One of the most important tools available to veterinarians to thoroughly and painlessly treat pets is the advent of modern day anesthetics. These anesthetic agents allow us to sedate and anesthetize a wide variety of animals with negligible chance of serious side effects. In addition to sedating them for surgery, these anesthetics enable smooth and pain-free recovery.
We work closely with the American Animal Hospital Association and their guidelines for anesthesia.
The doctors at the Long Beach Animal and emergency hospital have been successfully anesthetizing a wide variety of exotic and domestic animals since 1989. If your pet requires anesthesia one of our veterinarians will make a custom plan tailored to your pet’s specific situation.
Here are a few of the many different species of differing sizes and anatomies we can safely anesthetize:
- Canine (dog)
- Feline (cat)
- Avian (bird)
- Guinea Pig
- Pot bellied pig
- Reptile (herp)
- Snake
- Tortoise
- Turtle
- Lizard
- Iguana
- Chameleon
- Ferret
- Rabbit (lagomorph)
- Wildlife
- Zoo animals
- Rodents
Modern anesthetics allows us to safely anesthetize high risk animals like this duck with a fractured wing. You can see her surgery in our Wildlife Care page.
The lack of significant complications from anesthesia is due to a combination of expertise, thorough pre-anesthetic testing, and state of the art anesthetic and monitoring equipment. We are equipped to anesthetize any pet from a finch that weighs 15 grams (it takes 454 grams to make up one pound), to pets that weigh several hundred pounds.
We are also particularly proficient in anesthetizing senior pets and pets with medical problems like liver and kidney disease.
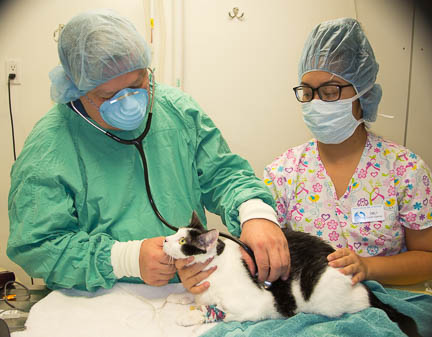
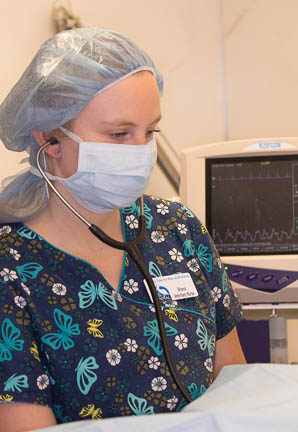
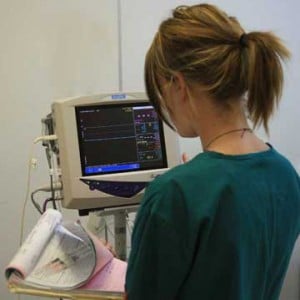
The most important part of monitoring your pet while it is under anesthesia is our nurse anesthetist technician. She is with your pet the whole time it is under anesthesia
The goals of anesthesia are to minimize anxiety and eliminate pain. In addition, from the surgical point of view, anesthesia allows profound muscle relaxation. This is helpful in every surgery because the procedure will go quicker and incisions can be made smaller when the muscles are relaxed. In certain types of surgery like fracture repair, this muscle relaxation is crucial for success.
It is normal for you to have concern if your pet is about to undergo a procedure that requires anesthesia. Because of this fact, we invite you to be a part of our anesthetic team. Your primary responsibility is to let us know of your concern. You will have access to your doctor to discuss any of your concerns and to set up a custom protocol for your pet, taking its specific needs into consideration.
Only when you are comfortable with the situation will we proceed any further. Also, to alleviate your concern on the day of actual anesthesia, we will call you immediately after your pet wakes up, if you so desire. Please leave a number where we can reach you on the day of surgery.
Pre-Anesthesia
A pre-anesthetic exam is performed just prior to anesthetizing any animal. We are looking for any problems, particularly with the heart and lungs.
We perform this exam just prior to anesthetizing your pet
Our more unusual patients also get an exam prior to surgery
Even our scaley friends get exams prior to anesthesia
One of the precautions we take to minimize the risk of anesthesia is to perform pre-anesthetic diagnostic tests. A pet can pass its pre anesthetic physical exam and still have significant internal problems, so it is important that we perform more than just a physical exam.
This is because animals cannot tell us of their problems, have high pain thresholds in comparison to people, and have defensive mechanisms allowing them to hide symptoms. Pre-anesthetic diagnostic tests are designed to alert us to internal problems that are occurring without any symptoms.
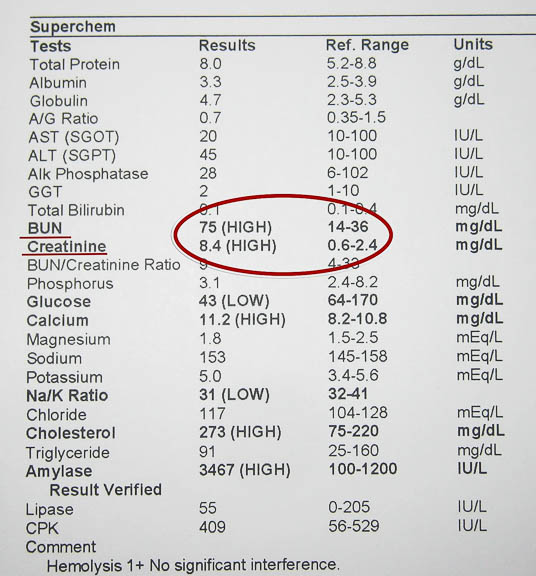
We prefer to perform an exam and blood panel about one week prior to surgery. We send this blood panel out to our lab for a thorough analysis of important organs like red blood cells, liver, and kidney and the immune system.
This report is showing a kidney problem
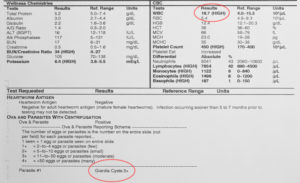
In an emergency, or when we cannot send the blood out to our lab several days prior to surgery, we can perform an analysis in our hospital by our blood analyzer
We can have this report in 30 minutes. This is how it checks the CBC (Complete Blood Count). It also gives us a biochemical report like the one above that checks the internal organs like the kidneys.
Those pets that have infections (especially tooth infections) might be put on antibiotics ahead of time. They make pets feel better, and help support internal organs.
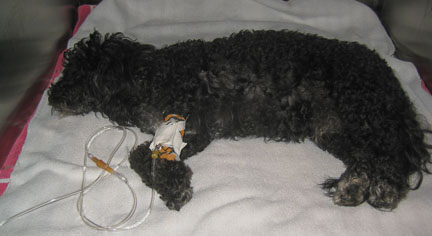
Older pets, or those with medical problem,s are given intravenous (IV) fluids prior to and during the anesthetic procedure. Giving fluids prior to the surgery greatly reduces anesthetic risk.
This is particularly important in older pets and those with kidney or liver disease. Most pets that have significant dental disease will also be given IV fluids.
IV fluids are one of the most important treatment modalities we have for a wide variety of medical situations in addition to surgery
Pre-Anesthetic ECG
For elderly pets, those with heart murmurs or heart conditions, we perform an electrocardiogram just prior too surgery.
This one has a potential problem that needs to be addressed
Pre-anesthetic Radiographs
These are extremely valuable in many cases since the gas anesthetic we use affects the heart and lungs. If we hear a problem with our stethoscope, if a pet has any breathing problem or coughing, if the blood panel shows a problem, or the pet is elderly.
Sometimes we find problems that we or an owner was not aware of at all. The radiograph below is a case in point. Compare it to the normal radiograph below it to see the dramatic difference on a pet that did not have any problems.
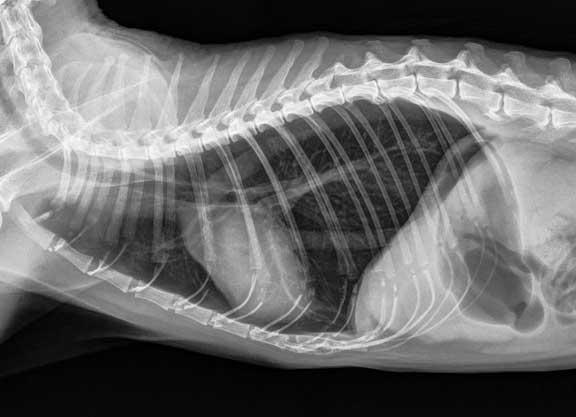
The cat has a serious problem called a diaphragmatic hernia. In this case the intestinal contents have ruptured through the diaphragm and entered into the chest cavity. This pet would be a major anesthetic risk, and we are glad we found out about it ahead of time.
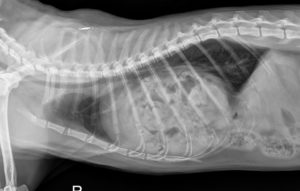
This is what a diaphragmatic hernia looks like on a thoracic radiograph of a cat. It is that large rounded area in the center of the chest. You can even see the gas (the dark areas in the rounded area) that indicate intestines. We did not know this until we took the radiograph.
The heart is the oblong white object in the center. You can see the aorta, lungs, bronchi, and lungs in this normal radiograph.
If you don’t understand the structures in the above radiograph you can learn to read a radiograph at this link.
Echocardiogram
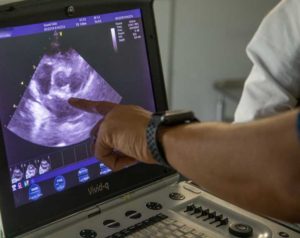
If a pet has a heart murmur, or we suspect any type of heart disease, an echocardiogram is the gold standard in determining if this pet can be anesthetized. This highly sophisticated tool gives us a detailed look at the heart to determine its ability to pump blood to the rest of the body.
Our cardiologist Dr. Fred Brewer is assessing the blood flow through the heart valves in between the chambers of the heart in this pet
Blood Transfusions
For those pets that are anemic, or in surgeries where we anticipate significant blood less, we give whole blood before, during, and after the surgery. This is important in surgeries like splenectomies.
This is what anemia looks like in a CBC from our in house blood machine
Dog do not have iso antibodies, so in an emergency, and if the dog has never received blood before, we can give blood from most any dog donor. It is not our preferred way of doing a blood transfusion.
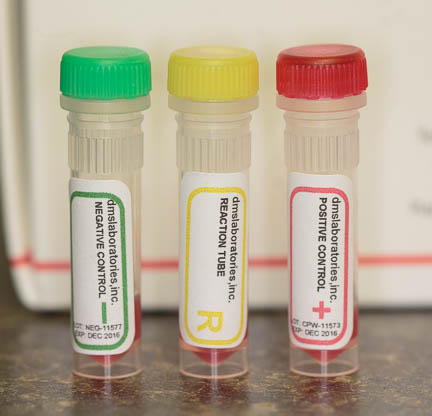
Before we give the blood we prefer to do a cross match
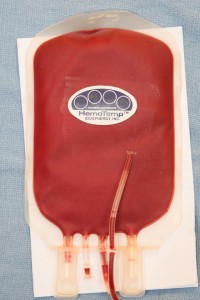
We use whole blood that is specially prepared and stored
Injectable Anesthesia
Injectable anesthetics are used for many purposes. One of their primary uses is to sedate pets before giving the actual anesthesia (called pre-anesthetic). In sedating ahead of time we dramatically minimize anxiety, cause a smoother recovery, and minimize how much anesthetic we need to administer during the actual procedure. In addition, some injectable anesthetics minimize vomiting, a common problem when waking up from anesthesia.
Injectable anesthesia is given intravenously, and rapidly induces relaxation so that we can put in a breathing tube
Injectable anesthetics are also used to give complete anesthesia for short periods of time. This is used for C-sections and minor surgical procedures. Injectable anesthetics are ideal to sedate a pet for radiographs (x-rays).
As new anesthetic agents evolve, the trend is towards using injectable anesthetics more and more for complete surgical anesthesia. They are very effective, very safe, and allow for rapid recovery from anesthesia. They also protect the environment because there are no anesthetic gases vented into the atmosphere.
Gas Anesthesia
The mainstay for general anesthesia is gas anesthesia because it is very safe and highly controllable. We use a safe and effective gas anesthesia called Isoflurane. It is so safe it can be used in creatures as small as tiny birds.
Lisa is watching carefully as this budgie is being anesthetized for a surgery to remove a growth on its cloaca
Gas anesthesia requires specialized equipment and training. Several precision components are used to administer and monitor anesthesia:
Oxygen
All pets put under gas anesthesia are given 100% oxygen from the moment they are anesthetized until they wake up, dramatically increasing the safety of the procedure.
We have a special machine in surgery that generates 100% oxygen
As a backup, oxygen is stored in large tanks under high pressure. The oxygen in these tanks is delivered to the anesthetic machine via special piping throughout the hospital. This allows us to have anesthetic machines in several hospital locations.
A pet can be brought into radiology after its surgery and still be kept under gas anesthesia, while the surgeon reviews post operative radiographs to ensure everything is in order. This is especially helpful when orthopedic surgery is performed.
Keeping a pet under anesthesia is important after orthopedic surgery to make sure the plates, pins, or screws are properly placed and in alignment. If they are not, any corrections can be made while still under anesthesia
Endotracheal Tube
Oxygen is routinely delivered to your pet by a breathing tube (endotracheal tube) in its windpipe. It is the preferred method to administer oxygen because it is very efficient, will prevent any vomitus from entering the trachea (vomiting rarely happens because of fasting and pre-anesthetic sedation), and allows us to gently inflate the lungs during surgery so that they work at maximum efficiency.
Besides oxygen, the anesthetic gas (Isoflurane) is also administered through the endotracheal tube. Medications can even be administered via this special tube.
The endotracheal (ET) tube is placed directly into the windpipe
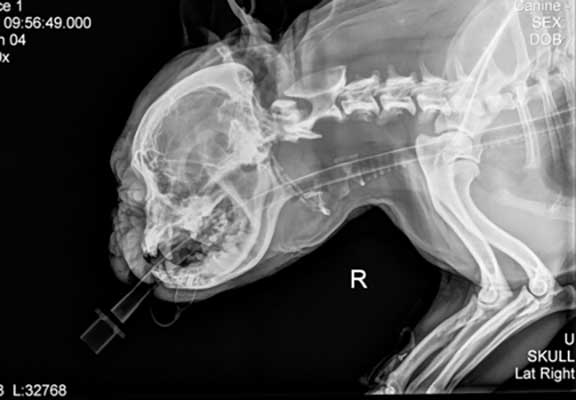
This x-ray shows the breathing tube as it passes over the tongue and down the trachea (windpipe)
We can easily breathe for your pet and inflate your pet’s lungs by gently squeezing the bag connected to the tube, monitoring the amount of pressure we are exerting with a gauge on the anesthetic machine. Each size and species of pet requires a different sized endotracheal tube.
The tube is not removed from your pet until it is literally waking up. This ensures that the swallowing reflex is present, and your pet is now safely able to breathe on its own.
Vaporizer
An instrument called a precision vaporizer is used to deliver the Isoflurane anesthetic gas within the oxygen. It is a very precise instrument allowing us to make fine adjustments in anesthetic level. Without this vaporizer we would not have the wide safety margin that we currently enjoy.
We can precisely and easily change the level of anesthesia during the procedure as needs change
For most surgeries we administer the anesthetic at a setting of 1-3 %. This small percent of anesthetic, added to the 100% oxygen the pet is breathing, is all that is needed to achieve complete surgical anesthesia. Before the surgical procedure is finished the anesthetic is lowered before it is turned off completely. As the surgeon is finishing the procedure your pet is in the beginning stages of waking up. This decreases anesthetic time, another way we minimize anesthetic risk.
Monitoring
Our surgeon is one of the best monitors, because he/she is literally visualizing the blood in the circulatory system. Any change in the blood is readily noticed because pets that are breathing 100% oxygen should have bright red blood.
In addition to all the high tech monitoring equipment we have, our anesthetist is hands-on in monitoring your pet. Here Brianna is using her stethoscope to check the heart, even though the heart monitor behind her is doing the same thing.
After listening to the heart she keeps a close tab on oxygen flow and the anesthetic level of our precision vaporizer
We keep detailed records of fluid rate rates, anesthetic and oxygen levels, and physiologic parameters, during the surgery
We keep a close tab on the heart with the stethoscope on all of our patients, including more unusual surgical patients
Since our small patients can easily become hypothermic due to the anesthesia and surgery, we monitor temperature continuously. This is especially important on the following species:
- Birds
- Ferrets
- Guinea Pigs
- Rabbits
- Rats
- Reptiles
You can learn more about surgery at this link on these species at this surgery link.
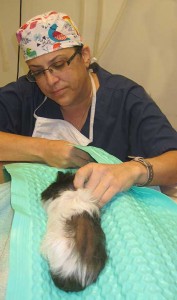
All of our patients, especially the smaller ones like this guinea pig, are kept on warm water water blankets to prevent hypothermia before during, and after any anesthetic procedure.
Anesthetic Monitor
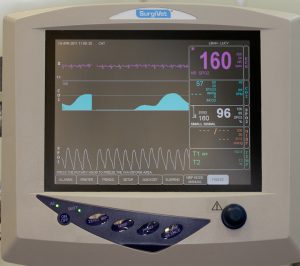
This highly accurate and sensitive monitor gives us detailed information on your pets physiologic status while under anesthesia.
It is a sophisticated instrument that gives us an early warning sign of impending problems with your pet’s physiology
It is calibrated prior to surgery to ensure accuracy
Watch it in action, and see if you an figure out what all these numbers mean
We sometimes use other instruments to monitor you pet while it is under anesthesia, even though the Surgical monitor does this also. It pays to be redundant. The two most important additional instruments we use are:
Pulse Oximeter (Pulse Ox)
The portable pulse oximeter is an instrument that measures the oxygen saturation of you pet’s red blood cells (to be more specific, its hemoglobin). It is an extremely sensitive instrument that gives us an indication of problems that may be arising long before your pet suffers any ill effects. In addition to measuring oxygen saturation, it measures heart rate, pulse character, and respiration.
This instrument does its magic by measuring the hemoglobin that is oxygenated, and comparing it to the hemoglobin that is not oxygenated. It does this by shining a light on an artery, and then measures how much of this light is absorbed. It gives us an answer in PaO2– the partial atmospheric pressure of oxygen.
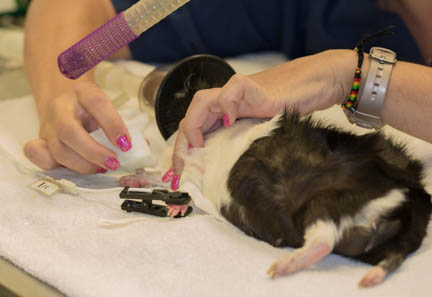
This Guinea Pig has the pulse oximeter sensor attached to his foot in preparation for surgery
The Pulse Oximeter measures oxygen saturation of 92% and a heart rate of 87 beats per minute (BPM). Both of these are normal on this pet, which is a pot bellied pig.
The pulse oximeter has several different types of sensors that can be attached in various locations depending on the procedure being performed.The pulse oximeter can also be used on pets that are not anesthetized. It is useful for pets that are having difficulty breathing (dyspnea) from many different causes.
It is also used to monitor pets that are in a state of shock. One of the most common reasons for pets to be presented to us in a state of shock is from trauma, especially being hit by a car (HBC).
Blood Pressure Monitor
We also monitor the blood pressure when pets are under anesthesia for the longer surgical procedures. This is done with our anesthetic monitor.
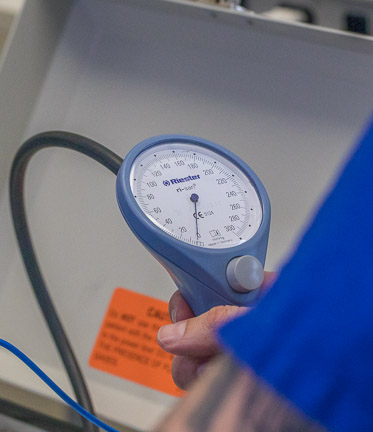
Blood pressure can also be checked manually at any time
Our hypertension page has a video of the doppler blood pressure monitor in action when we use it in an exam room.
Capillary Refill Time
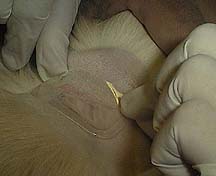
To complement these high tech methods of monitoring, our anesthetist technician uses several hands-on techniques as a backup. One of the easiest of these is called capillary refill time (CRT). By pressing on the mucous membranes in the mouth, and noting how long it takes for the blanched area to turn pink again, we get a basic assessment of your pets cardiovascular status.
A normal pet’s pink color returns within 2 seconds. This technique is used in other situations besides anesthetic monitoring. It is especially helpful when a pet is in shock or is dehydrated. It is also can help us with an anemic pet.
Capillary refill time on this pet is less than one second
Pain Medication
We complete the anesthetic process by giving your pet a pain injection before it wakes up from the anesthetic. Since the gas anesthesia has a small amount of residual analgesia (ability to kill pain), the pain shot kicks in as the gas anesthetic is wearing off. This allows for a very smooth and pain free recovery.
We monitor this closely, and will give additional injections as needed. This pain injection will keep your pet calm its first night home from any surgery. We will also send you home with oral pain medication also for several days.
Local Anesthesia
Another excellent way to prevent the pain encountered when your pet first wakes up is to use a long acting local anesthetic at the incision site. We administer it prior to completion of the surgery so it is in full effect when your pet wakes up.
We use the long acting version of this drug which eliminates pain for up to 8 hours
We even have a local anesthesia patch that is used in some cases to bring long term relief for several days if needed.
Pain Patch
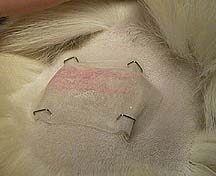
We also use Duragesic (Fentanyl) patches for general pain control in the more serious cases. It is preferable to apply it 12 hours before the surgery for maximum effect postoperatively. It provides pain relief for 3 days. It is important to make sure that no children or other pets are allowed to contact the patch in any way. Bring your pet back to us for proper removal and disposal.
The patch is applied in different locations depending on the surgery. Wrapped around one of the legs and between the shoulder blades are common locations. If we put it on the leg it is covered with a bandage. It will be bandaged for protection and to minimize the chance of contact with other pets and children. Please return in 3 days for us to remove it and dispose of it properly.
One of our nurses is applying it in this picture using gloves to ensure she does not come into contact with the active ingredient.
We will commonly staple the patch to the skin if we put it between the shoulder blades
Our surgical patients are monitored closely immediately after surgery. We will verify the pain medication is working, and that there are no ill effects from the anesthetic. It will also allow your pet to completely wake up and walk normally in a controlled environment where it cannot hurt itself.
Our technical staff monitors your pet post operatively until we are certain it is ready to go home
Long term pain control at home is also important during the next several days. We will routinely send you home with an anti-inflammatory medication or pain suspension for long term pain control. The two most common medications we use are Rimadyl and buprenorphine (Brprenex). We also use Onsior in cats for up to three days of pain control.
Laser Surgery
Even though it is not an actual pain medication, using our carbon dioxide laser when indicated during a surgical procedure dramatically minimizes pain because it decreases inflammation, swelling, and cauterizes nerve endings. By using the laser and stopping the pain cascade before it even begins there is a dramatic influence on decreasing post operative pain.
This video shows you how we calibrate and set the laser for a neuter surgery
Companion (also called Therapy) Laser Post Op
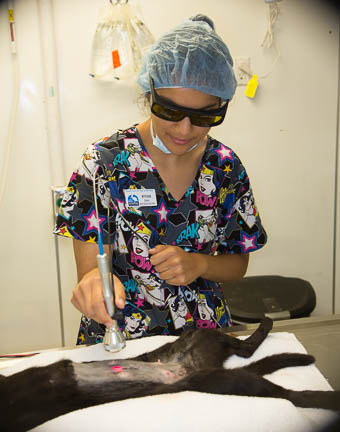
For additional pain control we use our Companion Laser on the incision line before your pet wakes up from anesthesia. This decreases post operative swelling and pain, and makes your pet much more comfortable.
You get to wear cool glasses when we use this laser
Watch it in action
Returning Home after anesthesia
When you bring your pet home after anesthesia it is helpful to follow some common sense suggestions:
- Keep contact with other pets and children to a minimum for at least the first 12 hours. Confine it to an area where it cannot hurt itself because it may not be steady on its feet for up to 24 hours. It might be groggy the first night due to the pain injection it was given.
- Use pain medication as prescribed and keep your pet in a warm and quiet area. Use pain medication until it is gone. You can spend time giving unlimited TLC
- Even though your pet has probably been fasted for the anesthesia, feed it only a small amount of food and water when first returning home. Give it more later if it eats well and does not vomit (emesis). Most pets return to a normal appetite within 24 hours. If your pet has not fully recovered from the anesthetic by the next day then please call our office.
- Please call us in the evening if you have any questions when your pet returns home from surgery or any anesthetic procedure.
Anesthesia is used in many emergencies. Our animal hospital with emergency vets is available until the evenings 7 days per week to help you if you see this in your pet, so please do not wait or attempt to take care of this problem on your own. If you have an emergency always call us first(562-434-9966) before coming in so that can advise you on what to do at home and so that we can prepare. To learn more please read our Emergency Services page.
To learn much more about how we do surgery at the Long Beach Animal Hospital please visit our Surgery Page and our Diseases Page. You can see photos and videos of actual surgeries on these pages.