The purpose of the cardiovascular system (heart and blood vessels) is to provide the cells of the body with oxygen, nutrition, and essential fluids. It also helps these same cells rid themselves of waste products, and distributes hormones and enzymes to allow for normal physiologic processes. It is even a big part of temperature regulation. all of this is no small feat when you consider the fact that the cardiovascular system must supply these needs to a body that contains billions of individual cells.
The cardiovascular system is a very complicated and does not lend itself to a simple explanation and categorization of its functions. This page summarizes this complex system. If you would like substantially more detail, go to our Heart page.
This page also has actual pictures of the heart and the organs of the chest. Most people will not be bothered by their graphic nature, and will actually find them fascinating.
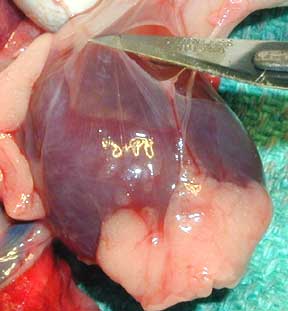
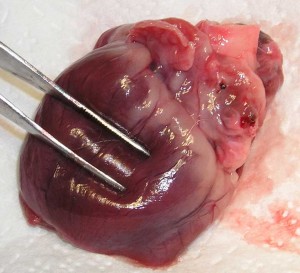
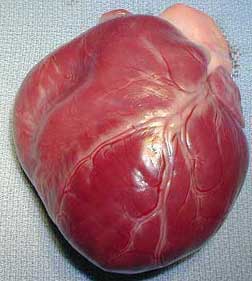
This is the heart of a 50 pound dog. It is about the size of your fist. You can easily see some of the coronary arteries that supply blood to the heart muscle in the same manner that the heart supplies blood to the rest of the body. This organ starts beating before birth, and continues until death. Think of how many beats that is in the lifetime of any living organism!
Later in this page we will be referring to the right heart and left heart, which might give you the impression there are two hearts. There is only one heart- we do this only because it helps to understand the flow of blood through the heart.
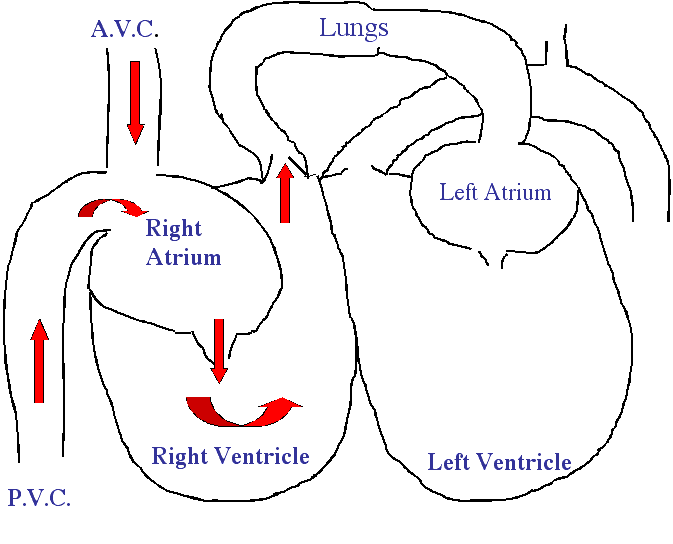
Schematic of Blood Flow Through the Heart
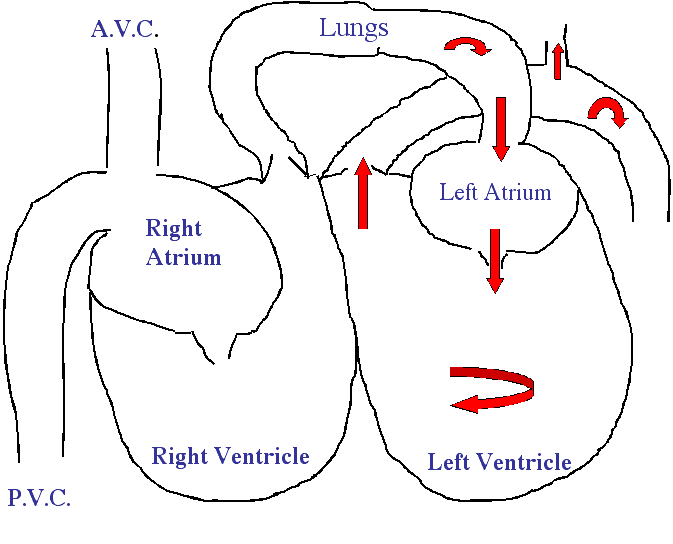
We will be using some basic diagrams to explain the flow of blood through the 4 chambers of the mammalian heart. This will dramatically help in your understanding of the flow of blood. It will also help in understanding the anatomy later in this page when we show you actual anatomic structures of the dogs heart. It might be a good idea to come back to these diagrams when we go into more detail later.
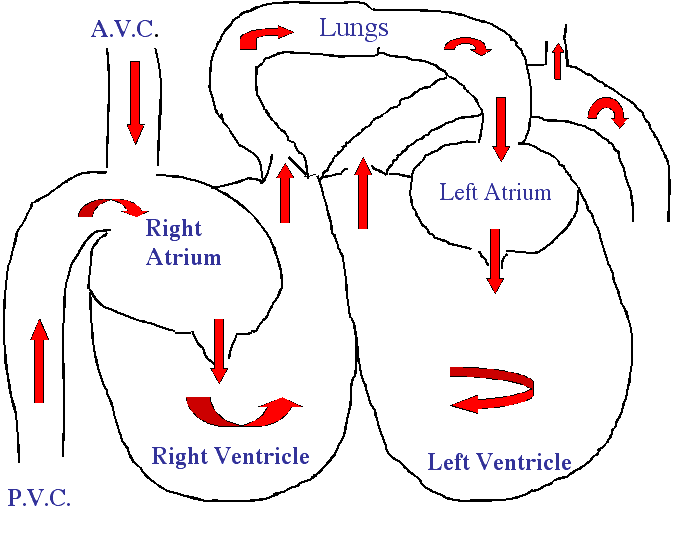
Blood that has supplied the cells with oxygen, and now contains carbon dioxide to be eliminated from the body when we exhale, flows into the heart from 2 directions. From the head, it flows through the anterior vena cava (AVC) into the right atrium. From the back end of the body it flows through the posterior vena cava (PVC) and into the right atrium. When an adequate amount of blood has filled the right atrium (this takes only milliseconds) it contracts, and blood flows through the tricuspid valve (also called the right Atrio-Ventricular valve) and into the right ventricle. The tricuspid valve, like the other valves in the heart, is a one-way valve. In a healthy heart blood can flow only from the atrium into the ventricle.
The blood that is now in the right ventricle rapidly mixes with the small amount of residual blood that remains in the right ventricle from its last contraction. When the right ventricle is filled adequately (again, this takes only a few milliseconds), it contracts and the blood flows through another valve called the pulmonic valve, into the pulmonary artery, and eventually into the lungs. In the lungs the blood rids itself of carbon dioxide and absorbs a fresh supply of oxygen during exhalation and inhalation. The blood goes from poorly oxygenated to freshly oxygenated, and is now ready to supply the cells of the body with fresh oxygen all over again. Now it just has to get to all those billions of cells.
The freshly oxygenated blood in the lungs flows through the pulmonary vein and into the left atrium. Just like in the right atrium, when there is enough blood present, the left atrium contracts and the blood flows through the mitral valve into the left ventricle. Remember this mitral valve since we will be talking about it later in a common heart problem in the geriatric pet called endocardiosis. The mitral valve is a one-way valve also.
The blood that enters the left ventricle mixes with residual blood that remains from the last contraction. When the left ventricle is adequately filled with blood it contracts and ejects its blood through the aortic valve and into the aorta. Once in the aorta, a branch called the brachiocephalic trunk, supplies the head, while the rest flows down the descending aorta and to the rest of the body. a small branch (not shown in this diagram) off the aorta supplies the heart through the coronary artery.
The right and left hearts are doing their work at the same time, so coordination of all this blood flow is critical. This is especially apparent when you realize that a typical dog or cat heart is beating between 100 and 200 beats every minute. This means that for the average dog or cat, everything in this diagram below happens twice each second. Think of the coordination needed in a bird whose heart rate is 350 beats per minute! The heart valves have to open and shut very rapidly, the atria and ventricles have to expand and contract very rapidly also, and the rest of the body has to cooperate in the first place by bringing an adequate amount of blood into the heart through both vena cava’s. In addition, the respiratory system has to cooperate by inhaling air, exhaling air, and exchanging carbon dioxide and oxygen. Its a wonder that all of this can even be coordinated.
When the heart muscle contracts and ejects blood it is called systole. When the heart muscle is relaxing in between systoles, and filling up with blood in readiness for the next contraction, it is called diastole. Diastole is important to the heart muscle itself, since it is during diastole that blood flows into the coronary artery to supply the myocardium.
With such a complicated system it is no wonder that things can go wrong. We will learn more about heart pathology later, first there is more to learn about anatomy and physiology of the cardiovascular system.
Cardiac Anatomy
Cardiac Muscle
The body contains three different types of muscle. The first, called skeletal muscle, is the muscle type we usually think about when we mention muscles. Skeletal muscles provide locomotion and movement- the biceps muscle to move our arms, or the quadriceps muscles to move our legs. These muscles perform their action due to conscious control of our brains. Your arm does not automatically shoot a free throw until you tell it to do so (even when Dr. P tells his arm to shoot the free throw it doesn’t always work as planned).
The second type of muscle is called smooth muscle. Smooth muscles tend to perform their functions automatically without any conscious thought on our part. You don’t tell them what to do, they do it on their own, under the control of the autonomic nervous system (ANS). The muscles that surround arteries to make them constrict or dilate are smooth muscles. The muscles of the intestines that push the food along (a process called peristalsis) are made of smooth muscle.
The last muscle type is called cardiac muscle, and only resides in the heart. Cardiac muscles have their own supply of electricity, and “fire off” on their own without any stimulation.
This is a close-up view of the heart muscle (myocardium) in the left ventricle of a dog. It is thick because this dog’s heart has to spend a lifetime pumping blood to all the cells of the body. Later on when we talk about cardiomyopathy it is this muscle that is affected.
How does the heart beat all by itself? It does this because each heart cell supplies its own electricity. To make a complicated story a little simpler, it has to do with how the heart cells retain or excrete potassium, sodium, and calcium ions. When sodium and calcium are pumped out of the heart cell, potassium is pumped in. This eventually creates an imbalance in their equilibrium, with many more sodium and potassium ions outside of the heart cell than inside. This creates a “positive” charge outside of the heart cell , and the heart cell is now “polarized” (remember this word when we discuss electrocardiograms).
The body eventually wants to correct this imbalance of sodium, calcium, and potassium. So the opposite occurs. Potassium rushes out while the sodium and calcium rush in. The cell is now depolarized, and will stay that way until the positive charge outside the cell again reaches a threshold and the flow once again reverses. Every time this reversal of flow occurs, it generates a spark of electricity which races through the heart. It is this electrical spark that causes heart cells to contract and the heart to beat.
Electrical System
Even though they beat on their own, the electrical activity in each heart cell needs to be coordinated if the 4 heart chambers (atria and ventricles) are to pump an adequate amount of blood in the proper direction. Later on, when we talk about electrocardiograms, it is this electrical conduction we will be referring to.
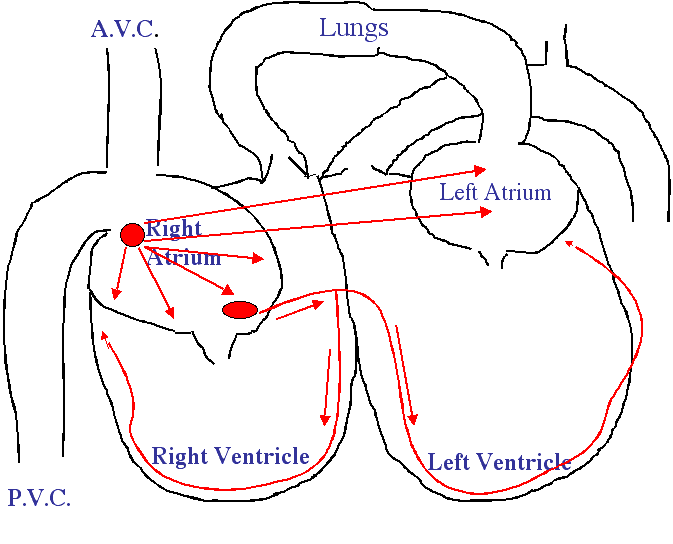
At the beginning of the right atrium there is an anatomical structure called the sino-atrial node (SA Node). It is the leftmost red circle on the diagram below. It is this area of the heart muscle that originates the coordinated beating of the heart. When this SA Node fires off it sends electrical impulses (the wires that carries these impulses are called perkinje fibers) through both atria, causing them to contract at the correct time.
One of the signals from the Sa Node also stimulates the atrio-ventricular node (AV Node) located at the bottom of the right atrium. Stimulation of this node stimulates nerve fibers that surround the ventricles, causing them to contract in a rhythmic way. There are other factors involved, especially hormones and other parts of the nervous system.
The atrio-ventricular bundle (AV bundle) is also known as the bundle of His in honor of the man who discovered it. Since the heart in a dog or cat beats approximately 2 times every second, these nodes have to fire off rapidly if everything is to stay coordinated. From the time the SA Node fires it takes only 0.22 seconds for the ventricles to contract.
The SA node is called the pacemaker because it depolarizes at a faster rate than any other group of cells in the heart, and imposes that faster rate on the heart as a whole. If for any reason the SA node stops beating, the AV node, which has the next fastest rate of depolarization, would become the heart’s pacemaker. If the AV node failed, the AV bundle would take over. If it failed, the Perkinje fibers would start the heartbeat, and if they failed as well, a group of cells somewhere else in the heart would start pulsing. However, the further away the heart gets from its normal pattern and rate of beating, the less blood it pumps and receives, until eventually it can no longer sustain Life.
Disturbances in the heart’s normal rhythm, known as arrhythmias, are a common problem in heart disease. Arrhythmias can be minor and unimportant, or severe and life threatening. There are many different kinds of arrhythmias, including:
Tachycardia – An abnormally fast heartbeat. If the hear beats too fast is does not spend enough time in diastole. Therefore the heart chambers do not fill up enough with blood, so the heart does not pump out an adequate amount of blood for the needs of the cells. In addition, the lack of time in diastole causes the heart muscle itself (myocardium) to suffer since it is in diastole that blood flows from the coronary arteries into the heart muscle.
Bradycardia – An abnormally slow heart beat. If the heart beats too slowly the blood pressure decreases and it does not generate enough flow of blood to the cells. One of the first signs of this is called syncope, which is the same this as passing out and becoming unconscious.
Heart block – Occurs when the electrical impulse has difficulty passing through the AV node.
Atrial fibrillation – When the atria contract in an irregular way and blood does not flow out of them effectively
Ventricular fibrillation – When the ventricles contract in an irregular and ineffective way, a condition which quickly leads to death unless corrected. This is a heart attack in people, and needs a defibrillator to correct the problem. People who have serious arrhythmia can sometimes have an artificial pacemaker implanted in their chest or abdomen. This battery powered device delivers a rhythmic electrical impulse to the heart on either a constant basis, or only when the heart’s natural pacemaker temporarily fails to sustain a normal beat.
You will learn more about the SA node and AV node in the electrocardiogram section to follow, so try to keep their jobs in mind.
Thoracic Anatomy (heart, lungs, blood vessels)
The normal mammalian heart has 4 chambers (birds also have 4, reptiles have 3). The 2 smaller chambers are called atria, the larger ones are called ventricles. The diagrams at the beginning of this page described the flow of blood through these chambers. Now lets see what these chambers and valves actually look like. Click here to review the diagrams at the beginning of the page if you need to.
The following are necropsy (the same as an autopsy in people) pictures showing how these structures actually look. They are done tastefully and should not bother you. It will be obvious from these pictures that the real anatomy is much more complicated than the diagram pictures. We will be emphasizing the left ventricle and mitral valve, since that is the area of the heart that causes most of the problem as dogs age. We will trace the flow of blood from the left atrium, through the mitral valve, and into the left ventricle.
Before we even get to the heart, there is a layer called the pericardium that surrounds it. In some diseases, fluid can buildup in between this outer layer and the actual heart muscle. This is the pericardium from a normal ferret. The fat at the bottom of this heart is normal.
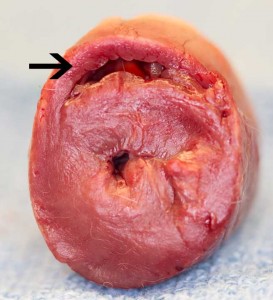
This picture shows mostly the inside of the left ventricle of a dog (its the same heart you saw at the very beginning of our heart page). You are looking into the chamber of the left ventricle. Note the thickness of the cardiac muscle (myocardium) surrounding the left ventricle, along with the smooth inner lining of the ventricle in the lower center of the picture. The lining needs to be smooth and relatively friction free for the red blood cells to flow through rapidly and not get ruptured or start clotting.
The tip of the metal hemostat (see arrow) just barely poking out is coming from the left atrium (not visualized), through the mitral valve, and barely into the left ventricle. This is the normal direction of blood flow as it comes out of the left atrium and into the left ventricle.
Let’s take a little closer look at the mitral valve. We have moved the hemostat a little further through the mitral valve in this next picture. Again, the left atrium is not visualized. The white filamentous structures are called chordae tendinae. When the blood flows through the mitral valve these chordae tendinae are relaxed since there is no pressure on them.
When the left ventricle contracts it exerts great pressure to get the blood through the aorta and to the rest of the body. This pressure pushes against the mitral valve, which is now shut since we do not want blood flowing backwards into the left atrium. It is these chordae tendinae that keep the mitral valve closed. A normal mitral valve can withstand this pressure, a diseased one cannot.

It is these strong chordae tendinae that prevent the blood from flowing back through the mitral valve into the left atrium. Remember this when we talk about mitral valve murmurs.
As we get even closer in the next picture you can see the leaflets of the mitral valve clearly (we removed the hemostat so you can see the bottom of the valve now). This thickened leaflet is called endocardiosis (you will learn more about this in the disease section when we teach you about chronic atrioventricular valve disease).
This thickening does not allow the valve to close fully, and blood regurgitates backwards into the left atrium when the left ventricle contracts. Since there is a huge difference in pressure (called a pressure gradient) between the left atrium and the left ventricle, this can have serious consequences.
This regurgitating blood is turbulent, and is the source of the heart murmur we hear with this disease. If the leakage is significant the pressure will cause the left atrium to enlarge (can be seen on a radiograph), with the potential for this added pressure to impede the flow of blood from the pulmonary vein.
If the blood in the pulmonary vein has a hard time flowing against this pressure in the left atrium, the plasma contained in the pulmonary veins will leak out of the capillaries and fill the lungs (the alveoli) with fluid. This is also called pulmonary edema, and is the “congestive” in congestive heart failure. Try to remember this when we discuss this in more detail later since it is an important aspect of chronic atrioventricular valve disease and congestive heart failure.

The top arrow points to a normal leaflet, the bottom arrow points to a thickened and shrunken leaflet
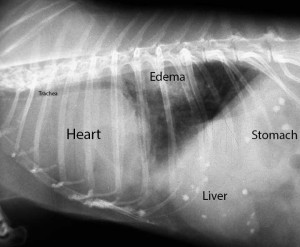
There are many other structures inside the chest (thorax) in addition to the heart and lungs. This next necropsy picture is from a dog. Before we show you the necropsy picture let’s get oriented using a chest radiograph.
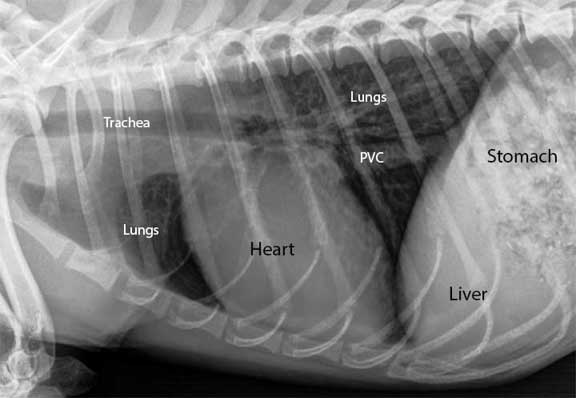
The dog is laying on its right side and the head is towards the left. This is the section of the thorax we will be looking at in the necropsy pictures to follow.
On the far right is the diaphragm (D), the muscle of respiration. It separates the thorax to the left of the diaphragm, from the abdomen on the right (the liver and stomach are just behind the diaphragm). The posterior vena cava (PVC) is visible as the horizontal blue structure at the bottom of the picture that is coming through the diaphragm. It is large because it has the job of returning almost all of the blood from the back end of the body to the heart.
The large horizontal pink structure above the posterior vena cava is the esophagus (E) as it goes through the diaphragm and enters the stomach behind the diaphragm on the right. It is not visible on the X-Ray above.
You can see one of the posterior lung lobes above and to the left of the esophagus. If you look closely you can also see a white nerve running horizontally along the esophagus (vertical arrow).
If you look even closer you can see a large white structure running horizontally just above the esophagus (horizontal arrow)- its the aorta embedded in tissue for protection.

With all of this anatomy packed into the thorax its a wonder we can even breathe at all!
The next picture is the same picture as the previous one, only viewed from the top and not the side. The head is towards the top with the dog laying on its back, the diaphragm (D) is at the very bottom. The structures are labeled the same.
Notice how much more lung is visualized. Look at the large veins to the lung lobes in the upper right. The posterior vena cava (PVC) is obvious as it runs vertically exiting the diaphragm at the very bottom of the picture and enters the right atrium at the top of the picture.
On each side of the vena cava are pink lung lobes, then the red esophagus (E), then the white aorta (A). Keep in mind these lungs are deflated. Think of how crammed this space is when the lungs are filled with air as we inhale. As a matter of fact, the negative and positive thoracic pressures that occur when we breathe have an influence on how this blood flows.

When normally inflated the lungs will fill the remainder of the thoracic cavity
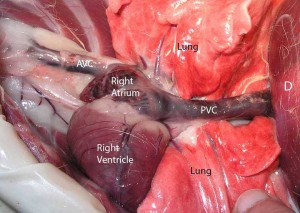
In the next side view picture we are shifted towards the left and away from the diaphragm and going closer to the heart. The head is still at the left. The heart is the dark blue structure on the top. The pericardium (lining of the heart) is still around the heart, so the heart is not as apparent as you might expect.
The right atrium cannot be visualized because the heart is covered with the pericardium. You can see the posterior vena cava (PVC) on the right as it enters the right atrium. The PVC returns venous blood from the back of the body to the heart.
You can also see the anterior vena cava (AVC) on the left as it also enters the right atrium. The AVC returns venous blood from the head and neck to the heart. You can also see a nerve as it runs horizontally on top of each vena cava.
Here is the feline version of the same area. In the first picture we are looking at the right side of the heart. The structures are smaller, but being a mammal, the anatomy is the same.
You cannot see the aorta in this view because the lung lobes are covering it
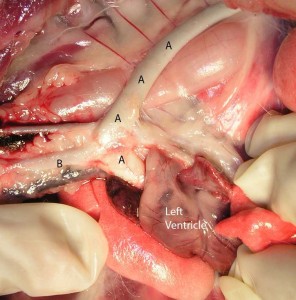
In this picture we have lilted up the heart and rotated it to the right, so now we can see the left side of the heart and underlying structures like the aorta (A)
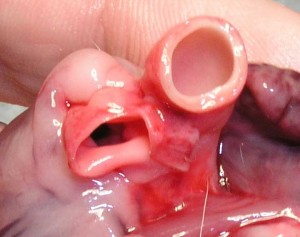
The walls of the aorta are much thicker that the pulmonary artery due to the added pressure of the blood as it is pumped out of the left ventricle. The pressure of the blood coming out of the right ventricle and going into the pulmonary artery is much less than the aorta, so the walls are not as thick
The opening to the pulmonary artery is on the left, the aorta opening is on the right.
Physiology of Heart Disease
The whole point of the cardiovascular system is to provide the individual cells in each organ an adequate flow of blood (called perfusion) that gives them the nutrients and oxygen they need. When these cells have what they need they can perform their normal function. So for the kidneys, that means they can filter out waste products. For the muscles, that means they can initiate movement. For the liver, that means that liver cells can metabolize drugs we put into the body. This adequate perfusion equates back to how much fluid the heart can deliver to these cells. an adequate cardiac output is needed for this perfusion.
There is a difference between heart disease and heart failure. In heart disease the heart has some type of abnormality. If minor enough, the heart is able to deliver adequate perfusion to the cells, and there is no problem. In heart failure, the heart does not maintain an adequate perfusion for normal cell function. Pets that are relatively inactive may be able to stave off the effects of heart failure longer than active pets because they do not challenge the cardiovascular system. This has a bad side though, because by the time the symptoms of heart failure are finally apparent to an owner, the disease is well entrenched and more difficult to treat.
If the right heart becomes diseased, a similar set of physiologic sequences occurs. The higher blood pressure that results when the cells send their emergency signals to the brain results in a greater amount of blood being presented to the right heart (increased preload). Eventually, the weakened right heart cannot pump blood into the lungs faster than the venous system is presenting blood to it. This causes back pressure to build up in the venous system, especially the vena cava and other veins in the abdomen and even thorax. When the pressure gets high enough in these veins fluid leaks out, leading to ascites and pulmonary effusion. This problem can occur in both hearts at the same time, causing even more problems.
If the left heart becomes diseased it does not pump an adequate amount of blood (decreased cardiac output) through the aorta for distribution to the cells of the body. This inadequate flow of blood ((poor perfusion) prevents these cells from performing their normal functions The brain monitors this perfusion, and goes into action by regulating hormones and sodium in conjunction with the kidneys and the lungs. This increases the pressure in the arterial system as a whole, and satisfies the needs of the cells temporarily by supplying them with a greater flow of blood (better perfusion).
This added blood pressure fills the diseased left ventricle with blood more than usual (increased preload), causing it to dilate and weaken further. It also increases the pressure the left ventricle has to pump against (increased afterload) to get the blood through the aorta and into the cells. These add further work to an already diseased heart, compounding the problem even further. Eventually, the blood presented to the left ventricle does not get pumped out effectively, which causes a back flow (added pressure) in the lungs. When the pressure reaches a certain point the fluid in the blood vessels in the lungs leaks out, causing pulmonary edema. This is congestive heart failure (CHF).
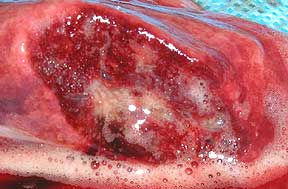
This white frothy fluid is severe pulmonary edema. It is a cut section of the lung of a cat that died from cardiomyopathy
A pet that cannot breathe well due to pulmonary edema (fluid in the lungs) is in a panic situation. It needs to be handled very gently, so the first thing we do is put it in 100% oxygen until it calms down. Only then do we attempt to diagnose and treat it.
A pet that cannot breathe well is a medical emergency requiring immediate veterinary care. They can collapse and go into life-threatening shock. The Long Beach Animal Hospital, staffed with emergency vets, is available until the evenings 7 days per week to help if your pet is having any problems, especially shock, seizures, pain, difficulty breathing, or bleeding.
Think of us as your Long Beach Animal Emergency Center to help when you need us for everything from minor problems to major a major emergency. We serve all of Los Angeles and Orange county with our Animal Emergency Center Long Beach, and are easily accessible to most everyone in southern California via Pacific Coast Hwy or the 405 freeway.
If you have an emergency that can be taken care of by us at the Animal Emergency Hospital Long Beach always call us first (562-434-9966) before coming. This way our veterinarians can advise you on what to do at home and so that our staff and doctor can prepare for your arrival. To learn more please read our Emergency Services page
Cause of Heart Disease
There are several factor, usually working in combination, that lead to cardiac disease:
Bacteria
They can buildup on the heart valves inhibiting their ability to flow blood in the proper direction through the heart. This is a particularly important cause of heart disease since so many pets have severe enough dental disease that the bacteria in their mouth number in the billions. These bacteria can go into the bloodstream at the base of the tooth and invade the heart and its valves. Our dental page talks about this in more detail.
They can buildup on the heart valves inhibiting their ability to flow blood in the proper direction through the heart. In almost all cases in dogs and cats this is from dental disease.
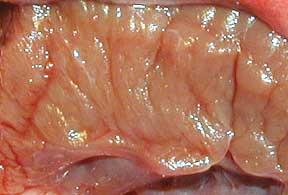
This is periodontal disease in a cat. The bacteria that are in the inflamed area of the gums are in the millions, and can spread to the bloodstream and go to the heart valves.
Virus
They can directly affect the heart muscle (myocardium), causing cardiomyopathy. In the early years of parvo virus there was a form of the disease that attacked the myocardium and caused rapid death.
Amino Acids
Taurine, an essential amino acid in cats, can lead to dilated cardiomyopathy. Humans and dogs can produce taurine naturally (non-essential) and do not need it in their diet. A deficiency of taurine in the cat will also cause degeneration of the retina. Taurine was not included in adequate amounts in cat food many years ago. This problem has been corrected in almost all commercial cat foods, so we rarely see this problem anymore.
Hypothyroidism
An inadequate amount of the thyroid hormone thyroxin can predispose a dog to heart disease. This problem is diagnosed with a blood sample and corrected with thyroxin hormone replacement. This problem is almost exclusively seen in dogs.
Hyperthyroidism
This cat problem occurs when the thyroid gland has a tumor and secretes excess thyroid hormone (thyroxin). You can learn about it in detail in our hyperthyroidism page. In this disease the heart is racing as it tries to keep up with the increased metabolic rate of the organs as they respond to the increased thyroid hormone.
Valve Disease
Congenital abnormalities of the heart valves, usually a problem in young dogs, can lead to significant heart disease. These can include any of the valves. We get an indication of this early in a pets life by the presence of a heart murmur. Young animals can have what are called “innocent murmurs”. These are heart murmurs that don’t cause any problems and eventually resolve. If these murmurs persist, are of high intensity, or the pet is ill, they should be pursued further with diagnostic tests.
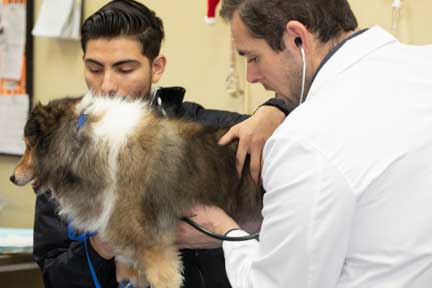
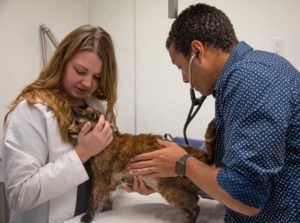
Heart murmurs are diagnosed with a stethoscope. One of our student externs is learning about the three heart valves that can be ausculted on the left side of the chest. The three valves are the pulmonic, aortic, and mitral valves.
Older dogs get a problem with heart valves that also can be significant. We will go into this in more detail soon because it is the most common cause of heart disease in the dog.
High Blood Pressure
This tends to be secondary to some diseases, most notably kidney disease and hyperthyroidism. We have a page on hypertension (high blood pressure) that goes into this problem in more detail.
Drugs
Some drugs are toxic to the heart. It is ironic that one of the drugs used to treat heart disease, called digitalis, can be toxic to the heart also. This drug is commonly used to help slow down a racing heart. When used, we monitor digitalis levels with a blood sample at least every l6 months to make sure it does not go into the toxic range.
Trauma
A heart that receives a severe blow can have problems with adequate pumping of blood or the normal electrical beating.
Parasites
The heartworm parasite (dirofilaria immitis) can cause severe heart disease. This problem is not uncommon in dogs, and has been diagnosed with increasing frequency in cats lately.
Lung Disease (cor pulmonale)
Problems with hypertension in the lungs can cause the right heart to fail. These problems can include cancer, heartworms, infections, trauma, toxins, hypothyroidism, and Cushing’s disease.
Metabolic Disease
When vital internal organs like the kidney and liver are diseased there can be many changes that effect the heart. These include electrolyte abnormalities, calcium irregularities, and waste product buildup.
Toxins
Some poisons selectively target the heart. Curare, the drug used in the tips of poison arrows and darts, is one of these drugs.
Symptoms of Heart Disease
Typical symptoms of cardiac disease include:
- lethargy
- poor appetite (anorexia)
- coughing- initially caused by an enlarged heart pushing upwards on the mainstem bronchi (windpipe) when the left atrium enlarges. As time goes on, this coughing is exacerbated by fluid buildup in the lungs (pulmonary edema).
- passing out (syncope)
- weakness
- difficult breathing (dyspnea)
- distended abdomen (especially if the right heart is diseased) called ascites
- pale or bluish colored gums (cyanosis)
- racing heart (tachycardia)
These symptoms are found in many other diseases also, especially of the respiratory tract. To determine which disease is causing these symptoms we need to strictly adhere to the diagnostic process.
In some heart diseases, notably cardiomyopathy in cats, there might be no symptoms prior to a sudden death. These cats seem fine until a stress causes their diseased yet compensating heart to reach its limit.
Physical Exam
Several abnormalities might be noted in an animal with a heart problem. Most of these are due to poor perfusion of the target organ or fluid buildup due to changes in preload and afterload.
Difficult breathing or coughing due to fluid buildup in the lungs (pulmonary edema) or thoracic cavity (pleural effusion). This can be picked with the stethoscope during auscultation (listening to) of the heart and lungs. The term we use for an increased in lung sounds due to pulmonary edema is called rales.
Pale or bluish mucous membranes (cyanosis or anemia). This is noted when we look at your pet’s gums. Capillary Refill Time (CRT) might be prolonged.
This video shows how we check the CRT
Distended abdomen (ascites) due to back pressure of blood not flowing from the back of the body into the right heart properly. This makes pets uncomfortable and difficult to breathe with the added pressure on the diaphragm.
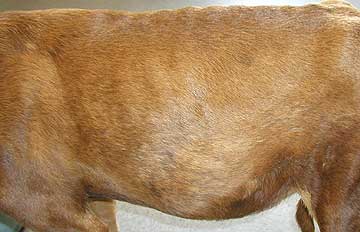
This Doberman with heart failure shows the typical appearance of a distended abdomen caused by ascites. There are other diseases that can cause this look, including Cushing’s disease.
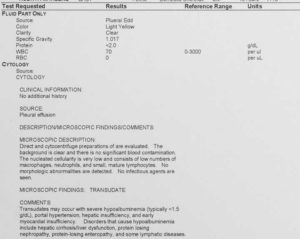
We tap the fluid off to make it much easier for this dog to breathe and also to analyze it and make sure there are no cancer cells. We will also pull this fluid off when it occurs in the chest, called pleural effusion.
This is a typical report we get when we analyze pleural effusion fluid on a dog with heart disease
Distended jugular veins due to back pressure of blood not flowing from the head to the right heart properly. Right heart failure can be a cause of the ascites you just learned about.
This short movie shows distended and pulsing jugular vein
Pulse deficit- a lack of synchrony between the beating heart and the pulse. This is detected with a stethoscope and palpation of the femoral artery.
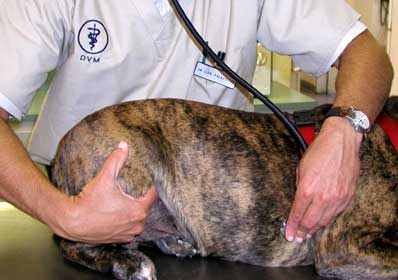
An increased heart rate (tachycardia)
A heart murmur during auscultation with the stethoscope
Cool extremities to the touch
Reduced mental capacity
Diagnostic Tools
Blood Panel
Many pets with heart failure are senior pets, so it is common for us to run a routine blood panel. There are no specific blood panel tests that diagnose heart disease in dogs and cats, although we can see indirect evidence of heart problems and their consequences sometimes. Also, the blood panel lets us assess problems in important organs like the kidney and liver that can occur simultaneously with heart disease in senior pets. This becomes important when we use medication to treat heart disease.
Thyroid Test
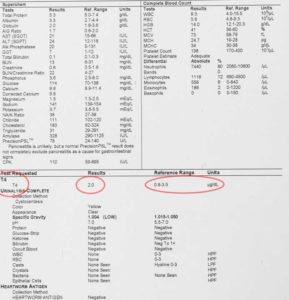
Our lab routinely performs a thyroid test on the blood panel for senior pets since a low thyroid level can be a cause of heart disease. This disease is called hypothyroidism, and occurs in dogs. A high level of thyroid hormone, called hyperthyroidism, occurs in cats, and can also cause heart problems. All pets 8 years of age or older should be checked for this hormone imbalance on a yearly basis.
The thyroid level is important in many diseases, so it automatically included in our full blood panel. It takes a special lab to be able to monitor a hormone that is measured in micrograms per deciliter (see reference range in report above).
Stethoscope
A very important tool in the diagnosis of heart disease is the stethoscope. This simple yet elegant instrument allows us to hear the valves of the heart as they open and close, and also to hear the rhythm of the heart as it contracts. The name stethoscope comes from the Greek word “to spy on the chest”. It was designed in 1816.
We work with a wide variety of species, so we use different stethoscopes depending on the size of the pet. Each stethoscope has 2 different sized diaphragms, allowing us to hear heart sounds of different frequencies.
Animals have a normal arrhythmia, called sinus arrhythmia. This arrhythmia is an alternation in the rhythmic beating of the heart that coincides with breathing. This can easily be heard with the stethoscope. It is perfectly normal, yet does not occur in humanoids.
The stethoscope really comes into play for an animal that has a heart murmur. A heart murmur is a turbulence of blood flow as it goes through the heart valves (mitral or tricuspid). In a perfectly normal heart the blood flows past the valves silently, and all we hear with the stethoscope is the rhythmic lub-dub of the heart valves as they open and shut. If a murmur is present there is a whooshing sound mixed in with the lub-dubs, almost like the sound of a washing machine. Click on the heart murmur link above to hear a murmur.
This murmur is caused by blood becoming turbulent as it passes through an abnormal heat valve, although other problems can cause a murmur, the most notable being anemia. As we stated earlier, young animals can have an innocent murmur that resolves on its own and does not cause any problems.
Heart murmurs are graded from 1 to 6. One is barely audible with the stethoscope, 6 is so loud that you can feel the murmur with your hand on the chest (the technical word for this is a thrill oddly enough). In general, the louder the murmur the more significant the disease, although this does not apply in all cases. Mitral murmurs tend to be louder due to the large difference in pressure (pressure gradient) between the left atrium and left ventricle.
In addition to their loudness, murmur have other audible characteristics. The sound can increase or decrease in intensity, a term we call crescendo or decrescendo. Murmurs that do not change in intensity are called holo.
This rabbit is getting its heart checked by Dr. Wood as part of a pre-anesthetic exam before being neutered with our laser
It takes many years of practice to properly auscult the heart with a stethoscope on small animals that are not cooperative and have rapid heart rates (not to mention that also purr a lot)! This is our cardiologist Dr. Fred Brewer showing one of our students how to listen to this cat’s heart.
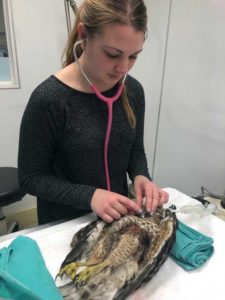
Even though it is a challenge to properly auscult the heart of a dog that is panting or a cat that is purring, their heart rates, although high compared to humanoids, are slow compared to an avian heart. A bird heart routinely beats well over 300 times per minute.
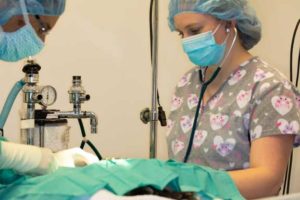
We use the stethoscope almost continuously in surgery to monitor anesthesia
If you get a chocolate bunny at Easter you can practice your auscultation skills!
Electrocardiogram (EKG or ECG)
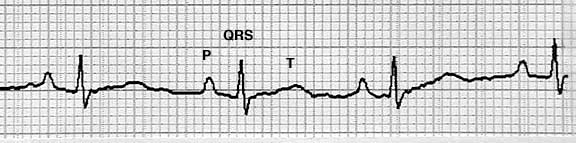
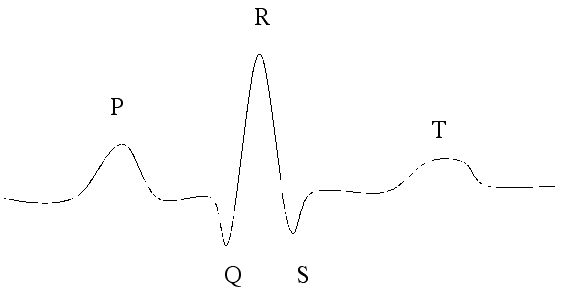
As you already learned cardiac muscle (myocardium) is unique in its rhythmic beating. This rhythm is analyzed with an electrocardiogram. What the EKG measures is the depolarization (losing their electrical charge) and repolarization of the heart muscle as the cells contract. We talked about the mechanism of this in the cardiac muscle section in regard to sodium, potassium, and calcium. The EKG line that is produced measures the direction of the electrical activity along with its magnitude. Since the atria are smaller in size than the ventricles, their magnitude on the EKG strip is smaller.
What an EKG report looks like
The hardest part about performing an EKG on an animal is keeping it still enough to get a good reading. Sedatives are not used since they can interfere with the results. Interpreting the EKG is a medical art, and requires the familiarity of the electrical differences of many different breeds of dogs and cats.
If our cardiologist is not available we use a service that allows us to transmit the ECG through the telephone or via fax to a group of veterinary cardiologists that specialize in EKG’s. In addition to interpreting the EKG, they also give us a cardiac consultation via fax the next day (or within a few minutes if it is an emergency).
Our cardiologist, Dr. Fred Brewer, does his EKG’s on a computer
We use the EKG in several situations. The first is for a dog or cat that is older or might have the symptoms of heart disease, especially coughing. We also use it prior to any anesthesia in high risk pets or when there is significant concern about anesthesia in general . We have a complete page on anesthesia to learn more.
An EKG alone cannot determine if heart failure is present. It can be helpful in determining that heart failure is not present. We need other information from the Diagnostic Process, along with an echocardiogram, which you will learn about later in this page.
This EKG is from a pet that stayed still long enough for us to get a reading. It shows almost 4 complete beats of the heart.
We enlarged one of the 4 beats to help when we explain below
We use the ECG in several situations. The first is for a dog or cat that is older or might have the symptoms of heart disease, especially coughing. We also use it prior to any anesthesia in high risk pets or when there is significant concern about anesthesia in general . We have a complete page on anesthesia to learn more.
Radiography
An excellent tool in the diagnosis of heart disease is radiography. The size of the heart and pulmonary vessels, along with fluid buildup in the lungs, can be seen in a radiograph. We will show you some normal radiographs first, then some abnormal ones. You might one to come back to the normal ones to refresh your anatomy as you view the abnormal ones. Before we get to the radiographs lets review some thorax anatomy
You might want to do a more detailed review at our heart anatomy page
We will also show you radiographs of pets with breathing problems that are not the result of heart disease. This shows the importance of radiography in diagnosis, and emphasizes the need to follow the diagnostic process at all times. Don’t forget that changes in the lungs can eventually cause the right heart to fail (cor pulmonale).
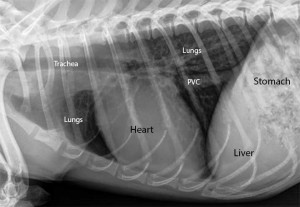
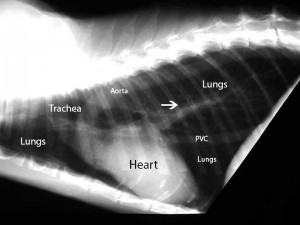
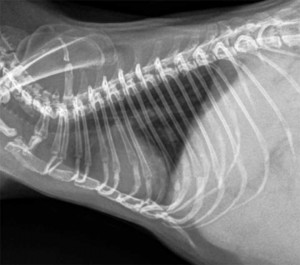
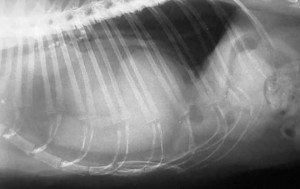
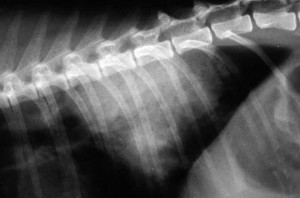
Normal dog heart and lungs side view (called a lateral view). The head is towards the left. The trachea is in the correct location and is of the proper size. The dark lungs are readily visible along with the normal sized heart. PVC is posterior vena cava.
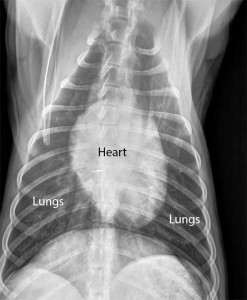
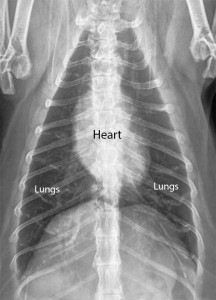
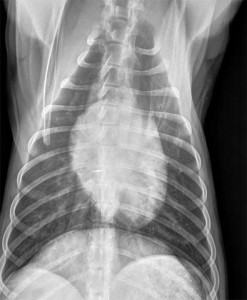
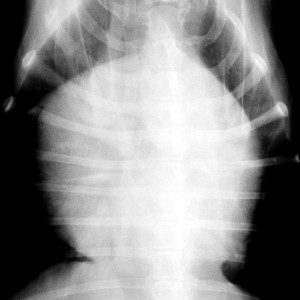
Normal dog heart and lungs top view (called a DV (Dorsal-Ventral) view). The heart is the correct size, and it is surrounded by normal lung tissue. The lung tissue is black because it is filled with air. The white semicircular area at the bottom is the diaphragm.
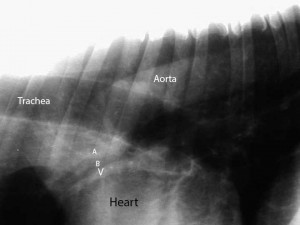
There is significantly more information in a chest radiograph than just the trachea, heart and lungs. In this radiograph you can see the aorta along with an artery (A), bronchus (B), and vein (V) to the cranial lung lobe. Changes in the size of these veins and arteries give us clues as to whether heart disease is present along with the cause of the heart disease.
An even close view of the artery (A), bronchus (B), and vein (V)
Normal cat heart and lungs side view. You can see the same structures as the dog radiograph. Do you see the artery, bronchus, and vein to the cranial lung lobe? They are smaller than the dog, but they are present. Do you also see the posterior vena cava? The arrow points to it.
A normal cat from the top view (DV). Its not easy to get a cat to sit still to take this radiograph!
We work on all different kinds of critters that get heart disease. This ranges from ferrets, to rabbits, to guinea pigs to rats. They all show different symptoms, and it is not easy to diagnose them in these species
This is a ferret chest radiograph
Guinea Pig chest radiograph
An enlarged heart is called cardiomegaly. There are several parameters we use to give us an indication a heart is enlarged. These parameters are variable, and depend heavily on the breed of dog. We will show you a dog with heart disease. We put a normal heart radiograph first for comparison.
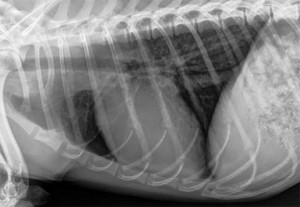
This dog in the following radiographs has a very large heart (cardiomegaly). Not all pets with heart disease show such obvious and extreme changes. Many changes are subtle, and do not show up well on a web site at low resolution, so an extreme one is used for better understanding. We would hope to see a dog like this long before the radiograph progressed to this point.
This is a normal dog chest radiograph to help in visualizing the dog with the heart problem below
The radiographic diagnosis is elevated trachea, mainstem bronchus compression, loss of caudal waste, loss of cranial waste, pulmonary edema, and increased sternal contact
Normal dog DV view for comparison to radiograph below
The heart is much larger due to the heart failure
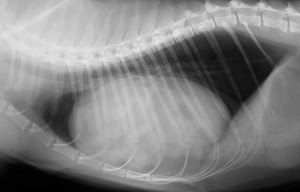
Not every enlarged heart (cardiomegaly) on a radiograph is a sign of heart disease. This cat has an apparently enlarged heart with an elevated trachea. In this case it is caused by a diaphragmatic hernia, where the liver has literally torn through the diaphragm and resides in the thorax.
Sometimes the hernia is not so apparent, and makes it look just like an enlarged heart
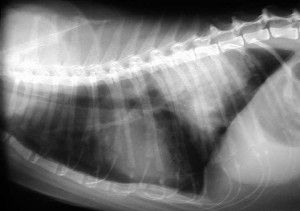
Radiographs are also used to diagnose pulmonary edema, which is fluid buildup within the lungs themselves. It is a sign of congestive heart failure. All the whitish area at the the top right of the lungs is the fluid. Normally this area should be black because it is filled with air.
This is a large amount of pulmonary edema
A close up of the edematous (fluid filled) area in the lungs
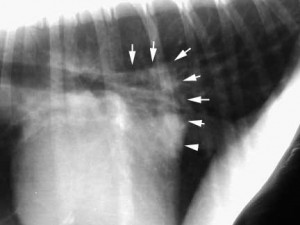
When the left atrium is enlarged it is also a sign of heart failure. We can see an enlarged left atrium radiographically if it is large enough.
The arrows point to a very enlarged left atrium at the arrows
The previous radiograph changes of pulmonary edema (congestive heart failure)were due to failure of the left side of the heart (left atrium and left ventricle). If the right side of the heart goes into failure, the radiograph might show fluid in the abdomen and no changes in the thorax. Fluid the builds up in the abdomen is called ascites.
Draining ascites fluid from an abdomen of a dog with right sided heart failure
Heart disease is not the only problem that can cause ascites. Several other conditions can give this radiographic appearance, especially FIP in cats and cancer.
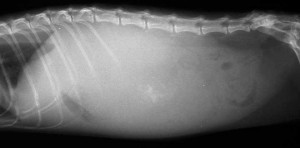
This cat has ascites, which is fluid buildup in the abdomen. If you compare it to the radiograph below it you can see that individual internal organs are not visualized. This is because the organs are surrounded by fluid. The dark areas are air in the stomach and in the intestines.
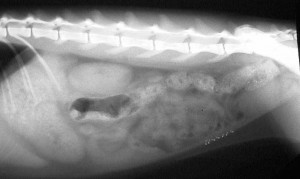
This normal cat abdominal radiograph shows all the distinct internal organs for comparison to how the fluid above obscures them
Time for a break from all this radiology stuff. Let’s look at something fun. It is the beating of the heart of a tortoise that is undergoing bladder stone surgery.
Click on the video and enjoy the beat.
Echocardiogram
An echocardiogram of the heart is almost indispensable in detecting a significant number of heart problems. Echocardiography refers to the imaging of the heart with ultrasound. Echocardiography may be divided into three types based on the instrumentation and application. These are M-mode, Two-dimensional, and Doppler Echocardiography.
M-Mode
This image is useful to measure the thickness of the ventricular walls along with size of the cardiac chambers. With these measurements a formula is used to determine cardiac contractility.
Two Dimensional
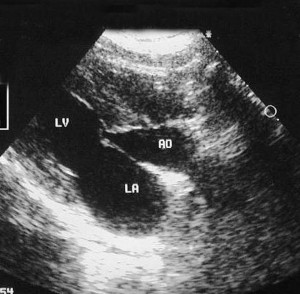
This image gives us an overall view of the heart. We can look into the chambers and see the valves in action. We can also see fluid around the heart if it is present.
This ultrasound picture shows the left ventricle (LV), aorta (AO) and left atrium (LA)
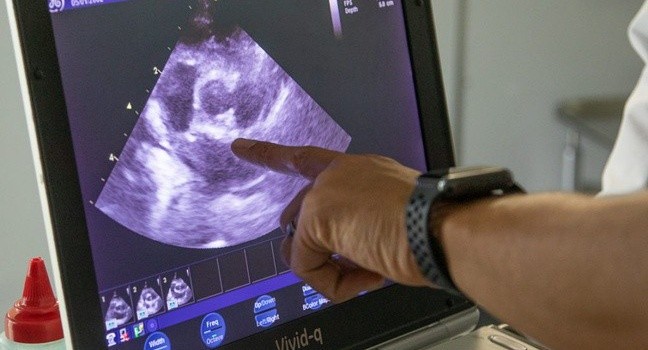
Echocardiograms require the expertise of an expert. In this photo our cardiologist Dr. Fred Brewer is teaching one of our student externs.
He is pointing out the valves between the chambers of the heart
After many calculations are performed this is the report we get
Doppler
The Doppler view allows visualization of the blood as it literally flows through the heart. It is usually performed simultaneously with the Two Dimensional image. It can sometimes help us detect the degree of valvular disease by measuring the speed at which the blood flows through the abnormal valve.
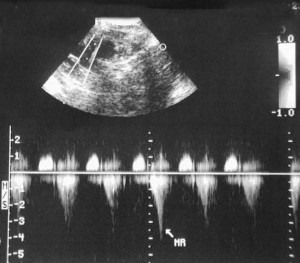
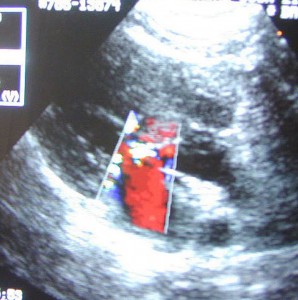
In the top half of this ultrasound picture the 2 parallel running vertical lines are the doppler measuring the blood flow through the mitral valve. The “MR” at the bottom half of the picture is the doppler measuring the intensity of the mitral regurgitation that is occurring.
The color doppler makes it easy to visualize the blood flow through the heart valves
Click on the movie below to watch the color doppler in action (and listen to our cardiologist talk to one of our students). Notice how fast this heart is beating. Remember our earlier lesson on heart failure, and one of the ways the body adapts to a heart that is not pumping enough blood is to increase the heart rate. That is occurring in this case.
The Doppler Echocardiogram allows visualization of the blood as it flows between the chambers of the heart
Heart Diseases And Their Treatment
This are several common heart diseases encountered in dogs and cats. This page will cover the diagnosis and treatment of chronic valve disease and cardiomyopathy:
Chronic valve disease
Cardiomyopathy
Heartworm
Aortic Stenosis
Pulmonic Stenosis
PDA (Patent Ductus Arteriosis)
Medical Treatment of Heart Disease
Chronic Atrioventricular Valve Disease (Myxomatous AV Valvular Degeneration)
This disease goes by several names. They include endocardiosis, mucoid valvular degeneration, chronic valvular fibrosis and acquired mitral regurgitation/insufficiency. It is the most common cause of heart disease and congestive heart failure (CHF) in the dog. Tricuspid valve regurgitation can also occur with this disease. It is rarely seen in cats.
Cause
The exact cause is unknown. It effects the mitral valve more commonly than the tricuspid valve, although both can be involved. It probably affects the mitral valve more commonly because of the high pressure in the left ventricle. As dogs age nodules form along the edge of mitral and tricuspid valves. When they get thicker the valves begin to leak (regurgitation), and as the disease progresses, the valves become deformed and shrink. You saw this previously in the necropsy pictures of the dog heart. As the problem progresses the chordinae tendinae might even rupture.
As the blood regurgitates abnormally backwards into the left atrium it increases the pressure in the atrium, making it harder for blood to flow from the lungs into the heart (from the pulmonary vein to the left atrium). As the back pressure increases, the pressure in the veins of the lungs increases to a point (pulmonary hypertension) where the fluid leaks out, leading to pulmonary edema.
This regurgitating flow of blood through the left atrium eventually causes it to enlarge (you saw this in the radiograph pictures). The regurgitating blood can go from the left ventricle through this valve and into the left atrium with such force that it causes “jet” lesions in the wall of the left atrium. The left atrium might also develop an arrhythmia as it continues to dilate. The enlarging left atrium can actually tear and cause blood to leak within the pericardial sac.
Since some of the blood that would normally be ejected by the left ventricle is now regurgitating back into the left atrium there is less flow of blood out of the left ventricle and into the aorta. This can begin the process of poor perfusion, leading to the cascading series of events culminating in congestive heart failure (CHF). Not every case of chronic atrioventricular valve disease will lead to heart failure though. Some dogs can have thickened and deformed valves and never show any symptoms.
To review all of this again in more detail follow our Heart Anatomy & Physiology Page.
Signalment
It usually occurs in smaller breed dogs, notably:
Poodles
Miniature Schnauzers
Fox terriers
Cavalier King Charles spaniels
Lhasa apso’s
Shetland sheepdogs
History
Symptoms might include exercise intolerance, weakness, syncope (passing out), cough, shortness of breath, and lethargy. Some pets have no symptoms
Physical Exam
A heart murmur along with an arrhythmia is a clue to this disease. As the problem progresses the murmur becomes louder. In the later stages of the disease the fluid that builds up in the lungs (pulmonary edema) can be heard with the stethoscope also. Fluid in the abdomen, called ascites, could also occur. In cat there might be general fluid in the chest surrounding the lungs called pleural effusion.
An irregular rhythm and increased heart rate might also be present as the disease progresses. In the early stages of this disease there might not be any abnormalities on the physical exam.
Diagnostic Tests
Blood samples are usually normal if only the heart is having a problem. Since these are geriatric patients usually, a blood sample is still indicated to check for other problems in pets this age.
Radiographs are used commonly to help in the diagnosis. The left atrium is enlarged, and sometimes the left ventricle. We might also find enlargement of the pulmonary veins and even evidence of pulmonary edema.
An echocardiogram can also give us significant information. The abnormal valves can be seen, along with rupture of the chordae tendinae in some cases. The doppler can actually view the blood regurgitating through the abnormal valve. The left ventricle might also be enlarged.
Our cardiologist Dr. Fred Brewer is pointing to a heart valve on this echocardiogram
This is what mitral regurgitation looks like during a doppler echocardiogram
In the early stages the ECG might be normal. As the problem progresses arrhythmia’s might be present
Treatment
Surgery and balloon catheter dilation are helpful but may be of limited value. Medical therapy is used to treat this problem if it progresses to CHF.
Medical therapy is utilized to slow the progression of the disease (minimize the compensation mechanism we describe earlier), control the fluid that builds up in the lungs, and decrease the heart rate as the problem worsens. The advent of ACE inhibitors (afterload reducers) has given us the opportunity to help slow the progression of this incurable problem.
Therapy might depend on the stage of the disease. If there is a murmur in one of the affected breeds, but the left atrium is not enlarged, then minimizing sodium (salt) in the diet might be of help. As the murmur intensifies and the left atrium enlarges we will start Enalapril, and continue with the low sodium diet. As the murmur intensifies and the problem progresses we might increase the dose of Enalapril.
Pimobendan is of significant help to the heart
When a cough appears lasix will be used, and even a beta adrenergic blocker. If pneumonia occurs or other lung
Prognosis
Mildly affected dogs can have a good quality of life for years. It all depends on when the diagnosis is made and when therapy is instituted.
All dogs on therapy for CHF should be monitored every 3-6 months to adjust for changes. This includes a blood panel with thyroid, a chemistry panel, ECG, and chest radiographs.
Chronic atrioventricular Valve Disease can mimic infectious endocarditis, which is an actual infection of these valves caused by a bacteria. This is a serious disease that can cause significant illness.
Some of the more common bacteria are:
E. coli
Strep spp.
Staph spp.
Pasteurella
Klebsiella
These bacteria arise from infections of the gums, skin, urinary tract, prostate, lungs, and internal organs. The infection can spread to the spinal cord, causing a disease we call diskospondylitis. It is treated the same way, since CHF is present. In addition we will use antibiotics for up to several months to control the infection.
Cardiomyopathy
Cardiomyopathy is a disease where the actual heart muscle (myocardium) becomes weak and unable to contract with sufficient force (decreased contractility leading to a decreased stroke volume) to provide adequate perfusion (reduced cardiac output) for the cells of the body. Pets that get cardiomyopathy have a poor prognosis in general.
There are three types of cardiomyopathy:
Dilated
The heart muscle is weak and flabby, and does not have the strength to contract with enough force to provide adequate perfusion of the cells. This form is rare in cats now because of supplementation with Taurine.
This is the heart of a cat with this disease. The forceps are pushing on the ventricles and showing how flabby they are.
Hypertrophic
The heart muscle has become so thickened that the left ventricle chamber is too small to allow an adequate amount of blood to flow into it (diastole) before it contracts (systole) and perfuses the cells of the body. It is like a bodybuilder who is too buff to move efficiently.
This is the form of the disease that is prevalent in cats. The heart muscle might hypertrophy due to hypertension or problems with the outflow tract of the aorta.
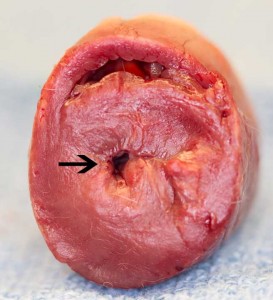
The bottom tiny opening (arrow) is the left ventricle surrounded by excessive thickened heart muscle. The opening should be 4x this size. You can see it is just too small to hold enough blood to be pumped out of the aorta to the cells of the body.
This increase muscularity of the left ventricle increases pressure in the left atrium, causing it to dilate. This increases the pressure in the pulmonary veins leading to pulmonary edema. Pulmonary edema (congestive heart failure) is fluid in the lungs, and is a serious end consequence of cardiomyopathy.
This arrow points to the dilated left atrium, which is 2x larger than it should be
Restrictive (Intermediate)
This form has characteristics similar to dilated and hypertrophic. Cats with this problem have scar tissue instead of normal heart muscle. The scar tissue decreased the strength of the heart, so it pumps out less blood at each beat (decreased stroke volume).
The diseased heart muscle beats irregularly (arrhythmia) and does not have the contractility to pump blood to the rest of the body (decreased cardiac output). This leads to the congestive heart failure we described in the pathophysiology section. In some cases there is sudden death from the arrhythmia that occurs.
Cause
Viruses, toxins, drugs, and taurine deficiency are suspected as causes. In most cases, especially in the breeds that are prone to this problem, the cause is unknown.
Signalment
This disease occurs in large breed dogs like the Great Dane, Labrador, German Shepherd, St. Bernard, Irish wolfhound, English cocker spaniel, Scottish deerhound and Boxer. It is especially prevalent in Doberman pinschers. Most of these dogs are males and get the dilated version of cardiomyopathy.
Even though dogs of any age can get this problem, the tend to me middle aged. Dilated cardiomyopathy also occurs in Burmese, Siamese, and Abyssinians.
History
The symptoms noted are those of congestive heart failure (CHF). Typical symptoms include weakness, poor appetite (anorexia), cough, breathing difficulty (dyspnea), weight loss collapse (syncope) and distended abdomen (ascites). In some cases sudden death occurs before any symptoms.
Some Doberman pinschers can have this disease and not show symptoms for several years. By then the prognosis is poor.
In cats the symptoms are similar. Unfortunately, a significant number of cats do not show any symptoms, they just have a sudden death. Cats also get paralyzed in their back legs because of a blood clot (thrombus) that enters the blood vessels to the back legs. This is called a “saddle thrombus” because it occurs at the point where the abdominal aorta branches into each of the arteries that supplies the rear legs with blood.
The blood clot arises from the pooling of blood that occurs in the left atrium secondary to the hypertrophy of the left ventricle (described above in the hypertrophic section). These cats are in significant pain, and palpation of the rear legs might reveal a cooler temperature than the rest of the extremities. The prognosis is poor for this form of feline cardiomyopathy.
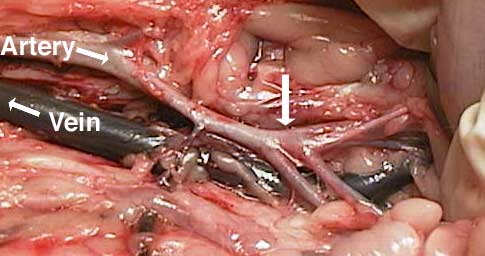
To get you oriented for the following pictures, this cat’s head is towards the left and the back legs are towards the right. Blood coming from the heart flows down the abdominal aorta (labeled as artery in this picture) and towards the rear legs. At the vertical arrow the abdominal aorta branches into the internal and external iliac arteries.
From there it goes into the femoral arteries to supply the rear legs with freshly oxygenated blood. The poorly oxygenated blood returns to the heart through the femoral vein, then the iliac veins, and eventually the caudal vena cava (labeled as Vein in this picture). At the vertical arrow is where the saddle thrombus forms.
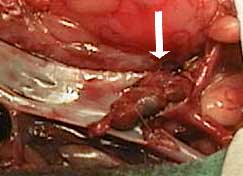
The white arrow points to where the blood clot forms
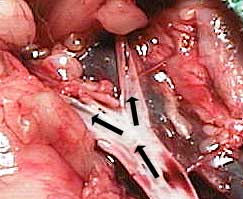
The thrombus (vertical white arrow) is apparent when the artery is opened up
This is the way the artery is supposed to look when there is no thrombus
The removed blood clot. You can see why it is called a “Saddle Thrombus”
Physical Exam
Abnormalities found during an exam are similar to other heart diseases and even other diseases in general. Auscultation of the thorax might reveal an arrhythmia and high heart rate. There might even be a pulse deficit if atrial arrhythmia is present. a murmur might be found in some pets with cardiomyopathy, although not every pet with a murmur has this disease.
Cats with a saddle thrombus might have weak or non existent femoral pulses. They will be painful and might not be able to use the rear legs.
Diagnostic Tests
The ECG can pick up arrhythmia’s caused by cardiomyopathy, in some cases prior to the onset of congestive heart failure. In breeds that are highly prone to this problem like the Doberman pinscher, it is advised to perform an ECG yearly to monitor for these changes.
On a radiograph the heart will appear enlarged because of the dilatation of all the chambers. Pulmonary edema and congested veins are indications of congestive heart failure secondary to cardiomyopathy. Some Boxers with cardiomyopathy will have normal appearing hearts on a radiograph.
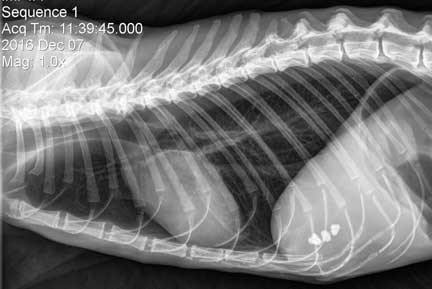
The first X-Ray is from a normal cat, the second is from a cat with heart failure.
You can distinctly see the white heart and the black lungs. Those 3 white areas to the right (in the abdomen) are stones in the gall bladder.
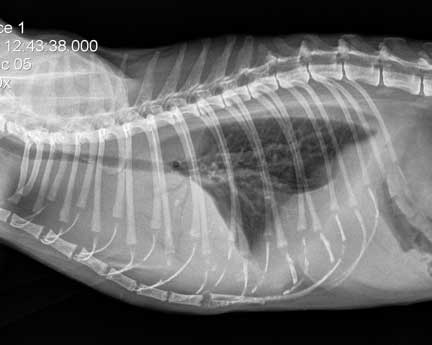
This cat has pleural effusion due to heart failure. There is fluid in the chest obscuring the heart and causing the caudal lung lobes to collapse.
There is a lot more to reading a radiograph than this. If you visit our How To Read A Radiograph Page you can learn even more.
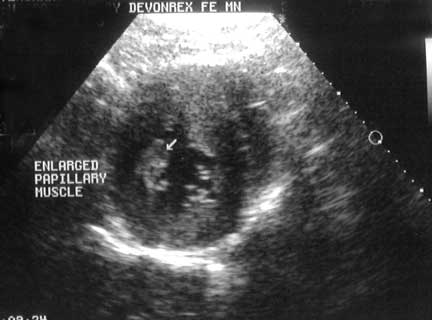
An echocardiogram is the gold standard for diagnosing HCM and heart failure. This is an echocardiogram of the cat with the enlarged heart above. . We could even visualize the blood swirling around as it formed a pre-clot that would eventually become a thrombus and expelled from the ventricle to large in some artery in the body.
The echocardiogram showed an enlarged papillary muscle in the ventricles
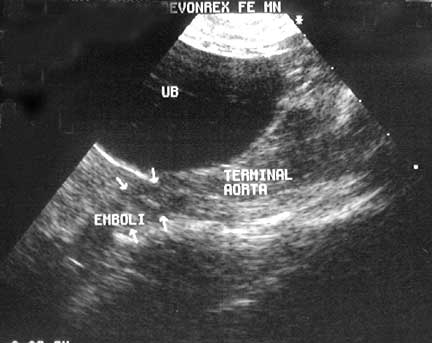
We could even visualize the thrombus at the end of the aorta just before it branches into the iliac arteries
These are the calculations made during an echo to determine if a heart is having a problem
This is the final report from our cardiologist on a cat with HCM (Hypertrophic CardioMyopathy)
Treatment
Routine treatment for congestive heart failure and arrhythmias is used. The effectiveness of therapy depends on the severity of the disease and how long the problem has been present. Some dogs and cats can do well for several months and even years if treated early enough.
Since the arrhythmia that occurs with cardiomyopathy can be detected before the onset of congestive heart failure, it is obvious that checking for this problem is important, particularly in Doberman pinschers and Boxers. Doberman pinschers with atrial fibrillation and dilated cardiomyopathy have a poor prognosis.
Cats might also be treated with aspirin to prevent a saddle thrombus. It is imperative that cats are kept in a relatively stress free environment.
The best long term approach for dogs and cats is not to breed lines that are prone to this problem.
Medical Treatment of Heart Disease
The medical management of animals with CHF (congestive heart failure) is aimed at controlling the deleterious effects of the underlying pathology. These effects typically include pulmonary congestion and edema, cardiac arrhythmias, reduced cardiac output, and excessive vasoconstriction. Many medications are used to treat heart disease. In almost every case they can only control the symptoms, and hopefully, slow down the progression of the disease.
In general, medications used to treat cardiac disease, especially CHF, are highly beneficial. The goal of therapy is to improved the quality of life of these pets while simultaneously minimizing the side effects of the drugs used. Most pets will not go back to being able to exercising vigorously, as a matter of fact, too much exercise can destabilize compensated dogs and cats.
Therapy needs to be tailored made to each pet, and again, constant monitoring is needed to adjust for any changes that are occurring. This means that blood panels, radiographs, ECGs, and blood pressure need to be checked weekly initially, then every 3-6 months, assuming the heart failure is under control.
Cardiac disease is commonly diagnosed in geriatric patients that have other problems simultaneously. Some of the medications used to treat heart disease can exacerbate other medical problems common in geriatric patients. Using these medications properly tends to be a balancing act, minimizing their deleterious affects while maximizing their advantageous properties. This is particularly true if a pet has kidney disease along with heart disease. This balancing act requires constant monitoring.
Many drugs are used in cardiovascular disease. We will go over the more common treatments, especially in regards to congestive heart failure.
ACE (Angiotensin Converting Enzyme) Inhibitors
These drugs are a part of the treatment plan of almost every dog with CHF. The addition of Enalapril® or Benazepril® to conventional therapy in dogs with chronic congestive heart failure resulted in a significant decrease in clinical signs and a 92% increase in survival time. The use of vasodilators, such as Enalapril®, increase the survival time of dogs with CHF. This is especially true in CHF from cardiomyopathy, but does not necessarily apply to dogs with CHF from mitral insufficiency.
They add to the quality of your dogs life by minimizing the fluid buildup in the lungs (pulmonary edema) and abdomen (ascites).
In general, ACE inhibitors lower the blood pressure (decrease afterload) and decrease salt and water retention. They work by inhibiting the conversion of angiotensin I to angiotensin II in the lungs. We discussed this in the Cardiac Anatomy and Physiology section of our heart disease page.
This decreases fluid buildup in the lungs, thorax, and abdomen, and it also makes it easier for a weakened or enlarged heart to pump the blood out into the bloodstream. Kidney values and electrolytes should be monitored while on ACE Inhibitors.
The more common ACE inhibitors we use are Enalapril®, Benazepril®, and Captopril®. Enalapril® is approved for use in the dog by the FDA, and is the most common ACE inhibitor we use. ACE inhibitors can take up to 7 days to produce beneficial effects, and need to be constantly adjusted to maximize their benefits.
ACE inhibitors are commonly used in people that have high blood pressure (hypertension), even if they do not have heart failure.
ARB’s (angiotensin receptor blockers) are also used, and have a mechanism of action similar to ACE inhibitors
Diuretics
Diuretics (lasix, also called furosemide) are the mainstay of treatment for CHF, and should be used in conjunction with ACE inhibitors.
Lasix is a loop diuretic. That means it has its effects on a section of the kidney called the loop of Henle. It is here that lasix causes more sodium (salt) to be excreted from the body. Sodium pulls water with it when it is excreted, so urination increases and fluid level of water in the bloodstream decreases.
This decreases the blood pressure in the capillaries, so less fluid leaks out into the lungs (pulmonary edema) and abdomen (ascites). Another medication, called spironolactone, is also used with lasix, or in place of it.
Overuse of diuretics can cause dehydration and can interfere with normal kidney function. As was already mentioned, lasix use should be monitored with a blood panel every 3-6 months to assess kidney function. As a geriatric pet ages, the kidneys and heart can both have disease, so the use of lasix is a balancing act between these two diseases.
It is rare for a dog or cat to need potassium supplementation (K+) while on a diuretic, unlike people. Your pet will drink more than usual, so make sure fresh water is available at all times.
As a rule of thumb, if a dog or cat in congestive heart failure increases its respiratory rate routinely beyond 30 breaths per minute, we give additional lasix. It is better off to remove the fluid from the lungs and let the red blood cells get oxygen to deliver to the cells, at the expense of the kidneys, than to treat the kidneys with extra fluids to flush waste products out, and have the lungs fill up with more fluid. The more we are able to run diagnostic tests to monitor this, the better we can titrate the diuretics and fluids.
Pimobendan (Vetmedin®)
This FDA approved drug is in a class of drugs called indodilators. This means it increases the strength of the contraction of the heart muscles (ventricles). This is called a positive inotropic effect. It also helps dilate the peripheral blood vessels, decreasing afterload, and making it easier on the heart to push the blood into the arteries. If you review our heart anatomy and physiology page you will learn much more about all of this.
This drugs has been a major help in the treatment of congestive heart failure due to dilated cardiomyopathy or endocardiosis. It increases survival time and quality of life in these patients.
Diet
Minimizing salt in the diet is beneficial in preventing fluid buildup (ascites of pulmonary edema) only when the fluid is present. If you start a restricted sodium diet too soon you can actually cause the opposite effect.
Typical food include Hills K/D and H/D. Many pets eat these foods well, but if they have diminished appetite on these foods then they are of no benefit, since they will continue to lose weight and be lethargic.
Supplements
Supplementation with Omega 3 fatty acids might be of help, along with carnitine and taurine in specific cases of dilated cardiomyopathy. Carnitine will only be effective in a small number of dogs. To know for sure if a dog is carnitine deficient, a biopsy of the heart muscle is needed.
Coenzyme Q10 is also used, although this has not been proven to be effective either.
Exercise Restriction
If your dog or cat has heart failure it needs to stay relatively inactive. The heart is already compromised and working at maximum capacity, and does not have the capacity to increase cardiac output.
Cardiac Emergency
Some pets are presented to us having severe difficulty breathing from pulmonary edema. They can succumb to this problem, so they are a true emergency.
They need to be handled very carefully since they are literally drowning in the own fluids and unable to get air. It would be like a person firmly holding a pillow over your face. These pets need to be left alone initially and given 100% oxygen. Once they are more stable and can be handled we give the medication.
100% Oxygen
Nitroglycerin to dilate the blood vessels and decrease the after load. This is usually only used in an emergency situation.
We use gloves to put the nitroglycerin on the ears since it is absorbed through the skin and can cause a person to pass out
We will also hook up a pulse oximeter to assess the oxygen in the red blood cells
Lasix to reduce pulmonary edema.
We might use low levels of low sodium intravenous fluids to help the kidneys if they are failing also. We cannot thoroughly flush out kidney waste products because this much fluid given intravenously will exacerbate the pulmonary edema that is already present. Once the emergency is under control we might be able to slowly increase these fluids.
The Long Beach Animal Hospital, staffed with emergency vets, is available until the evenings 7 days per week to help if your pet is having any problems, especially shock, seizures, pain, difficulty breathing, or bleeding.
Think of us as your Long Beach Animal Emergency Center to help when you need us for everything from minor problems to major a major emergency. We serve all of Los Angeles and Orange county with our Animal Emergency Center Long Beach, and are easily accessible to most everyone in southern California via Pacific Coast Hwy or the 405 freeway.
If you have an emergency that can be taken care of by us at the Animal Emergency Hospital Long Beach always call us first (562-434-9966) before coming. This way our veterinarians can advise you on what to do at home and so that our staff and doctor can prepare for your arrival. To learn more please read our Emergency Services page.