IBD is an inflammatory condition of the stomach, small intestines, or large intestines (the gastrointestinal (GI) tract). It is sometimes called Idiopathic IDB. The Idiopathic part means that the cause of the condition is unknown.
IBD tends to be chronic in nature. It is one of the most common conditions of the gastrointestinal tract diagnosed in pets, especially in cats.
Despite its prevalence, it is one of the least understood conditions, especially regarding cause. Some pets respond well to treatment, others do not.
Some cases of IBD involve the liver and pancreas. In this case there are 3 diseases occurring, and we refer to it as Triaditis. This is more difficult to treat than IBD alone.
The usual symptoms of IBD are poor appetite, vomiting, diarrhea, and weight loss. Cats tend more towards vomiting, dogs tend towards diarrhea. These symptoms appear in many other diseases, so you cannot assume your pet has IBD from symptoms alone.
To learn the process of how we make a diagnosis of a disease when the symptoms are the same as many other diseases, we have a methodical and detailed approach. It is called the Diagnostic Process.
We discuss the importance of worms (internal parasites) many times in this page in regards to IBD. With the modern medications we have, including flea products that contain medication to kill worms, it behooves you to treat your pets for worms monthly.
Not only might it help prevent IBD from appearing at some time in your pet’s life, it will protect you and your children. Our Internal Parasites page has the scoop on all of this.
In spite of its prevalence, many pets are diagnosed with Idiopathic IBD when they do not have it. To standardize what IBD is, the World Small Animal Veterinary Association has listed the following criteria to help make this diagnosis:
The GI (GastroIntestinal) symptoms must be present for at least three weeks
Diet change, worming, and medication do not give a significant reduction in symptoms
No other explanations can be found for the symptoms
Biopsies of the intestines show significant inflammation of the interior lining
The resolution of symptoms when put on mediations that modulate the immune system (immunosuppressive).
This criteria means that a pet that responds to just a diet change technically has a Food Responsive Enteropathy. If a pet responds just to antibiotics then it technically has an Antibiotic Responsive Enteropathy.
Graphic photos of surgeries are on this page
Anatomy and Physiology of the Gastrointestinal (GI) Tract
When your pet eats, food from the stomach passes into the small intestine, which is composed of three different sections called the duodenum, jejunum, and ileum. The majority of nutrient (proteins, carbohydrates, fats) digestion occurs within the small intestines.
The inner lining of the intestines is called the mucosa, and that’s where all the action occurs when it comes to absorbing nutrients. The mucosa has a large surface area because there are microscopic folds called villa.
This is the lining of the small intestines. The villa are microscopic, so you cannot see them without a microscope.
There are many different types of specialized cells in the lining of the mucosa. Some of these cells specialize in aiding digestion, some are for absorption of these nutrients into the bloodstream, and some are part of the immunes system and defend the body from foreign invaders.
These immune system cells are important for protection due to the constant exposure the GI tract has to outside invaders in the form of oral ingestion of food and its many contaminants. It is these cells that can overreact and cause IBD symptoms.
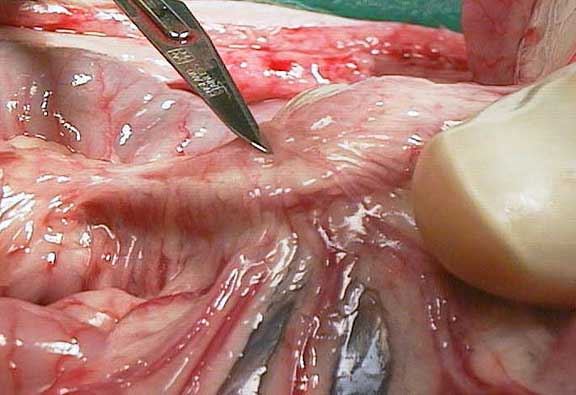
These are the small intestines during a routine abdominal surgery. Notice the extensive blood supply, necessary to get those nutrients from the lining of the intestines into the bloodstream, and then off to every cell in the body- amazing!
This is what the ingesta looks like as it passes through the small intestines
The pancreas secretes digestive enzymes into the small intestines as the food passes through the duodenum. These enzymes are crucial for digestion of fats, carbohydrates, and proteins. As the food continues down the small intestines the enzymes from the pancreas continue their breakdown of nutrients, which are then absorbed by the mucosa of the jejunum and ileum and make it into the bloodstream.
This is the pancreas, a small but mighty organ. Our surgeon is holding the duodenum (D), with the pancreas in the center (P).
Close up view of the architecture on the outside of the pancreas
The gall bladder secretes bile into the duodenum to help in digesting fats. When the liver is a part of IBD the bile can build up in the liver and cause a problem. This is a part of the Triaditis that complicates IBD.
The large intestine is composed of the cecum (our appendix), colon, rectum, and anus. Water, electrolytes (sodium and potassium), sugars, and vitamins are the main nutrients absorbed by the large intestine. Some vitamins are produced in the large intestine also.
Nutrients that were not broken down or absorbed well enough within the small intestine are further digested in the large intestine due to microbial fermentation. The large numbers of these good bacteria that are present in the intestines are crucial to normal health.
The human cecum (appendix) has atrophied to the point that it is no longer needed. Our diet does not have the fiber of our ancestors, so this organ is not needed for normal digestion, which is why it can be removed if appendicitis occurs.
As a fun anatomical comparison, the cecum of a rabbit is enormous in relation to the rest of its body. That is because it is a hind-gut fermenter, and contains large numbers of bacteria to help digest food that is high in fiber.
Part of the cecum of a rabbit on a radiograph
Our rabbit GI stasis page has radiographs of the cecum along with actual pictures to give you an idea of just how large it is.
Pathophysiology
Allergens cause inflammation of the mucosa, leading to the symptoms associated with IBD. The allergens that cause this inflammation can be anything, with food (especially protein) as the main culprit. Bacteria and parasites are also allergens that cause inflammation of the mucosa.
It is the immune system that over reacts to these antigens that causes the symptoms of IBD. This immune system over reaction is why pets that truly have IBD need medication to suppress the immune system, in addition to dietary changes and antibiotics.
The size of the lumen thorough with the food passes and intestinal wall thickness of a normal small intestine
You can easily see the smaller lumen and thickened intestinal wall in this pet with IBD
Inflammation of the pancreas is known as pancreatitis. In pancreatitis, the digestive enzymes that would normally be secreted into the duodenum to digest food are now leaking out of the pancreas into the abdomen, causing tremendous inflammation and pain to surrounding organs.
Pancreatitis is a serious disease, and usually requires hospitalization, intravenous fluids, and medication. It can be hard to diagnose in cats because they usually become quiet and sit as if content, when in reality they are in pain. A clue is the fact that are not eating well.
Inflammation of the liver in some cases may be associated with IBD, permitting an infection to creep up the bile duct and into the liver. There are many different sources to this infection, ascending from the GI tract or urinary tract.
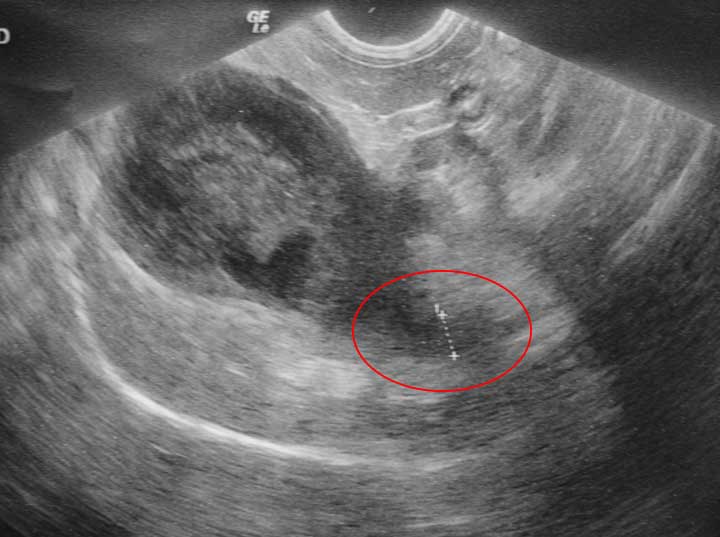
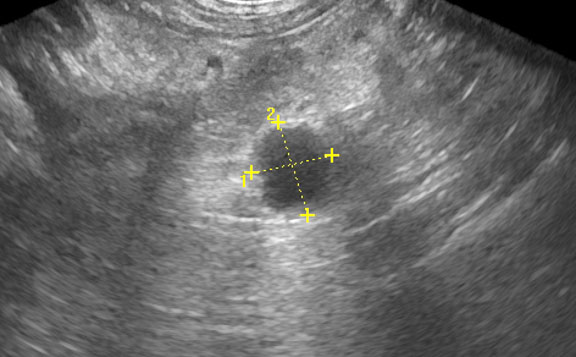
This is the common bile duct being measured during an ultrasound
The pancreas, liver, and intestines are closely associated, and when one has a problem it causes inflammation in one of the other ones. When all three have a problem it is called Triaditis. As you can see, it all gets quite complicated.
Cause
IBD is one of those conditions where the exact cause might never be identified. The most common causes are dietary allergies, infections, and environmental stress. Stress can happen in multiple pet households, during holidays, and in extreme weather. Please read our page on how to reduce stress in cats.
Dietary allergies are involved with sensitivity to protein in the diet. Sometimes, an inability to absorb nutrients, called a malabsorption syndrome, is involved. Some pets generate an excessive amount of a specific white blood cell called an eosinophil (eosinophil gastroenteritis) in the lining of the GI tract.
Other dietary causes might include artificial coloring, preservatives, and food additives. Differentiation between the above-mentioned causes is difficult, especially since many IBD cases are associated with several concurrent factors.
It is suspected that puppies with a large amount of internal parasites (worms) are setting the stage for IBD later in life. This is another good reason to have your pet checked for internal parasites at least yearly, and wormed frequently when young.
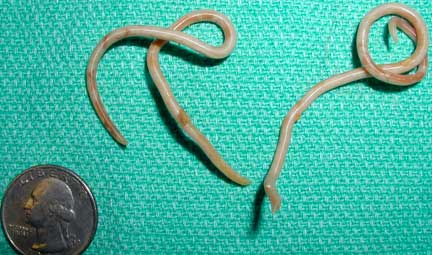
These are what roundworms (ascarids) look like when expelled
Pancreatitis is highly associated with pets that are overweight, particularly spayed female dogs. Fatty meals are important components of the clinical history for cases involving pancreatitis. As a result, we tend to see this cause of pancreatitis around the holidays when people are celebrating with turkey (and gravy) and other similar foods that their pets’ eat also.
Inflammation of the pancreas can spread to the liver due to its proximity. This can inflame the gall bladder, causing bile to backup into the liver. This can lead to Triaditis mentioned earlier. You can learn about this from our Gallbladder Removal page.
Inflammation of the liver and biliary system, known as cholangiohepatitis, is most commonly associated with a bacterial infection. In cases of Triaditis, it is unknown as to whether the liver is the first organ affected, resulting in secondary inflammation of the pancreas and gastrointestinal tract, or if it is the other way around.
It has been hypothesized that bacterial infections may be the initiating cause of cholangiohepatitis, with IBD and pancreatitis following thereafter.
Proteins and grains in the food contribute to dietary intolerance. Intolerance occurs when there is an abrupt change in the diet, resulting in an inability for the gastrointestinal tract mucosa and associated cells to adapt accordingly. When this happens foods are often not digested or absorbed properly.
Maldigestion is a separate condition of the gastrointestinal tract that generally occurs secondary to exocrine pancreatic insufficiency. The endocrine pancreas secretes insulin to regulate the blood glucose level. The exocrine pancreas secretes the digestive enzymes needed to digest food in the intestines.
If the pancreas is not secreting enzymes into the small intestines as the food passes, the nutrients will not be broken down and absorbed into the bloodstream. This leads to weight loss and diarrhea, even in a pet that is eating.
Malabsorption is secondary to numerous disease processes such as food allergies and/or intolerance, protein losing diseases of the gastrointestinal mucosal layer, intestinal parasites, antibiotic responsive disease, cancer, IBD, and immune-mediated disease.
In this situation the exocrine pancreas is secreting the proper digestive enzymes. It is an inflammation of the inner lining of the intestines (the mucosa) that prevents absorption of the nutrients into the bloodstream.
There are numerous intestinal parasites known to cause the same symptoms as IBD. They include roundworms, hookworms, whipworms (dogs only), cryptosporidia (protozoa), toxoplasma (protozoa; cats only), coccidia, and giardia.
Some intestinal parasites are known to affect humans as well (zoonotic potential). These include the larvae of roundworms causing organ involvement (visceral larval migrans), or eye involvement (ocular larval migrans), hookworms (skin involvement), giardia (gastrointestinal disorders), coccidia (gastrointestinal disorders especially in immune suppressed individuals), toxoplasma (congenital defects in babies), and cryptosporidia (gastrointestinal disorders).
A fecal examination is often one of the first steps when diagnostics are being evaluated in a pet with a gastrointestinal disease. Our intestinal parasites page has detailed information on these parasites (worms). We sometimes do a fecal Giardia test since this parasite can be hard to detect.
Cancer can also be a cause. In cats, lymphosarcoma is the most common type of cancer known to affect the gastrointestinal tract. This is not easy to diagnose, since the changes present in IBD are very similar to those in Lymphosarcoma when the pathologist analyzes them under the microscope.
Depending on the type of lymphoma (small, medium or large cell lymphoma), tissue samples must be sent in for further diagnostics in order to definitively differentiate between early cancer and IBD. Proper treatment depends upon a proper diagnosis.
These severely thickened intestines are from cancer
We have a page that shows an exploratory surgery on a cat with intestinal cancer.
Although there are no definitive infectious agents that consistently result in IBD, some bacterial organisms such as Giardia, Salmonella, Clostridium, and Campylobacter could be a cause. Some of the “good” bacteria, those that are necessary for life, can become imbalanced and cause the symptoms seen in IBD.
Any medication can disrupt the lining of the intestines. The most common one is antibiotics, since they disrupt the normal GI bacteria (referred to sometimes as flora).
Toxicities (plants, chemicals), hyperthyroidism, FIP, FeLV, FIV can all be a part of the cause of IBD.
Diagnosis
Signalment
Both dogs and cats are commonly affected by IBD, although it is much more of a problem in cats. IBD can occur at most any age due to the numerous causes of the condition; however, it is usually observed in pets over the age of two .
Triaditis is more commonly diagnosed in middle to older aged cats. If it is associated with a food allergy, they tend to be young adults to middle aged. Males and females get IBD in equal frequencies.
Addison’s disease, which is common in Standard Poodles, can cause symptoms similar to IBD.
History
Sometimes pets are affected by IBD for many years while appearing apparently healthy in all other aspects. Typical symptoms are lethargy, poor appetite (anorexia), weight loss, diarrhea and vomiting.
Depending on the inciting cause, the clinical signs may occur intermittently over a long period of time (i.e. dietary allergy) or abruptly and progressively (immune-mediated, infectious, dietary allergy, cancer).
If Triaditis is present clinical signs may range from lethargy and decreased appetite to severe vomiting, diarrhea, abdominal pain, and icterus (jaundice) due to liver compromise).
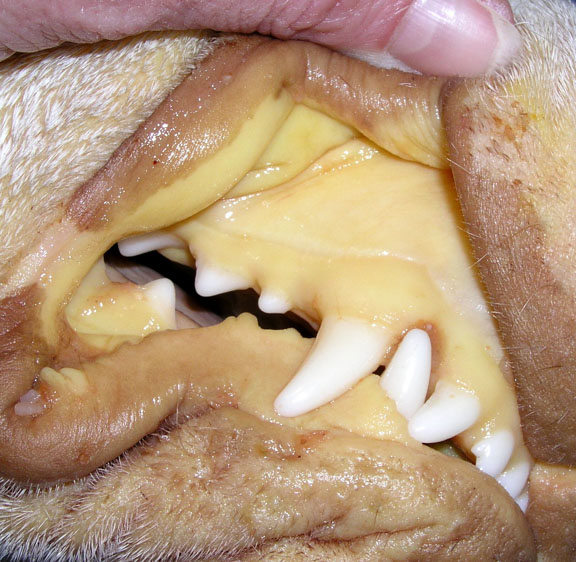
This pet has severe icterus (also known as jaundice)
Cats can have variable symptoms compared to dog. Cats that have pancreatitis might sit quietly and appear to have no problems. In reality, these cats are painful, which is why they sit like this.
Physical Exam
In both dogs and cats, palpation of the abdomen might reveal painful and thickened bowel loops. This is not a consistent sign, and just because bowel loops are thickened, does not mean there is a problem. Pain may also be associated with palpation of the pancreas or liver in cases of Triaditis.
Lymph nodes deep within the abdomen may be enlarged and palpable as well as painful. Excessive intestinal sounds (called borborygmus ) might be heard on auscultation of the abdomen.
In more chronic cases, other subtle signs may be present such as a dull hair coat, mild to moderate dehydration, fever, and overall poor body condition. None of these are consistent findings, and cannot be relied upon for a diagnosis of IBD.
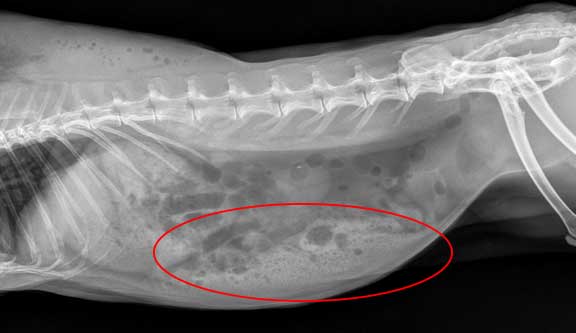
These lymph nodes, call the sub lumbar, are enlarged on this dog. They are the whitish circles within the red circle. They are due to cancer, but they cannot be palpated.
Diagnostic Tests
Complete blood count, biochemistry panel, and urinalysis, are a starting point for diagnosis. Certain blood values might suggest IBD if in combination with clinical signs.
Even “normal values” are clinically diagnostic, as they help to rule out another disease that can cause the same symptoms as IBD. A pet with a perfectly normal blood panel can still have IBD.
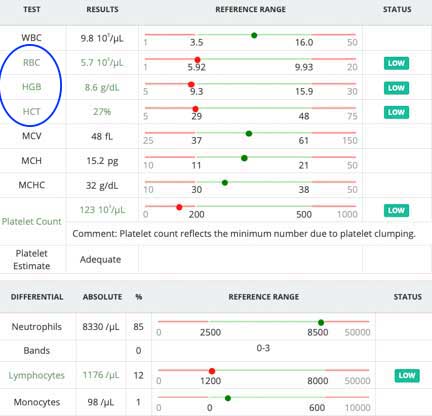
Some pets will have a chronic anemia (low red blood cells). Sometimes the white blood cells will be elevated, in other cases the protein will be low (hypoproteinemia).
Anemia is diagnosed on a blood panel
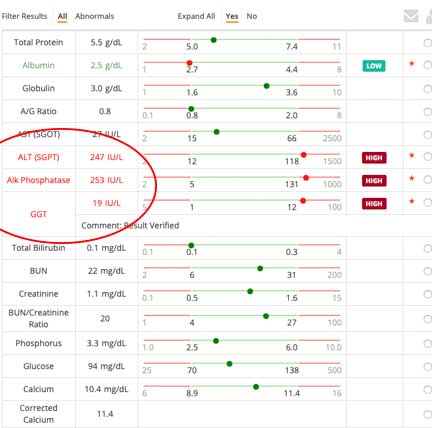
Cholangiohepatitis (inflammation of the liver) in cats, when Triaditis is present, may be further suspected if bilirubin (hyprebilirubinemia) or liver enzymes are increased.
All three of these liver enzymes are elevated, a possible indication of Triaditis
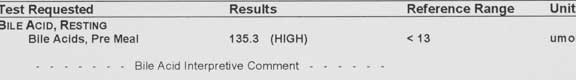
A bile acids test helps assess the liver in these cases. There might also be a low cobalamin level.
This bile acids test in a cat with a liver shunt is very high
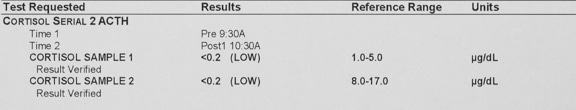
A resting cortisol or ACTH stimulation test might also be used to eliminate Addison’s (hypoadrenocortocism) disease
This low cortisol on an ACTH stimulation test is classic for Addison’s disease in a dog
Fecal examination is an important and inexpensive test to rule out internal parasites (worms). We sometimes give worm medication (called anthelmintics) to pets with a negative fecal if they have and GI symptoms.
This is because a pet can have internal parasites that do not show up on a fecal exam. Our intestinal parasites page has much more information explaining this.
A fecal exam, checking for internal parasites (worms) is important in every pet with any signs of illness. In this exam, we are checking for eggs (ova) of the parasite. A special test for Giardia is also used.
Bacterial cultures are also utilized in some cases. The bacteria we are checking for include:
Campylobacter
Salmonella
Cryptosporidium
This is what we want to see when we do a urine culture- no bacterial growth in 48 hours
Abdominal radiographs are often normal in cases of IBD, but are a necessary tool to rule out other causes of similar clinical signs. Survey abdominal radiographs are also indicated prior to ultrasound as well.
This dog had chronic diarrhea. Nobody took a radiograph prior to treatment. The cause was not IBD, it was the pennies stuck in the rectum.
This cat has IBD, as evidenced in this case by the thickened small intestines at the arrow. This can also be a normal finding, and it can also be a sign of intestinal cancer. The more common intestinal cancers are lymphoma, adenocarcinoma, and mast cell tumors.
Prior to the common use of ultrasonography, barium contrast studies were performed in order to reveal disruptions of the mucosal surface along the gastrointestinal tract. We are looking for filling defects and ulcers of the mucosa and thickening.
Barium has lost some of its significance since ultrasonography tends to be much more sensitive. One very nice “side effect” of giving barium to a pet that might be vomiting is its soothing affect on the lining of the intestines (mucosa) to stop the vomiting.
TLI type tests- serum fPLI (pancreatitis), fasting serum TLI (exocrine pancreatic insufficiency), fasting serum cobalamin and folate (small intestinal function and bacterial overgrowth). These are specialized tests and take several days for the results to come back.
Endoscopy is a useful tool since we can observe the lining of the esophagus, stomach, and duodenum for ulcers, lesions, and foreign bodies, that might not show up on a radiograph. Biopsy samples can be taken, although they are not full thickness, and only take the lining of the small intestines. This can lead to an inaccurate diagnosis.
This is a report from a stomach and intestinal biopsy with the endoscope
The most accurate way to diagnose IBD is to perform an exploratory surgery and take full thickness intestinal biopsy samples. If the blood protein level is low (hypoproteinemia) care must be taken because healing can be delayed.
Samples obtained during surgery are analyzed by a pathologist to help confirm a diagnosis of IBD, and also rule in or rule out the possibility of intestinal cancer. Sometimes the pathologist cannot tell the difference between IBD and cancer due to the abundance of inflammatory cells.
During surgery, samples of other important organs like the liver and lymph nodes can also be obtained. These samples are very informative, and are taken in many cases.
Surgery has the major advantage of being able to see and palpate the intestines, along with taking a complete (called full thickness) sample of the intestines. This surgeon is using a scalpel blade to take the sample.
These samples are analyzed by a histopathologist. The report might come back with several different terms describing the IBD in specific medical terms, depending on the cell type:
Lymphocytic-plasmacyltic (the most common one)- respond best to diet change, antibiotics, and immunosuppressive drugs.
Eosinophilic (2nd most common)- respond best to worming medication, diet change, and sometimes immunosuppressive drugs
Neutrophilic- bacteria is a possible cause, so culture and antibiotics, with no immunosuppressive works best
Granulomatous- least common, suggests fungal or intra-cellular pathogen
Ultrasonography of the abdomen is an invaluable diagnostic tool. Ours are performed by an experienced radiologist always when we we suspect IBD. It takes their type of training and experience to make this diagnosis.
Prior to the advent of ultrasound, exploratory surgery was needed to make an accurate diagnosis, and that was only after biopsy samples were obtained. Our ultrasound page has more.
Ultrasound is dramatically less invasive and expensive compared to surgery, and the results are obtained immediately in many cases. In the case of IBD it can tell us of thickening of the intestines and gives us a suspicion that IBD is indeed present, but it cannot confirm the diagnosis.
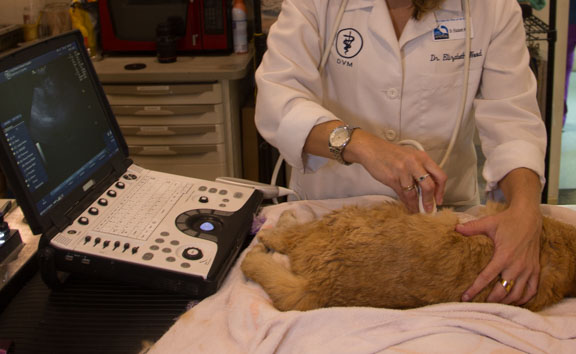
Ultrasound is rapid and painless, and the only invasive part is shaving your pet’s abdomen
This is a typical report of a pet with IBD. Note how detailed it is, and how organ size is measured.
Ultrasound can be used to measure wall thickness of various segments of the intestinal tract, which yields supportive evidence in the face of clinical signs. However, it cannot be used to differentiate between IBD and other disease processes that result in significant inflammation of the intestinal wall (i.e. lymphoma). This is where surgery has an advantage since full thickness biopsy samples can be taken for analysis
This is what the small intestines look like during ultrasound while they are being measure for size
This is what the pancreas looks like, also being measured
All of the abdominal organs are assessed during an ultrasound. This is what an enlarged abdominal lymph node looks like.
Ultrasound is a big aid in the diagnosis of IBD in its ability to to rule out cancer and foreign bodies as a cause of vomiting. It also gives us an accurate way to biopsy internal organs like lymph nodes and the liver.
Our surgeon is preparing to biopsy the mesenteric lymph node
This is how we biopsy the liver during surgery
Fine needle aspirate samples may be obtained with the guidance of ultrasonography. Sometimes this test is diagnostic, sometimes it is not. Even though it is not a perfect test, we sometimes recommend it due to the simplicity in obtaining it.
A hypoallergenic diet trial may be issued for cases of highly suspected dietary allergies or intolerance. In such cases, some pets respond when the diet is altered and no further diagnostics are necessary. You must feed this food, and only this food, to see if this works. Sometimes results are immediate, other times it might take several months to know for sure.
This can be a risk if the diet trial is attempted before numerous other disease processes are not first ruled out, especially cancer and internal organ diseases like Feline Hyperthyroidism. This delay in diagnosis can affect outcome. If clinical signs do not improve or resolve within the first two weeks of the diet trial, then further diagnostic work-up is indicated.
Treatment
Depending on the severity of disease at presentation, treatment must first begin with stabilizing the pet. What we do to stabilize depends on the severity and duration of symptoms.
Symptomatic
Stabilization generally includes intravenous fluids to correct dehydration, correct electrolyte imbalance, and improve kidney function. If the protein level is low we might use a fluid called Hetastarch.
Pets that are not eating are assist fed a special diet called A/D to maintain appropriate caloric intake and to prevent further disruption of internal organ function and get the GI tract back to normal. Probiotics to help stimulate the normal bacterial flora might be beneficial.
Vomiting pets are continued on fluids to maintain normal hydration, and given a specific medication called Cerenia® (maropitant) to stop the vomiting. This drug has been a tremendous help in alleviating vomiting in pets due to many different causes.
We use it for IBD and also for other GI problems like parvo virus and pancreatitis without IBD. Cerenia works on the emetic (vomiting) center of the brain.
We use the injectable version in the hospital, and send home an oral version if needed
Diet
It must be understood that if one of our doctors recommends a dietary change to treat your pet’s IBD that the only food or treat that can be fed to your pet is this new diet. Nothing else can be used as a food source. Feeding other foods is a reason why this dietary change does not work in some cases. When multiple people feed a pet this needs to be communicated to everyone.
Dietary intervention is considered a mainstay for many gastrointestinal cases because a large proportion of cats and dogs with gastrointestinal disease are associated with food-sensitivity. We need to get these pets eating again for the intestines to return to normal function.
Dogs and cats with pancreatitis, which is painful and causes severe illness, do well initially with a low fat diet in the early stages to get them stronger and get the intestines used to digesting food again. I/D (Intestinal Diet) has been used by our doctors for well over 35 years, and is the gold standard for pets with GI problems. After the pet is stable we look for a long term food.
Every pet food manufacturer has some magic food it claims will cure your pet’s GI problem. Please read our Nutrition Page to understand what is going on much better, and why the groomer, breeder, or person at the pet store has no business giving dietary advice to you.
I/D comes in many variations, and our doctors will tell you which one is appropriate for your pet’s specific problem
Once we get your pet eating again without vomiting or diarrhea with I/D we sometimes change to a hydrolyzed protein diet called Z/D. It is the most common diet fed for pets with IBD, and can be tried first before I/D in some cases.
It is the protein component of the food that causes the problem in IBD. Hill’s has solved this problem by making a food with a hydrolyzed protein that does not cause a reaction. It is unconditionally guaranteed, and is worth using in every case because it works often, and you can get your money back if it does not work.
This is a complete diet and can be fed for the rest of your pet’s life. It is very rewarding when a dog or cat with the signs of IBD improves on only food and does not need medication.
The best food we have found overall for dogs and cats with food allergy is called Z/D
Novel proteins are not manipulated protein sources (as compared to hydrolyzed proteins like Z/D), but are simply new proteins that the pet has never ingested before. Many dogs and cats immune systems have not been exposed to venison, duck, or rabbit.
Due to the fact that it takes long-term exposure to a protein before the immune system will react against it, then these novel protein diets are often attempted when the protein source is suspected to be the cause of IBD. The new diet will take at least 2 weeks, and up to 4 weeks, for the symptoms to diminish or resolve.
These foods might contain:
Potato
Duck
Sweet potato
Venison
Salmon
Vitamin supplementation is a critical component of treatment for some individual pets whose IBD stems from a deficiency in cobalamin (vitamin B12), specifically in cats. Pets that are sick enough to have a low cobalamin level are generally in need of more than just vitamin supplementation, requiring a combination of other medications and dietary alterations.
Immune Modulators
Steroids (corticosteroids) are used in many cases in order to decrease the inflammation. This is because they work, and with cats especially, are tolerated well. If we use just one medication to treat your cat for IBD it will most likely be a steroid called prednisolone.
The most common ones include prednisolone or prednisone. Budesonide, is a weaker steroid, that is also used. If the root of IBD or Triaditis is due to an immune-mediated process, then more potent immune system suppressants than steroids are required, such as cyclosporine, chlorambucil, or azathioprine.
Cyclosporine is an immune modulation drug that can suppress the inflammation from IBD.
Chlorambucil (Leukeran) is a chemotherapy drug for treatment of resistant IBD or some forms of cancer
Antibiotics
Antibiotics should be chosen based on bacterial culture and susceptibility when possible, especially in cases of Triaditis. Antibiotics such as Flagyl (metronidazole) are very commonly used for their ability to treat patients with chronic diarrhea.
Some pets respond well to this medication only (they have Antibiotic Responsive Enteropathies). Flagyl suppresses the bacteria that are involved with IBD, and also mildly decreases the immune response that is an important component of IBD. Other antibiotics include Tylosin, Amoxicillin, and Fluoroquinolone’s. Tylosin must be compounded.
Probiotics and Probiotics
These are commonly used to help with the trillions of beneficial bacteria in the GI tract. IBD disrupts these “good” bacteria, and even the antibiotics we use to treat IBD can disrupt the normal GI flora. Make sure there is not a chicken or beef base.
Probiotics have bacteria that are considered to be beneficial to the GI tract. Probiotics have fiber that is fermented for good bacteria.
Liver Support Medication
When the liver is involved (Triaditis) we might also use Actigall (ursodiol) or Denamarin (s-adenosyl methionine)
Denamarin helps support liver function
Stem Cells
Limited studies show promising results
Fecal Transplant
A last resort that can be effective. The feces must be negative for pathogens.
Prognosis
The prognosis depends on many factors. This disease is usually not cured, unless there is a food allergy and we find the right diet for your pet.
Most cases are controlled with diet and medication. IBD and it’s associated diseases tend to be a long-term problem that is usually managed successfully. You increase your chance of success by giving medication consistently and bringing your pet to us for exams and diagnostic tests to look for changes that require a change in treatment.