One of the most insidious diseases we encounter in canines and felines is arthritis. We even see it in birds, reptiles, and pocket pets like rabbits and guinea pigs.
It was not long ago that pets were euthanized because they seemed “old” based on their symptoms of poor appetite, decreased activity, and lethargy. In reality they were not “old”, they had arthritis, and acted like they were old because they were painful.
Today we can treat their arthritis and give them a new lease on life and lead a great quality of life for many more years. All animals get arthritis, we most commonly see it in dogs and cats. This page will emphasize it in dogs since it is most prevalent in them.
Many of our pets are stoic, and can have a disease process brewing on the inside yet show no external symptoms. As the disease progresses eventually the symptoms appear, and we are presented with a very ill pet that seemingly became sick overnight. The reality is that the problem was present for a long period of time. It went unnoticed until your pet went rapidly downhill, when the bodies mechanisms for compensating and coping with the disease have become overwhelmed, and your pet is in a debilitating condition. At this point the disease process is so well entrenched that the prognosis for recovery is poor.
The American Veterinary Medical Association (AVMA) recognizes the importance of early diagnosis and treatment of arthritis..
This concept applies to arthritis in dogs and cats.With our new digital radiography that gives us much more detail, we are diagnosing it earlier. Coupled with substantially improved treatments, we can successfully treat these arthritic and painful animals, and give them a vastly improved quality of life for many more years.
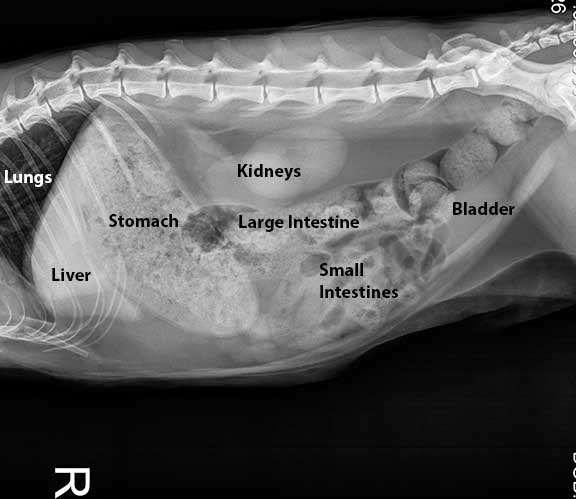
This digital radiograph of the abdomen shows the tremendous detail we get with digital, and how we can see the internal organs in the abdomen. Click on the photo above if you would like to learn how to read a radiograph (you do know the 5 radiographic densities don’t you?).
What’s even better is the fact that some of these new treatments do not involve the use of drugs. We have a multi-system approach to arthritis due to its chronic and debilitating nature, and the fact we strive for treatment modalities that involve minimal use of long term drugs.
Here is a summary of how we approach this important problem. We will talk about these treatments in more detail later in this page:
If your pet is overweight, a common problem in arthritic animals, modifying diet and feeding habits to bring it back to its fighting weight can minimize the symptoms of arthritis. This common sense, inexpensive, and drug free option, seems to escape many people.
Hill’s makes a prescription diet called Metabolic + Mobility that addresses obesity and arthritis at the same time. It is the food of choice for overweight dogs that that are also arthritic.
Arthritis tends to be a disease of the aging. Older pets have different nutritional needs that need to be addressed. These needs cannot be addressed by going to a pet store and listening to the advice of some amateur nutritionist behind the counter trying to sell you the latest gimmick in canine food marketing.
It comes after you discuss your pet’s individual lifestyle needs with your veterinarian, your pet is given a thorough physical exam, and your veterinarian has blood panel and radiographic tests on your pet. Only then will the full picture of your pets needs be understood, leading to a custom treatment protocol specific for your pet.
Chondroprotective agents called neutraceuticals can help in some cases. These are the chondroitin sulfate- glucosamine products available everywhere, including the checkout stand at Trader Joe’s. They are not a panacea, and its important to take a critical look to see if they are working in your pet’s case. Sometimes the placebo effect seems to be transmitted in our minds to our pets, and we do not have an objective standard to determine if these medications truly help. Fortunately they do not seem to hurt, so we can achieve or first goal of “do no harm” as veterinarians.
NSAID’s (non-steroidal anti-inflammatory drugs) are a tremendous advancement in the treatment of arthritis. Non-steroidal means they do not contain cortisone, which was one of the primary drugs used to treat arthritis in the recent past. The NSAID’s are better at treating arthritis when used judiciously to maximize their good effects, while minimizing their potential for side effects. Every pet reacts differently, so if one NSAID does not seem to work, we will try another.
Veterinary Neuronal Adjustment (VNA or VOM) is a tremendous treatment modality that uses the bodies natural healing processes without the use of any drugs. It involves stimulating the autonomic nervous system (specifically the sympathetic branches) and provides substantial pain relief. We have been using VNA at the Long Beach Animal Hospital for over 25 years.
Therapy Laser brings an additional and highly effective treatment modality that again does not involve the use of drugs. This laser penetrates the hair and skin and goes right to the problem area to decrease inflammatory mediators. We recently updated our equipment to include a new therapy laser called MLS that treats using two different wavelengths.
Acupuncture can also be used to augment all of the above therapies. Dr. Seto and Dr. Yamamoto are both certified in acupuncture in animals.
Stem cell therapy is starting to be used, utilizing your dog’s own fat cells. It is still in the early stages, and treatment is not long lasting. If this area of treatment evolves and becomes more practical, we will utilize it.
Exercising your pet in the cooler part of the day, without excess trauma like jumping for long periods of time, will keep your pet flexible, the joins warm and lubricated, and keep its weight under control. If your pet is not afraid of water, letting it swim in a shallow area is a great way to enhance mobility.
A relatively new drug from Zoeitis, called Librela (bedinvetmab), is a once-monthly injection of a monoclonal antibody to treat arthritic pain. It targets nerve growth factor (NGF), a key cause of pain in arthritic animals. One of our doctors will let you know if it applies to your pet when we diagnose arthritis.
Please be realistic about the fantastic claims that abound on the Internet for cheap treatments that will help your pets arthritis. These treatments have show to be nothing more than effective marketing. This disease is complicated and serious, and needs more than some supplement you purchase online.
What is Arthritis?
Dogs are prone to many different types of bone problems. This page will focus on the arthritis that tends to occur in canines, especially as they age. Arthritis literally means inflammation of the joint, but the term is used more generally to describe several different processes. These include degenerative joint disease (DJD), infectious joint disease, immune mediated joint disease, and crystal-induced joint diseases.
Many people use the term arthritis synonymous with osteoarthritis (OA), a complex, slowly progressive, and degenerative arthritis that is characterized by the gradual development of joint pain, stiffness, and a decreased range of motion.This is the type of arthritis common in older pets, and is increasing as pets live longer.
Anatomy
A normal joint is lined with hyaline cartilage, which is the covering over the end of the bone. It provides an almost frictionless surface for the bones to articulate, and also acts as a shock absorber. Hyaline cartilage is comprised of chondrocytes, proteoglycans, and collagen.
A normal joint is encased in a fibrous structure called the joint capsule. The joint capsule helps stabilize the joint and keeps the cartilage bathed in synovial fluid. Ligaments, which attach bone to bone, also provide joint stability.
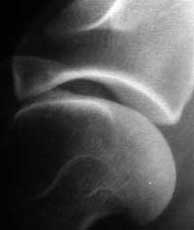
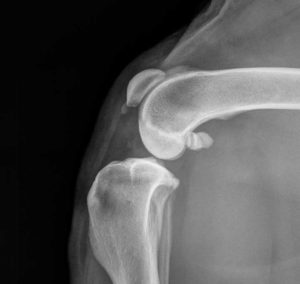
This picture is from an actual surgery on the knee of a dog with a ruptured cranial cruciate ligament. The head is on the right, the foot is on the left, so the joint appears horizontal.
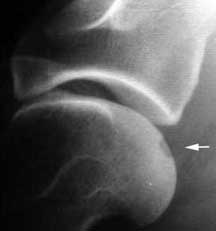
This picture from surgery during repair of a ruptured cranial cruciate ligament shows a ridge of bone running horizontally at the bottom (arrow). This is what arthritis looks like in the joint. The normal smooth cartilage above it is the normal groove of the knee (stifle) joint. The patella runs along this groove.
Cause
The cause of this complex and multi factorial disease can be primary or secondary. Primary OA results from normal stresses acting on abnormal cartilage. Secondary OA is more common, and results from abnormal stresses acting on normal cartilage, such as an unstable joint caused by canine hip dysplasia, fragmented coronoid process, ununited anconeal process, patellar luxation, or a ruptured cruciate ligament. Some of the factors that can cause OA include excessive exercise, obesity, poor nutrition, trauma, immune reactions, and genetic predispositions.
The following radiograph on the top is from a normal shoulder joint. The one on the bottom has an abnormal flap of cartilage at the arrow. This is know as osteochondritis dissecans, and is a primary OA. Without this radiograph we never would have know this limping pet had this problem.
This normal shoulder joint shows no problems
The white arrow points to a flap of cartilage that has eroded off
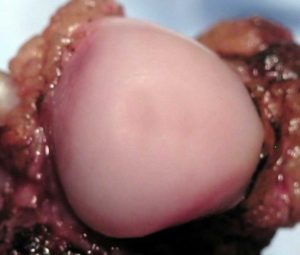
To help you understand what you are looking at in the above two radiographs, this is what a normal shoulder joint looks like during a necropsy. Notice how smooth it is.
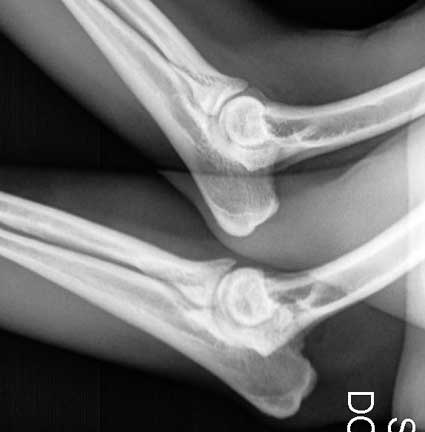
These two elbows from the same dog are normal
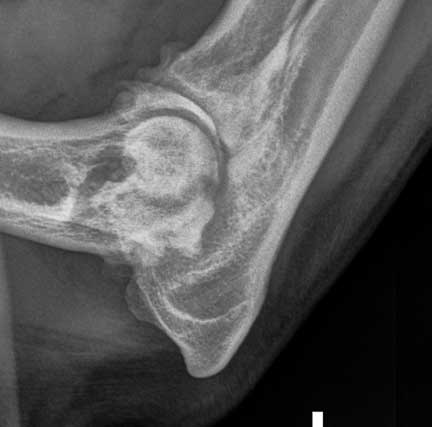
This elbow from a different dog shows advanced arthritis, as evidenced by the moth-eaten appearance. It is probably secondary to elbow dysplasia
Damage to cartilage might occur as one event, or be the culmination of many small events over years. As swelling occurs, and the joint capsule becomes stretched, pain occurs. Your pet will use the joint less because of this pain, leading to muscle atrophy and the inability of the surrounding tendons and muscles to support the joint. As the muscular support of the joint weakens the joint capsule, ligaments, and cartilage become further stressed and stretched, leading to even further pain.
At this point the body releases chemicals called inflammatory mediators, (the therapy laser works on these mediators) which further damage the cartilage and add to even more swelling. It is obvious that this rapidly becomes a vicious cycle leading to debilitating pain. When OA progresses to the point that you notice your pet in discomfort or pain, the damage to the joint might be irreversible.
Diagnosis
Signalment
OA is commonly diagnosed in older dogs and cats. Some breeds are prone to getting it because of the conformation of their joints.
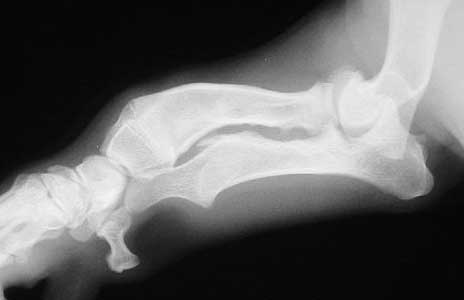
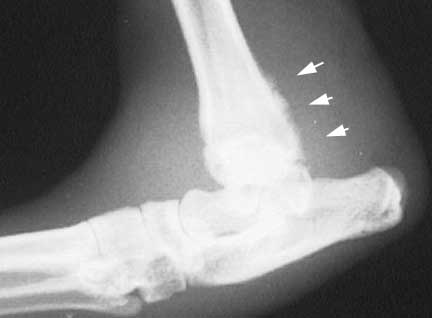
Dogs like Dachshunds have abnormally shaped long bones that might predispose them to OA. This is the wrist, forearm, and elbow of a Doxie. The medical terms are carpal, radius, ulna, and olecranon.
History
It is important to understand the initial symptoms might be subtle. Your pet will be experiencing pain or discomfort, yet it might not show any external signs. Dogs, especially large breeds, can be stoic, and show no outwards signs of pain even though they are painful on the inside. Close observation of your dog’s daily habits as it ages will help you to see the subtle signs of pain.
Symptoms are related to joint pain and stiffness. Most owners notice a pet losing its ability to perform normally, such as a reluctance to jump or climb stairs, or even limping. Stiffness after rest that diminishes rapidly as your pet starts moving and warms up is a hallmark sign of OA. Other symptoms of arthritis include lethargy and poor appetite, which are the result of pain.
Initial symptoms are subtle and easily missed. Most dogs show a reluctance to run or move about. Some might not walk as long as usual, stop part way through a walk, or come back from a routine walk and go right to their bed to rest. They might be slow getting up.
Some will be reluctant to go up or down stairs, or might even be limping. As the disease progresses these dogs might be in overt pain and lose their appetite. Some of these symptoms occur in other diseases, notably hip dysplasia and intervertebral disk disease. The are treated in similar ways in some cases, in different ways in other cases, so a proper diagnosis is imperative.
Dogs that will not go on extended walks, or dogs that pant excessively during a walk could also indicate OA. Symptoms can be worsened by obesity, too much exercise, and by cold or damp conditions.
Physical Exam
In some pets there are no abnormalities detected during a physical exam. Pain or discomfort might be found by palpating a joint or pushing on the mid or lower back. We might feel grinding of joints (crepitus), a swollen joint, abnormal bone formation and roughened bones, or inflammation at the joint. Dogs with longer standing OA might show atrophy of muscles. Range of motion might be limited and cause discomfort or pain. There might also be subtle signs during the neurologic part of the exam.
Some pets are so distracted during an exam (this happens to us people commonly) that they do not exhibit signs of pain when touched in painful places. This is why we need some basic diagnostic tests.
Diagnostic Tests
Radiography is an important diagnostic test to perform on a dog suspected of having OA. Even though a radiograph can be normal in a pet that has OA, it is a substantial help in verifying the diagnosis and determining the degree of involvement.
There are many diseases that can mimic the symptoms of OA, so a radiograph should be taken on every suspected OA to eliminate these other causes.
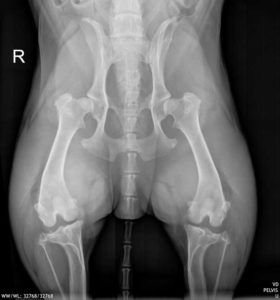
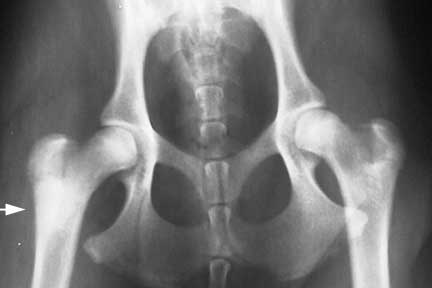
This is a VD (venture-dorsal) view of a dog’s pelvis. This dog has hip Dysplasia. Do you see it? Follow this link to our Hip Dysplasia page to learn more.
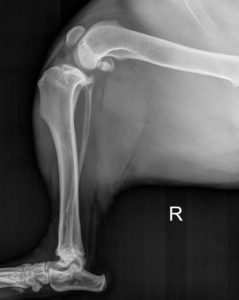
This is an Xray of the femur, knee joint (stifle), tibia (shinbone), and tarsus (ankle). It is a lateral view of the same dog as above.
This is a lateral view showing a close up of a normal knee without arthritis
This knee has arthritis. The arrows point to all of the rough edges that are indicative of OA. Also, the bone has a stronger whitish appearance, another indication of OA. The subtle changes on the radiograph don’t seem like much, but to a joint this is abnormal and painful.
This dog was originally suspected of having arthritis based on a history of soreness in the hip area. It would be a mistake to treat this dog with an arthritis supplement and let the undiagnosed problem progress.
Radiographs revealed the true diagnosis was not the assumed arthritis in this case. The white circular area in the bone has the potential to be several different diseases, some of them serious like bone cancer. A bone biopsy is need to know for sure.
A close-up view gives you a better idea of this dog’s problem
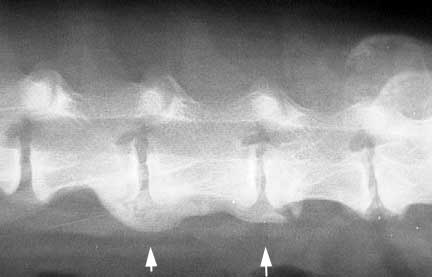
This form of OA is called spondylosis, which is arthritis of the vertebrae in the spine.
It is very common as pets age and causes substantial discomfort, nerve weakness, and even urinary and bowel incontinence.
This 12 year old Chihuahua has severe spondylosis throughout its lumbar vertebrae
The red circles show the severe spondylosis this bulldog has. The lumbo-sacral (called L-S) spondylosis on the right is very painful. It is affecting the nerves to the bladder, causing an inability to properly urinate. The hugely distended urinary bladder is the result of this nerve problem, and can be seen as the large whitish area in the center of the radiography. A bladder this large is painful and prone to a chronic infection (UTI or cystitis).
You can learn more about the bones of the spine by going to our intervertebral disk page.
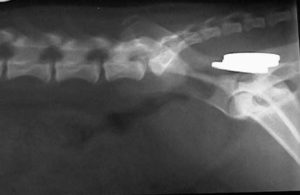
This next dog was sore around its rear quarters when petted by the owner. The owners of the dog assumed it was arthritis and treated the problem on their own. When it did not improve the dog was brought to us for a proper diagnosis. Look at the lateral radiograph below of its posterior abdomen and see what you think the cause of the soreness was.
Did you figure out what is going on? Those circular white objects towards the top right of the radiograph are 3 pennies in the rectum! Even though it seems like a safe place to store money, it was painful and causing this dog’s problem.
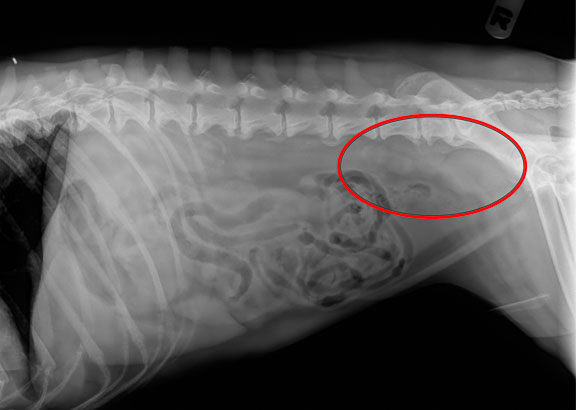
This is another dog that was sore in its rear quarters which that owner (and all of his well intentioned friends that love to give advice) assumed was just old dog arthritis. The circle shows the real cause of the problem in this dog’s back end. It is due to enlarged sublumbar lymph nodes from malignant cancer.
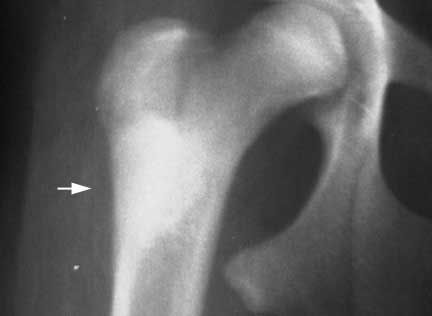
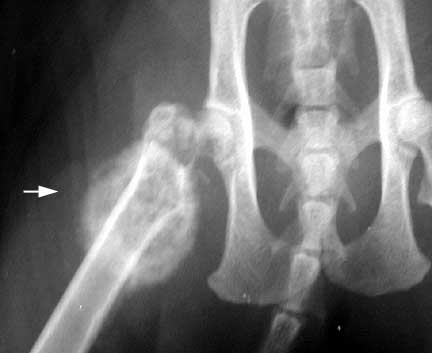
A very important differential when diagnosing OA on a radiograph is a bone tumor. This one is on the femur (thigh bone). This dog had symptoms of muscle atrophy and limping on this leg. If a radiograph had not been taken these symptoms could have easily been mistaken for arthritis. At this stage of the disease amputation is usually the only way to temporarily stop the tumor from spreading.
This is a serious form of cancer, and usually requires amputation
The other important differential on radiograph like this is a bone infection called osteomyelitis. The fuzzy or roughened edges at the arrows is the infection.
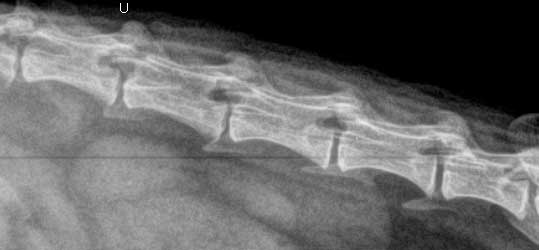
The incorporation of digital radiography into our practice gives us substantially more detail on a radiograph. This is easily seen in the Ferret spine radiograph. Ferrets are prone to many disease, click here to learn more.
Treatment
Treatment of OA initially includes correction of any underlying primary diseases such as surgical correction of a torn ligament or arthroscopy to remove a cartilage flap. Once any primary disease has been addressed, the goal of treatment is to slow the progression of OA and to keep your pet comfortable. It’s important to realize that there is no cure for OA. The following are the treatment options we find that are most successful, and were mentioned at the beginning of this page.
As you will see from the following treatments, we use a wide variety of treatment options, and customize them for your pet’s specific situation. We always use a balanced approach, utilizing drugs only if needed, and at the lowest dose possible.
Nutrition
Most pets with OA will require some adjustment in their lifestyle. Weight management is most important, since obese pets put unnecessary strain on joints, leading to a more rapid progression of the disease. Depending on the degree of obesity your veterinarian might put your overweight pet on Hill’s Metabolic Diet or Metabolic + Mobility. This is a weight control product with lasting effects and is our first recommendation. We might also use Hill’s W/D (weight diet) or Hill’s R/D (reducing diet).
If your pet is not overweight we will utilize a food called Hill’s J/D (joint diet). It has added chondroitin sulfate and glucosamine in addition to essential fatty acids and carnitine. These foods are complete and balanced nutrition and can be fed for the rest of your pets life. There is a version for dogs and one for cats.
Like all Hill’s foods it highly recommend in almost every case of arthritis unless your pet has some other disease that precludes their use. All Hill’s Prescriptions Diets our doctors recommend are unconditionally guaranteed. We have a detailed page on Nutrition Advice to help clear the air on all the hype that exists on the Internet to get you to put your money into this multi billion dollar a year business.
Exercise
Excessive exercise that leads to pain or discomfort should be avoided, but moderate exercise is recommended. Swimming is an excellent exercise for pets that have OA and aren’t fearful of water. Most pets do best with several short, exercise periods per day rather than fewer extended periods. Each patient will have their own unique program of weight management and exercise, and we can help you individualize one for you and your pet.
There are even veterinarians that specialize in rehabilitative therapy, with specialized swimming pools and therapy methods.
Chondroprotective Agents
These products typically contain precursors of cartilage and joint fluid synthesis. We like to use these medications first since there are negligible side effects and they might be an aid in preventing further deterioration of the cartilage. Hill’s J/D contains adequate amounts of these ingredients. Please remember that if a little is good, a lot is not necessarily better, because you disrupt the nutrient balance that is so important in nutrition.
These products have a positive effect on cartilage matrix synthesis and an inhibitory effect on the enzymes that break cartilage down. They might require up to 6 weeks of use before OA symptoms are diminished. Unfortunately they do not work in every case, so be realistic and make a careful assessment as to their efficacy.
Adequan
Adequan (polysulfated glycosaminoglycan) is an injectable chondroprotective agent. Adequan incorporates into joint cartilage and inhibits several enzymes that break down cartilage. No studies have been done in animals other than horses and dogs, but it appears to be safe and effective in other species including cats, rabbits, ferrets, and birds.
The intramuscular injections are initially given twice weekly (every 3-4 days) for a month, then given monthly as needed. Adequan seems to be most effective when given in the early stages of OA.
Dasuquin
Unlike the injectable adequan, Dasuquin and other oral joint supplements are considered nutraceuticals, or nutritional supplements, and do not require FDA approval. Cosequin contains glucosamine and chondroitin sulfate, agents proven to be effective at supporting and protecting joint cartilage.
In addition, Dasuquin contains ASU (avocado/soybean unsaponifiables) that makes the glucosamine and chondroitin sulfate more effective.
NSAID’S
The non-steroidal anti-inflammatories (NSAID’S) are the most commonly used drugs in treating OA in dogs. NSAID’s are highly effective and tend to be the drug of choice when we put your pet on actual arthritis medication. They are so effective we even use them for routine post operative pain control in dogs and cats. They have saved many a dog from long term pain, and even euthanasia.
There are many different versions, with the original one being Rimadyl (carpofren). After using many different NSAID’s over the decades we still use it. There is another NSAID called Galliprant that we have been using more and more, and it is becoming our medication of choice to treat arthritis.
NSAID’S work by inhibiting an enzyme in the inflammatory pathway, thereby providing analgesia (pain relief), antipyrexia (decreased fever) and reduced tissue swelling. The enzyme that is inhibited is cyclooxygenase (abbreviated COX). This enzyme causes an inflammatory reaction in the joint fluid that surrounds the joint. Galliprant works by blocking the prostaglandins that cause inflammation.
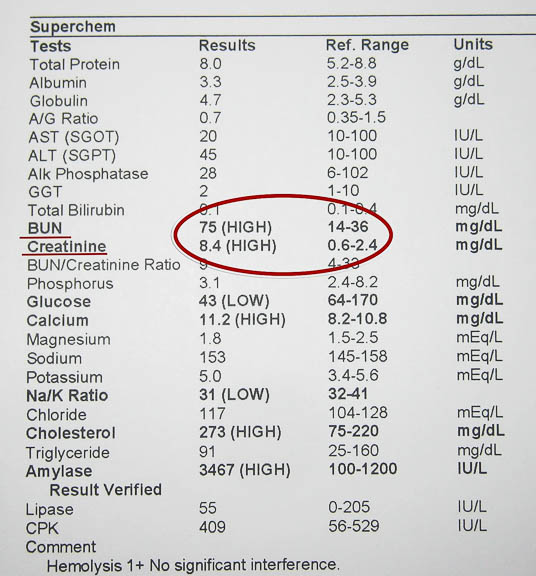
Before we start your pet on NSAID’S we perform an examination and run a baseline blood sample. Every 6 months we will examine your pet and recheck the blood to look for any potential side effects. This will make sure kidney and liver function is adequate.
This pet has kidney disease, and the problem needs to be addressed before we institute NSAID therapy. We would use a lower dose of the NSAID many times in a pet with kidney disease like this to make sure the NSAID is not making the kidney disease worse.
Using NSAID’S alone is not recommended since the signs of arthritis are masked, leading to a more active dog and a quicker progression of arthritis. NSAID’S, in combination with weight loss and chondroprotective agents, provide cartilage building blocks in addition to pain relief, and may slow the progression of OA.
All NSAID’S carry a small risk of side effects, so careful observation of your pet while on one of these medications is important. If they occur, the most common side effects are vomiting and diarrhea. There might also be kidney and liver problems, and even bleeding. These side effects can be minimized by using the lowest dosage and frequency possible, giving the medication on a full stomach, and giving Pepcid AC prior.
The best way to minimize the potential for side effects, yet still get the most out of NSAID’s, is to use the lowest effective dose of the NSAID of choice, and combine it with proper diet, VNA and Companion Laser as additional treatments. You will learn more about these treatments below.
VNA (also called VOM in the past)
An additional treatment modality that has yielded great success for well over the last 20 years is called VNA. It has been a game changer for us in the treatment of arthritis in a wide variety of animals.
It is a non-invasive and non-painful way to stimulate the autonomic nervous system to help correct the problem. Through the use of VNA we can decrease the use of the above medications in almost all cases. By decreasing the use of these medications, we help your pet live a longer and healthier life, while decreasing you medication costs over the life of your pet. Click here to learn more about VNA.
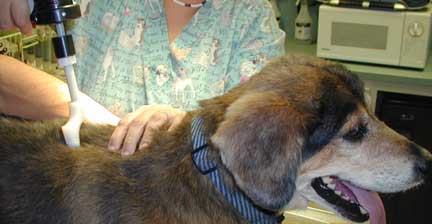
This dog is getting VNA therapy for its arthritic spine
We use VNA in a wide variety of species. This rabbit has GI stasis, and felt much better after this treatment.
Companion Laser Therapy
In the last few years we have added a new and natural way to treat arthritis using the Therapy Laser. This modality has been used to treat people for over 30 years and has recently been approved by the FDA for use in animals. This treatment modality has been a huge boon to our geriatric pets with painful arthritis, especially when used with low dose NSAID’s and VNA. To learn more about it please click here.
Acupuncture
This can also be used at any time to augment the treatment already being utilized. To learn more about how we use acupuncture follow this link.
Do you see the two acupuncture needles on this pet’s neck?
Miscellaneous Medications
Gabapentin
This seizure medication is another useful adjunct as the arthritis progresses.
Brupenorphine
Short term use can be effective for pain control.
Regenerative Medicine
What this is not doing is to generate new and healthly cartilage, as is a common misconception. What this treatment does is take a high concentration of growth factors and anti-inflammatories and bring them to an area of relatively poor tissue healing with the chance there will be a reduction on the inflammatory process.
Stem Cell Therapy- (Adipose Derived Stem Cells ( Ad-SCT ))
This promising yet unproven treatment utilizes stem cells from your own dog’s fat cells to alleviate arthritis symptoms. This means there is no chance of rejection, a major advantage of this technique.
Your dog has to be anesthetized for a short time in order to harvest the fat cells. Collection sites can be in many areas depending on your dogs conformation and fat reserves. Once the fat cells are harvested they are shipped overnight to the company that isolates the stem cells with a specialized technique. They are returned usually within 48 hours. We sedate your pet again and inject the stem cells into the affected area.
We will keep you posted as this promising therapy is given better scrutiny to make sure it has no deleterious effects in the long run and actually helps.
Platelet Rich Plasma (PRP)
This is a blood sample from your pet with a high concentration of platelets without red blood cells (RBC’s) and some white blood cells (WBC’S). These platelets have growth factors and anti-inflammatory properties.
Rehabilitation
This can range from using wobble boards and exercise balls up to underwater treadmills. These can be beneficial, and we would send you to a veterinary specialist to help determine if this will help in your pet’s case.
Return to Canine Diseases Page