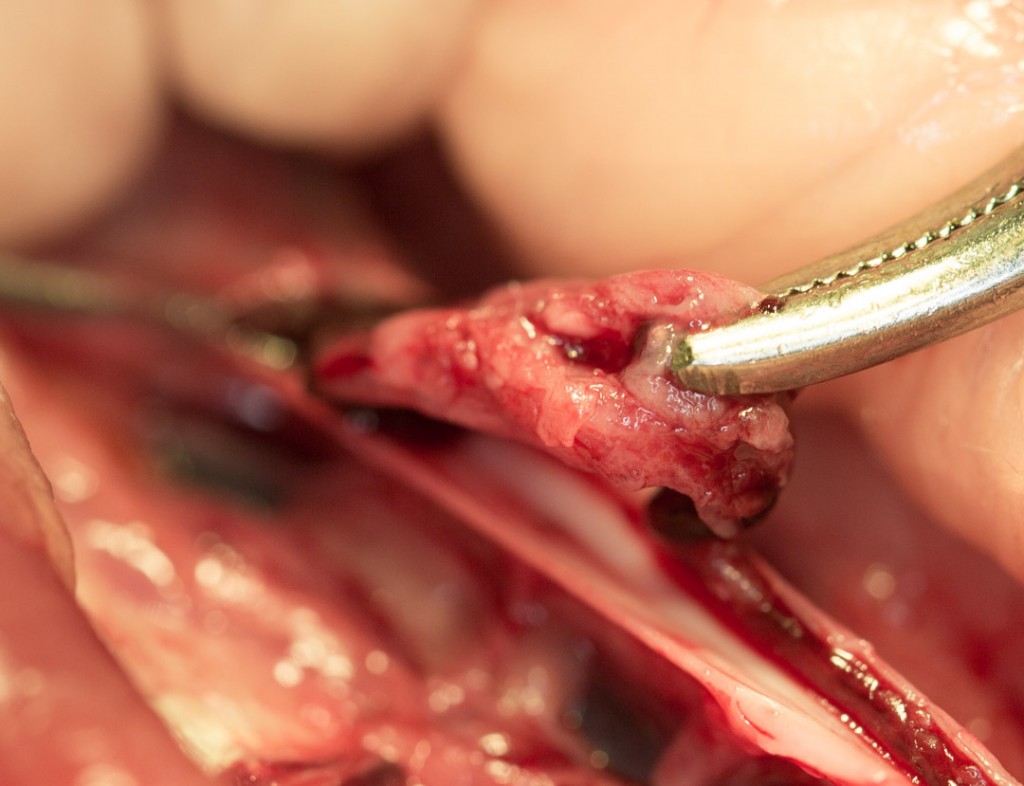
The removed blood clot. You can see why it is called a “Saddle Thrombus”
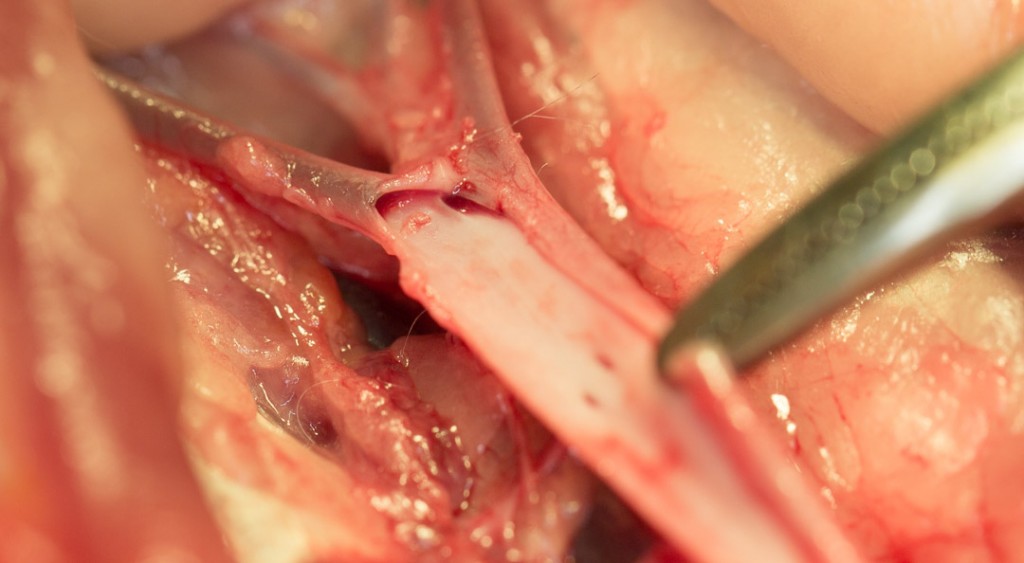
Here is a different cat with the same problem. In this picture the head is to the right, the snake-like clot is getting started at the right side. The large clot blocking the entrance to the blood vessels that supply the rear legs is apparent in the middle of the picture. The blue color to the rear leg vessels on the left is due to a clot that extends into them from the main clot in the center.
This large of a clot completely prevents blood flow to the back legs, a painful condition
Removing the large clot
You can see the very smooth wall of the aorta with the clot removed
The heart with a large clot in one of the chambers is the source of the clot in the aorta and legs. The clot is the dark structure in the middle of the heart towards the top.
Physical Exam
Abnormalities found during an exam are similar to other heart diseases and even other diseases in general. Auscultation of the thorax might reveal an arrhythmia and high heart rate. There might even be a pulse deficit if atrial arrhythmia is present. a murmur might be found in some pets with cardiomyopathy, although not every pet with a murmur has this disease.
Cats with a saddle thrombus might have weak or non existent femoral pulses. They will be painful and might not be able to use the rear legs.
Diagnostic Tests
The ECG can pick up arrhythmia’s caused by cardiomyopathy, in some cases prior to the onset of congestive heart failure. In breeds that are highly prone to this problem like the Doberman pinscher, it is advised to perform an ECG yearly to monitor for these changes.
On a radiograph the heart will appear enlarged because of the dilatation of all the chambers. Pulmonary edema and congested veins are indications of congestive heart failure secondary to cardiomyopathy.
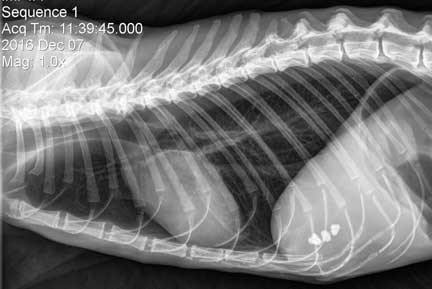
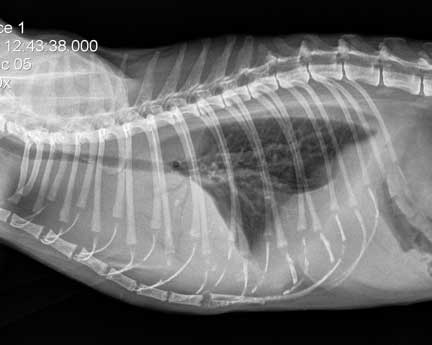
The first X-Ray is from a normal cat, the second is from a cat with heart failure.
You can distinctly see the white heart and the black lungs. Those 3 white areas to the right (in the abdomen) are stones in the gall bladder.
This cat has pleural effusion due to heart failure. There is fluid in the chest obscuring the heart and causing the caudal lung lobes to collapse
Some Boxers with cardiomyopathy will have normal appearing hearts on a radiograph.
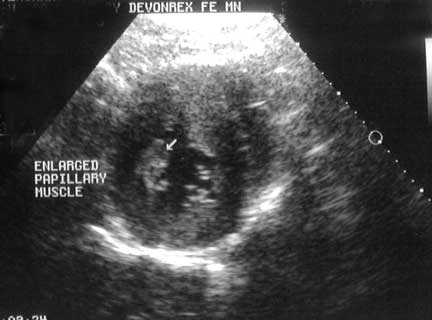
An echocardiogram is the gold standard for diagnosing HCM and heart failure. This is an echocardiogram of the cat with the enlarged heart above. . We could even visualize the blood swirling around as it formed a pre-clot that would eventually become a thrombus and expelled from the ventricle to large in some artery in the body.
The echocardiogram showed an enlarged papillary muscle in the ventricles
We could even visualize the thrombus at the end of the aorta just before it branches into the iliac arteries
These are the calculations made during an echo to determine if a heart is having a problem
This is the final report from our cardiologist on a cat with HCM (Hypertrophic CardioMyopathy)
Treatment
Routine treatment for congestive heart failure and arrhythmias is used. The effectiveness of therapy depends on the severity of the disease and how long the problem has been present. Some dogs and cats can do well for several months and even years if treated early enough.
Since the arrhythmia that occurs with cardiomyopathy can be detected before the onset of congestive heart failure, it is obvious that checking for this problem is important, particularly in Doberman pinschers and Boxers. Doberman pinschers with atrial fibrillation and dilated cardiomyopathy have a poor prognosis.
Cats might also be treated with aspirin to prevent a saddle thrombus. It is imperative that cats are kept in a relatively stress free environment.
The best long term approach for dogs and cats is not to breed lines that are prone to this problem.
Heartworm
Cause
Heartworm is caused by a parasite called dirofiliaria immitis. It is spread to dogs, and recently cats, by a mosquito. The mosquito is a necessary part of the life cycle.
In an affected dog or cat, female heartworms that reside in the pulmonary artery release small larval forms called microfilaria. Microfilaria circulate in the bloodstream for many months, and even sometimes years. If a mosquito bites a dog or cat that has circulating microfilaria it ingests them. These larva go through changes in the mosquito over the next 2 weeks. When this mosquito bites a dog it injects this larvae into a new dog. The larvae continue to develop in this dogs tissue and eventually become adult heartworms in the heart or pulmonary arteries 6-7 months later.
Traditionally this disease only occurred in hot and humid states that were essential to mosquito breeding. The disease occurs throughout our country now, although heartworm preventive medications have had a significant effect in lowering the incidence of heartworms.
Pathophysiology
The degree of heart disease that occurs depends on the number of heartworms, how long they have been present, and how the immune system reacts to them.
The actual presence of the worms in the arteries induces an inflammatory reaction causing blood clots (thrombi) to form. It also causes fluid to leak out of the artery into the surrounding tissue. Eventually pulmonary hypertension develops leading to an enlarged right ventricle as it works harder to pump the blood against all this pressure (afterload).
If a large number of worms are present they can literally fill up the right atrium and caudal vena cava. Not only does this interfere with the proper flow of blood through the heart, it also causes changes in the red blood cells and clotting system. In serious cases this can cause a bleeding disorder called disseminated intravascular coagulation (DIC).
The immune system can destroy the microfilaria released by adult heartworms in the pulmonary capillaries, resulting in a negative heartworm test. This is called occult heartworm disease.
Signalment
Dogs and cats of any breed can be infected, although we tend to see it more in large male dogs. Since it takes at least 6 months from the time a mosquito injects microfilaria into a dog until these microfilaria become adult heartworms, puppies must be at least 6 months of age before adult heartworms are present. Most dogs are diagnosed at middle age.
History
- Many dogs do not have any symptoms until heart failure progresses. This emphasizes the need for yearly testing. When symptoms occur they can include:
- Poor appetite
- Weight loss
- Coughing
- Lethargy
- Difficult breathing
- Exercise intolerance
- Distended abdomen
These are the symptoms of general heart failure, yet they can also occur in other diseases besides heartworm.
Physical Exam
- In many cases the physical exam is normal. As the disease progresses the following exam findings might occur:
- Cough when the windpipe (trachea) is palpated
- Increased respiratory rate (tachypnea)
- Increased lung sounds (crackles) when ausculting the chest with a stethoscope
Diagnosis
Radiographic changes that might occur include an enlarged right heart along with an enlargement of the pulmonary artery. Several smaller arteries might be dilated, tortuous, or pruned. Other changes are similar to those that occur with right heart failure.
An EKG might show changes indicative of right heart enlargement.
A routine blood panel might reveal an elevation of certain types of white blood cells called eosinophils and basophils. There might even be an elevated protein level and evidence of kidney problems.
Microfilaria detection is the best and most accurate way to diagnose adult heartworms. We can see them microscopically when we look at a blood smear from an infected dog. Unfortunately, this diagnostic method is unreliable due to the small size of the microfilaria in relation to the large amount of blood in the bloodstream.
Several tests were developed to increase our ability to see these microfilaria on the blood smear. They made a major improvement in diagnostic ability, but are still not as good as immunodiagnosis.
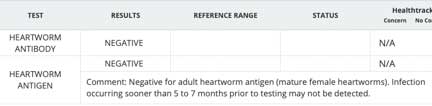
Immunodiagnosis involves looking for antigens of microfilaria or antibodies against the microfilaria using monoclonal antibody techniques. Several of these tests can be used in our office, therefore you get the report within 30 minutes. If the test is negative, then your dog or cat probably does not have heartworm.
This is the report we get from our lab when we request a heartworm test
Unfortunately, reproductively inactive female adult heartworms, along with male heartworms, will also show up negative on these tests. This is called occult heartworm disease. On occasion, false positives can occur, particularly if other parasites (roundworms, etc.) are present or there is another nonpathogenic heartworm present called dipetalonema reconditum.
Approximately 15% of the heartworm infected dog have occult heartworm disease. In occult heartworm disease there are adult heartworm parasites in the pulmonary arteries yet there are no microfilaria circulating in the bloodstream. Since the primary method of diagnosis is detection of these microfilaria, either visually, or with monoclonal antibody tests, it is possible to miss a diagnosis.
There are several reasons why occult heartworm disease might occur. It happens early in the course of infection when adult female heartworms have not had enough chance to release microfilaria to any significant extent. At the other end of the spectrum, old adult heartworms might not release microfilaria. It can occur if mostly male heartworms are causing an infection, since they do not release microfilaria. It can also occur if adult heartworms are present and your dog is on heartworm preventive medication.
Finally, it can occur if the immune system produces antibodies to microfilaria, suppressing their numbers so low that they are not detected with current monoclonal antibody techniques. Unfortunately, in this scenario there is significant pathology to the lung tissue because of this immune system reaction. These dogs usually present with severe breathing problems.
In general, we are starting to encounter dogs with adult heartworms that have minimal circulating larvae. This is making diagnosis more difficult.
Treatment
This is a disease where the treatment is almost as bad as the disease. No treatment is completely effective although the dog or cat feels substantially better. The worms that are killed can block small blood vessels and cause thrombosis. If large numbers of heartworms are present there can be a massive amount of thrombosis.
This can increase pulmonary hypertension and lead to additional fluid buildup in the lungs, even leading to disseminated intravascular coagulation. The inflammatory reaction that occurs can also affect the glomeruli of the kidneys. All treated dogs need to rest to minimize a reaction from the dead heartworms.
If a dog is already in heart failure it needs to be stabilized prior to treating the adult heartworms. This includes the routine treatment for CHF, particularly diuretics, digoxin, Enalapril®, exercise restriction, and aspirin.
The primary drug used to treat adult heartworms is melarsomine. It has arsenic as its active ingredient, although side effects are less than previous arsenic treatment for heartworms. It still has the potential to cause problems with the kidneys (nephrotoxicity) and liver (hepatotoxicity), so close monitoring is vital.
Dead heartworms can still cause a pulmonary allergic reaction with its associated problems. This problem is partially mitigated by giving melarsomine over a 2 day period of time instead of all at once. If your dog has severe heartworm disease it might be given one treatment, then sent home to rest for one month. At that time, it is given a full dose over 2 days.
Another treatment modality used by some veterinarians is to use heartworm preventive medications at a modified dose to slowly kill adult heartworms over 16 months. The theory is that the slow killing of the worms will minimize reaction from the death of adult worms. The disadvantage to this slow killing involves the damage the adult heartworms can cause during that time.
In some cases we use aspirin or cortisone as an adjunct to our routine therapy. These drugs minimize blood clots, platelet problems, and inflammation.
Once the adult heartworms are killed the microfilaria that are circulating in the bloodstream are our next target. The drug of choice, except in Collie breeds who can have a serious reaction, is Ivermectin. In Collie breeds we use a drug called Levamisole®.
Since heartworm is such a serious disease, and treatment has potential toxicity, it is obvious that prevention is the best way to go. There are many products that are highly effective at preventing heartworms. They all should be started within one month of the mosquito season, and continued to the end of the mosquito season.
Since many of these preventatives also control fleas and internal parasites, we recommend their use year round. Except for Revolution, your dog must be tested negative for heartworms prior to instituting these preventive medications.
These preventive medications need to be given monthly. If your dog does get adult heartworms because you did not follow the monthly schedule you set up a diagnostic problem. These dogs will have so few circulating microfilaria that we might not be able to make an accurate diagnosis.
Some of the more popular preventatives are:
- Trifexis® – It prevents heart worm, kills fleas, and treats for roundworms, hookworms, and whipworms. Its one of most recommend and used products.
- Heartgard® and Heartgard Plus®- They contain Ivermectin, and can be safely used in Collies over 10#. In addition, Heartgard Plus kills internal parasites. It is given on a monthly basis.
- Interceptor® – It contains milbemycin, which in addition to preventing heartworms also kills circulating microfilaria and sterilizes adult heartworms. It is also given on a monthly basis.
- Sentinel® – It contains milbemycin and lufeneron, so in addition to its ability to prevent heartworms, it controls roundworms, hookworms, whipworms and flea eggs.
- Revolution®- It contains the drug Selamectin, which is similar to Ivermectin, but much more broad spectrum in action. An advantage of Revolution is no adverse reaction if the dog already has microfilaria circulating from a current adult heartworm infection. In can be used safely in Collies, and treats and controls fleas in dogs and cats, ear mites in dogs and cats, sarcoptic mange and ticks in dogs. It even treats hookworms and roundworms in cats.
In general, the prognosis for dogs with heartworm disease is good. As is usually the case, it depends on the number of worms present, how long the disease has been occurring, and how the immune system is reacting. Although all of the worms are not usually killed, their decrease results in significant breathing improvement in almost all dogs.
Feline Heartworm Disease
Heartworm disease in cats is similar to dogs, yet there are some significant differences. Just like in dogs it is the mosquito that spreads the disease.
Symptoms can range from none to sudden death or chronic illness. Most do not have any symptoms. If they are present, they usually include breathing problems (similar to asthma) and vomiting and diarrhea.
They usually have less worms and more occult heartworm disease. Circulating microfilaria are not detectable with the microscope, and diagnosis using other means is difficult.
We rarely treat cats for heartworm due to toxicity from the treatment. Melarsomine is not used to kill adult heartworms. Prednisolone is used in small doses in select cases.
Due to the potential severity of this disease, the difficulty of diagnosis, and the toxicity of the treatment, prevention is paramount. The drugs used to control fleas also help prevent feline heartworm. These include Revolution® and HeartGard® for Cats. In warmer climates these preventatives should be given year round.
Aortic Stenosis
Cause
This disease of dogs arises when abnormal tissue near the aortic valve obstructs the flow of blood out of the left ventricle. If severe enough it can eventually lead to CHF and ventricular arrhythmias.
Signalment
It usually occurs in large breed dogs, notably:
- Newfoundland’s
- Golden Retrievers
- Rottweiler’s
- Boxers
- German Shepherds
- History
- Symptoms include exercise intolerance, rear limb weakness, syncope (passing out), cough, shortness of breath, and even death.
Physical Exam
- A heart murmur along with an arrhythmia is a clue to this disease.
- Diagnostic Tests
- Radiographs and electrocardiograms are of help in the more advanced cases. Echocardiograms are helpful in the moderate to severe cases.
- Treatment
- Surgery and balloon catheter dilation are helpful but may be of limited value. Medical therapy is used to treat CHF.
- Prognosis
- Mildly affected dogs can have a good quality of life. If the problem is more severe the prognosis is not as good.
Pulmonic Stenosis
Cause
This disease of dogs arises when abnormal tissue near the pulmonic valve obstructs the flow of blood out of the right ventricle. If severe enough it can eventually lead to an enlarged right heart and regurgitation of blood through the tricupid valve and into the right atrium. If severe enough right sided CHF might occur.
Signalment
The following breeds are know to be prone to pulmonic stenosis:
- Beagle
- Chihuahua
- English bulldog
- Keeshond
- Samoyed
- Mastiff
- Newfoundland
- Boxer
- Terrier breeds
- Spaniel breeds
History
Many dogs have no initial symptoms. If symptoms are present, they might include exercise intolerance, ascites, syncope (passing out), shortness of breath, and even death.
Physical Exam
A heart murmur along with distended jugular vein might be present.
Diagnostic Tests
Radiographs and electrocardiograms might show right ventricular enlargement. Echocardiograms are helpful in many cases.
Treatment
If the problem is severe enough surgery is used to correct the problem. This depends on exactly where the problem is in this valve along with other blood vessels to the heart. Balloon catheter dilation can also be used.
Medical therapy is used if CHF is present. When the CHF is stabilized surgery might be utilized.
Prognosis
Mildly affected dogs can have a good quality of life. If the problem is more severe the prognosis is not as good. These dogs should be monitored yearly for changes in their condition.
Pulmonic Stenosis
Cause
In this disease an abnormal opening occurs between the ventricles, which allows blood to flow directly from the left ventricle (higher pressure) to the right ventricle (lower pressure). This disease occurs in dogs and cats. The severity of this disease depends on exactly where the opening is located and how big it is. Eventually left sided CHF can occur because of an overload of blood to the left ventricle as more blood is shunted through the right ventricle, leading to more blood flowing through the lungs, leading to more blood flowing back into the left atrium and left ventricle.
Signalment
The following breeds are know to be prone to PS:
- English bulldog
- English springer spaniel
- History
- Many pets have no initial symptoms. If symptoms are present, they might include coughing and shortness of breath as CHF develops
Physical Exam
A heart murmur is commonly present.
Diagnostic Tests
Radiographs and electrocardiograms might show left ventricular enlargement and distention of the pulmonary vessels. Echocardiograms are used to confirm the diagnosis.
Treatment
Many pets need no treatment at all. Surgery is difficult to perform. Medical Therapy is used to treat CHF if it occurs.
Prognosis
Prognosis is good if the opening is small. Larger defects need to be monitored yearly.
Patent Ductus Arteriosis (PDA)
Cause
In the uterus the mother of the dog supplies the dog with its oxygen since obviously a puppy in the uterus is not breathing. One of the mechanisms of the body to bypass the lungs of the pup is to flow the blood directly from the pulmonary artery to the aorta. When the pup is born, this direct communication between these vessels closes, the blood now flows from the pulmonary artery to the lungs to get its oxygen. This disease of dogs occurs when the communication between the descending aorta and the pulmonary artery fails to close after birth. This abnormal flow of blood overloads the left side of the heart, leading eventually to CHF.
Signalment
The following breeds are know to be prone to PDA:
- Collie
- Maltese
- Poodle
- Pomeranian
- English springer spaniel
- Keeshond
- Bichon frise
- Yorkshire terriers
- Shetland sheepdogs
- German shepherds
History
Many dogs have no initial symptoms. If symptoms are present, they might include coughing and shortness of breath.
Physical Exam
A heart murmur called a continuous (occurs during systole and diastole) murmur, is a clue to this disease.
Diagnostic Tests
Radiographs and electrocardiograms might show left ventricular enlargement and distention of the pulmonary vessels. Echocardiograms are helpful but not needed in many cases.
Treatment
A surgical procedure that closes this abnormal connection is used to treat PDA.
Prognosis
Prognosis is good if surgery is performed before the symptoms of CHF start appearing.
Medical Treatment of Heart Disease
The medical management of animals with CHF (congestive heart failure) is aimed at controlling the deleterious effects of the underlying pathology. These effects typically include pulmonary congestion and edema, cardiac arrhythmias, reduced cardiac output, and excessive vasoconstriction. Many medications are used to treat heart disease. In almost every case they can only control the symptoms, and hopefully, slow down the progression of the disease.
In general, medications used to treat cardiac disease, especially CHF, are highly beneficial. The goal of therapy is to improved the quality of life of these pets while simultaneously minimizing the side effects of the drugs used. Most pets will not go back to being able to exercising vigorously, as a matter of fact, too much exercise can destabilize compensated dogs and cats.
Therapy needs to be tailored made to each pet, and again, constant monitoring is needed to adjust for any changes that are occurring. This means that blood panels, radiographs, ECGs, and blood pressure need to be checked weekly initially, then every 3-6 months, assuming the heart failure is under control.
Cardiac disease is commonly diagnosed in geriatric patients that have other problems simultaneously. Some of the medications used to treat heart disease can exacerbate other medical problems common in geriatric patients. Using these medications properly tends to be a balancing act, minimizing their deleterious affects while maximizing their advantageous properties. This is particularly true if a pet has kidney disease along with heart disease. This balancing act requires constant monitoring.
Many drugs are used in cardiovascular disease. We will go over the more common treatments, especially in regards to congestive heart failure.
ACE (Angiotensin Converting Enzyme) Inhibitors
These drugs are a part of the treatment plan of almost every dog with CHF. The addition of Enalapril® or Benazepril® to conventional therapy in dogs with chronic congestive heart failure resulted in a significant decrease in clinical signs and a 92% increase in survival time. The use of vasodilators, such as Enalapril®, increase the survival time of dogs with CHF. This is especially true in CHF from cardiomyopathy, but does not necessarily apply to dogs with CHF from mitral insufficiency.
They add to the quality of your dogs life by minimizing the fluid buildup in the lungs (pulmonary edema) and abdomen (ascites).
In general, ACE inhibitors lower the blood pressure (decrease afterload) and decrease salt and water retention. They work by inhibiting the conversion of angiotensin I to angiotensin II in the lungs. We discussed this in the Cardiac Anatomy and Physiology section of our heart disease page.
This decreases fluid buildup in the lungs, thorax, and abdomen, and it also makes it easier for a weakened or enlarged heart to pump the blood out into the bloodstream. Kidney values and electrolytes should be monitored while on ACE Inhibitors.
The more common ACE inhibitors we use are Enalapril®, Benazepril®, and Captopril®. Enalapril® is approved for use in the dog by the FDA, and is the most common ACE inhibitor we use. ACE inhibitors can take up to 7 days to produce beneficial effects, and need to be constantly adjusted to maximize their benefits.
ACE inhibitors are commonly used in people that have high blood pressure (hypertension), even if they do not have heart failure.
ARB’s (angiotensin receptor blockers) are also used, and have a mechanism of action similar to ACE inhibitors
Diuretics
Diuretics (lasix, also called furosemide) are the mainstay of treatment for CHF, and should be used in conjunction with ACE inhibitors.
Lasix is a loop diuretic. That means it has its effects on a section of the kidney called the loop of Henle. It is here that lasix causes more sodium (salt) to be excreted from the body. Sodium pulls water with it when it is excreted, so urination increases and fluid level of water in the bloodstream decreases.
This decreases the blood pressure in the capillaries, so less fluid leaks out into the lungs (pulmonary edema) and abdomen (ascites). Another medication, called spironolactone, is also used with lasix, or in place of it.
Overuse of diuretics can cause dehydration and can interfere with normal kidney function. As was already mentioned, lasix use should be monitored with a blood panel every 3-6 months to assess kidney function. As a geriatric pet ages, the kidneys and heart can both have disease, so the use of lasix is a balancing act between these two diseases.
It is rare for a dog or cat to need potassium supplementation (K+) while on a diuretic, unlike people. Your pet will drink more than usual, so make sure fresh water is available at all times.
As a rule of thumb, if a dog or cat in congestive heart failure increases its respiratory rate routinely beyond 30 breaths per minute, we give additional lasix. It is better off to remove the fluid from the lungs and let the red blood cells get oxygen to deliver to the cells, at the expense of the kidneys, than to treat the kidneys with extra fluids to flush waste products out, and have the lungs fill up with more fluid. The more we are able to run diagnostic tests to monitor this, the better we can titrate the diuretics and fluids.
Pimobendan (Vetmedin®)
This FDA approved drug is in a class of drugs called indodilators. This means it increases the strength of the contraction of the heart muscles (ventricles). This is called a positive inotropic effect. It also helps dilate the peripheral blood vessels, decreasing afterload, and making it easier on the heart to push the blood into the arteries. If you review our heart anatomy and physiology page you will learn much more about all of this.
This drugs has been a major help in the treatment of congestive heart failure due to dilated cardiomyopathy or endocardiosis. It increases survival time and quality of life in these patients.
Diet
Minimizing salt in the diet is beneficial in preventing fluid buildup (ascites of pulmonary edema) only when the fluid is present. If you start a restricted sodium diet too soon you can actually cause the opposite effect.
Typical food include Hills K/D and H/D. Many pets eat these foods well, but if they have diminished appetite on these foods then they are of no benefit, since they will continue to lose weight and be lethargic.
Supplements
Supplementation with Omega 3 fatty acids might be of help, along with carnitine and taurine in specific cases of dilated cardiomyopathy. Carnitine will only be effective in a small number of dogs. To know for sure if a dog is carnitine deficient, a biopsy of the heart muscle is needed.
Coenzyme Q10 is also used, although this has not been proven to be effective either.
Exercise Restriction
If your dog or cat has heart failure it needs to stay relatively inactive. The heart is already compromised and working at maximum capacity, and does not have the capacity to increase cardiac output.
Cardiac Emergency
Some pets are presented to us having severe difficulty breathing from pulmonary edema. They can succumb to this problem, so they are a true emergency.
They need to be handled very carefully since they are literally drowning in the own fluids and unable to get air. It would be like a person firmly holding a pillow over your face. These pets need to be left alone initially and given 100% oxygen. Once they are more stable and can be handled we give the medication.
100% Oxygen
Nitroglycerin to dilate the blood vessels and decrease the after load.
We use gloves to put the nitroglycerin on the ears since it is absorbed through the skin
We will also hook up a pulse oximeter to assess the oxygen in the red blood cells
Lasix to reduce pulmonary edema.
We might use low levels of low sodium intravenous fluids to help the kidneys if they are failing also. We cannot thoroughly flush out kidney waste products because this much fluid given intravenously will exacerbate the pulmonary edema that is already present. Once the emergency is under control we might be able to slowly increase these fluids.
Oral medications have no place in these dogs since they are usually anorectic and likely to have minimal GI motility. In addition, they are unable to absorb the medication through their intestines and into the bloodstream because blood is being shunted away from the intestines and to the vital organs.
The Long Beach Animal Hospital, staffed with emergency vets, is available until the evenings 7 days per week to help if your pet is having any problems, especially shock, seizures, pain, difficulty breathing, or bleeding.
Think of us as your Long Beach Animal Emergency Center to help when you need us for everything from minor problems to major a major emergency. We serve all of Los Angeles and Orange county with our Animal Emergency Center Long Beach, and are easily accessible to most everyone in southern California via Pacific Coast Hwy or the 405 freeway.
If you have an emergency that can be taken care of by us at the Animal Emergency Hospital Long Beach always call us first (562-434-9966) before coming. This way our veterinarians can advise you on what to do at home and so that our staff and doctor can prepare for your arrival. To learn more please read our Emergency Services page.